Johns Hopkins Experts Tout mRNA Vaccines' Safety, Future Beyond COVID-19
mRNA vaccines proven safe through COVID-19 could soon target cancer and flu; Hopkins scientists made the case for sustained funding to keep the U.S. ahead.
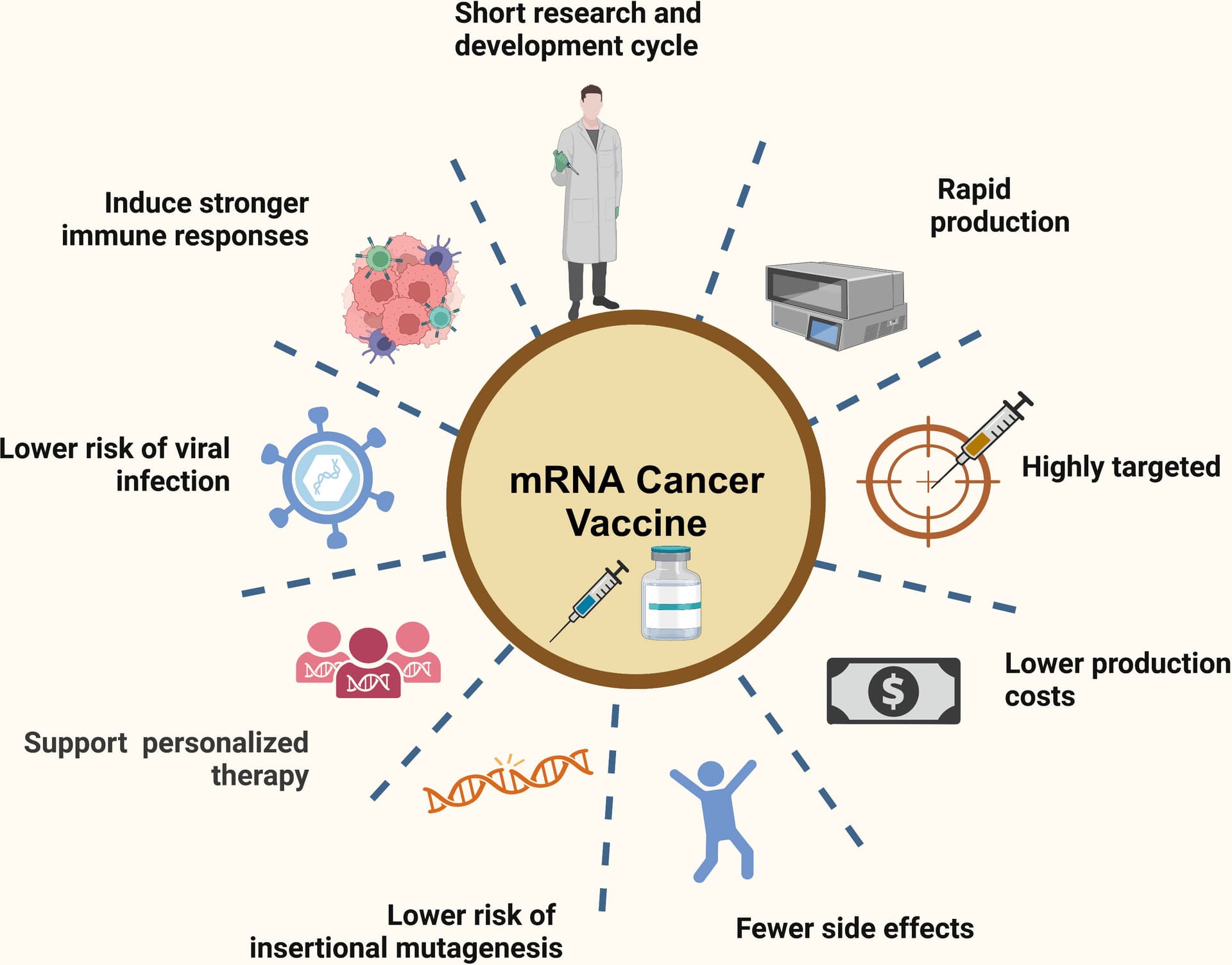
The mRNA technology that protected millions from COVID-19 could soon be deployed against cancer, faster seasonal flu strains, and emerging pathogens not yet on the radar of public health officials. That was the central argument from researchers at the Johns Hopkins Bloomberg School of Public Health, who convened a media briefing last Thursday to make the scientific and policy case for sustained investment in mRNA platforms.
The March 26 briefing featured Hopkins faculty and scientists who outlined the mechanics of mRNA vaccines, their established safety record from global COVID-19 rollouts, and the speed with which the platforms can be adapted to new biological targets. Researchers also addressed persistent public misconceptions, including unfounded concerns about fertility effects that have circulated since the pandemic's early days.
Beyond myth-busting, the briefing pushed into less-charted territory: flu vaccines that could be reformulated faster than current egg-based production methods allow; cancer treatments built on personalized mRNA sequences tailored to an individual patient's tumor profile; and rapid-response vaccines for pathogens that haven't emerged yet. Experts framed the technology's flexibility as its defining asset, one that makes mRNA not just a pandemic tool but a platform with decades of potential applications.
Hopkins researchers argued that realizing those applications requires consistent federal and philanthropic funding. Without steady financing, they cautioned, academic and translational research timelines stall, and the United States risks ceding ground in a field where it currently leads. The briefing's full recording and transcript were released publicly, giving journalists and policymakers direct access to the primary-source arguments.

Baltimore's stake in that funding debate is concrete. Johns Hopkins anchors both the city's health care economy and its identity as a national biomedical research hub, meaning federal decisions about mRNA research budgets ripple directly through local hiring, clinical trial activity, and partnership opportunities with regional health systems and manufacturers.
Grant announcements and pilot programs arising from Hopkins' work, particularly any tied to Baltimore-based clinical trial sites or local health systems, will signal how much of that promise translates from the lecture hall to the lab.
Know something we missed? Have a correction or additional information?
Submit a Tip

