Perham woman carries sister’s cancer advocacy legacy into statewide fight
Lisa Roberts is carrying Robianne Schultz’s fight from Perham to the Capitol, and free screenings could keep rural families from putting off cancer care.
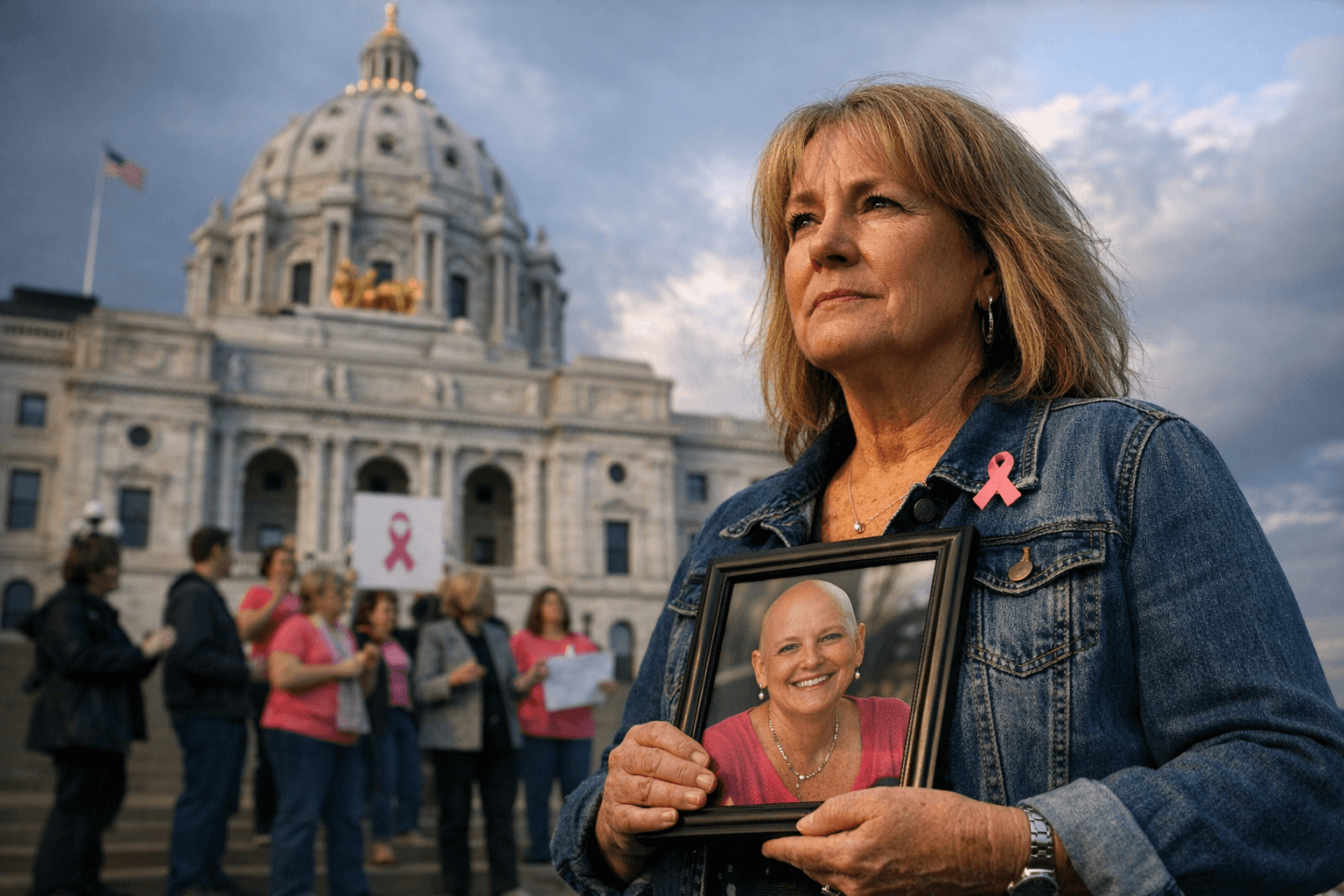
A free screening can change the odds in rural Otter Tail County
In rural Perham and across Otter Tail County, a mammogram or cervical screening can be more than a routine appointment. For people who delay care because of cost, long drives or gaps in insurance, Minnesota’s Sage Screening Program can be the difference between catching cancer early and waiting until symptoms force a harder path. The Minnesota Department of Health says Sage has participating providers at more than 450 locations across Minnesota, a reach that matters in places where access is measured in miles as much as minutes.
