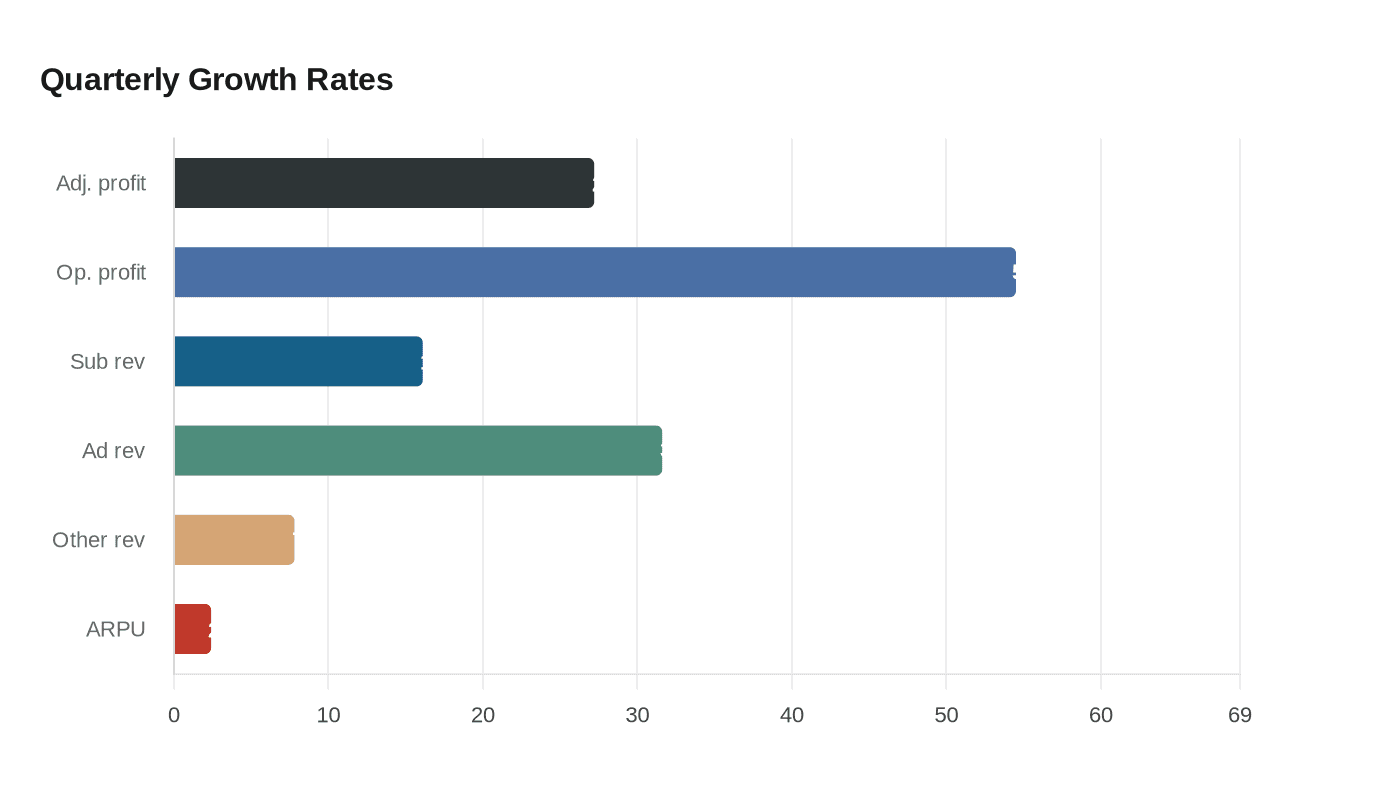CVS raises 2026 profit forecast after beating first-quarter estimates
CVS lifted its 2026 profit outlook after Aetna’s lower medical claims and a stronger pharmacy business, raising the question of efficiency or stricter care control.