What Sage covers, and who can use it
Sage offers free breast and cervical cancer screenings at participating sites for eligible Minnesotans. The program can cover an office visit, a mammogram, cervical screening such as Pap and HPV testing, and follow-up visits and diagnostic services if a screening comes back abnormal. That full chain of care matters because a screening is only useful if people can also get the next test without a financial shock.
Eligibility is based on age, insurance status and income. As of January 1, 2026, a household of one must have yearly income at or below $39,900, and a household of two at or below $54,100, with higher limits for larger households. In practical terms, Sage is aimed at Minnesotans who might otherwise skip care because even a routine appointment can become unaffordable.
Minnesota law adds another layer of protection. State statute 62A.30 requires many health plans covering Minnesota residents to provide coverage for routine cancer screening procedures and the office or facility visit, including mammograms, Pap smears, colorectal screening tests and certain ovarian cancer surveillance tests. That rule helps, but it does not erase the problem of uninsured or underinsured residents, or the gap between a covered test and the follow-up care a suspicious result can trigger.
- Office visit
- Mammogram
- Pap and HPV cervical screening
- Follow-up visits
- Diagnostic services after an abnormal result
How the federal safety net fits in
The CDC says the National Breast and Cervical Cancer Early Detection Program serves women who are uninsured or underinsured and have incomes at or below 250% of the federal poverty level. It generally serves women ages 40 to 64 for breast cancer screening and 21 to 64 for cervical cancer screening, though some younger or older women may qualify. That federal program helps explain why screening access remains a public-health issue, not just a private medical decision.
For families in Otter Tail County, the practical question is not abstract policy. It is whether a person can get screened before a lump, an abnormal Pap result or a delayed follow-up turns into a much more serious diagnosis. Sage’s statewide footprint, along with federal screening support, is designed to answer that question before cost and distance close the door.
How Robianne Schultz’s legacy still shapes the fight
Robianne Schultz spent much of her adult life pushing lawmakers at the State Capitol and the U.S. Capitol for cancer research funding because she wanted people fighting the disease to have a better chance of surviving. A 2017 CBS Minnesota report said Schultz was diagnosed with breast cancer at 27, fought the disease for 16 years and died on Nov. 22, 2017, at age 43. The same report said she served as Minnesota’s lead ambassador for the American Cancer Society Cancer Action Network and regularly traveled to both capitols to testify and train other volunteers.
That legacy now runs through her sister, Lisa Roberts, who has carried the work forward from her home base in rural Perham. In a county where families often know the cost of waiting too long for care, Roberts’ role gives the fight a local face and a local address. What began as one woman’s cancer battle became a family mission, and that mission now keeps the focus on what early detection can do when people actually have access to it.
Schultz’s advocacy was never only about symbolism. It was about making sure patients did not have to choose between saving their life and saving their life savings. That message still resonates in a state where cost remains one of the biggest barriers to care, especially for residents outside the Twin Cities who may have to weigh travel, time off work and insurance gaps before they ever reach a clinic.
Why the policy fight still matters now
ACS CAN says nearly 40,000 Minnesotans will hear a cancer diagnosis in 2026, and it lists maintaining funding for the Sage Screening Program as one of its Minnesota legislative priorities. That estimate shows why screening policy is not a side issue. It is part of the front end of cancer care, where the difference between early and late detection can shape everything that follows.
The Minnesota Breast Cancer Coalition says it helped mobilize Minnesotans for four years to pass treatment coverage for women diagnosed through the federal screening program. It also says it has worked with NBCC to secure more than $3 billion in federal funding for peer-reviewed breast cancer research since 1992. Those figures show how a local family story in Perham connects to a much larger system of screening, treatment and research that reaches from Otter Tail County to Washington.
Roberts’ work keeps that system visible in a place where the stakes are personal. For rural families who might otherwise put off a mammogram, Pap test or follow-up appointment, a free screening can be the first real opening in a long time. In that sense, the fight she inherited is not only about memory. It is about making sure the next cancer diagnosis comes with a better chance of survival.
Sources:
Know something we missed? Have a correction or additional information?
Submit a Tip