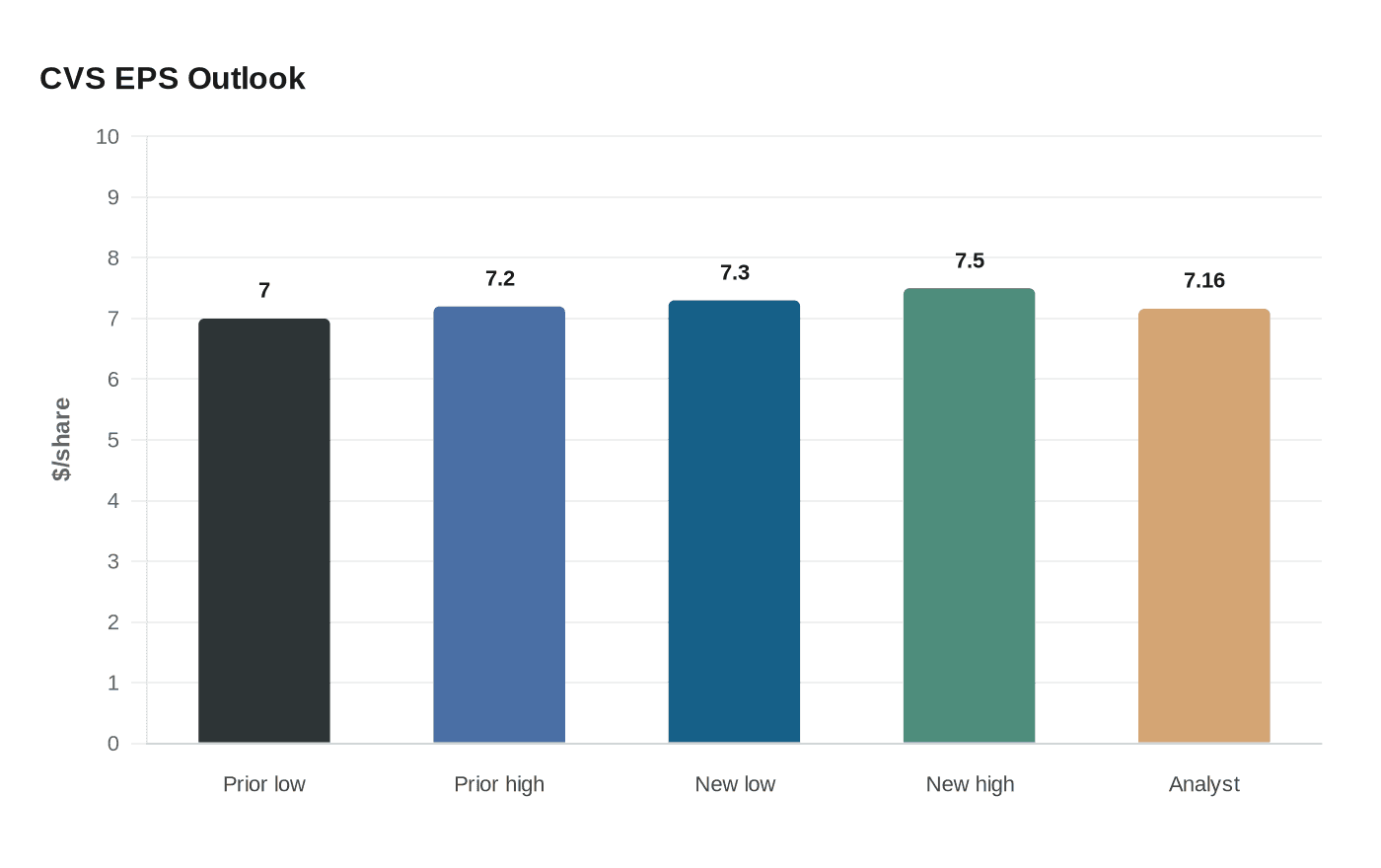
CVS Health raised its 2026 profit outlook after a first quarter that topped Wall Street expectations and showed tighter control of medical spending in its insurance business. The Woonsocket, Rhode Island, company now expects adjusted earnings of $7.30 to $7.50 a share, up from a prior range of $7.00 to $7.20, and above the $7.16 analysts had expected. It also increased its cash flow from operations forecast to at least $9.5 billion from at least $9.0 billion, a sign that management sees more room to fund the business as claims trends and pharmacy margins improve.
First-quarter adjusted profit came in at $2.57 a share, ahead of the $2.20 estimate, while revenue reached $100.4 billion. The biggest help came from lower medical claims in CVS’s government-sponsored health plans and a more favorable drug mix in CVS Caremark, the company’s pharmacy benefit manager. Aetna’s medical loss ratio was 84.6%, below the 87.58% analysts expected, meaning a smaller share of premiums went to medical claims than the market had modeled. CVS said the earnings gain reflected continued execution on the Health Care Benefits segment’s margin recovery plan.
That sets up the central question in CVS’s turnaround: is the company becoming more efficient, or simply more aggressive about restricting care costs? Aetna approved more than 95% of eligible prior authorizations within 24 hours in 2025, according to CVS’s investor materials, but lower claims costs and a better medical loss ratio can also reflect tighter utilization management. For patients and employers, the stakes are direct. Better cost control can help stabilize premiums and support pricing discipline, yet it can also mean more scrutiny before procedures, more pressure on pharmacy costs and more friction when access to care runs through prior authorization.
Brian Newman, CVS’s chief financial officer, said the company was improving its forecasting and that the cost trend “did not surprise me,” a sign of greater confidence in how the company is reading utilization and reimbursement patterns. CVS Pharmacy also completed a transition to cost-based reimbursement across its Commercial, Third-Party Discount, Medicare and Medicaid businesses, another move that should make margins more predictable but also underscores how closely the company is managing every dollar that flows through its retail and pharmacy network.
The update extends a stretch of steadier performance under David Joyner, who became president and chief executive officer on October 17, 2024, after replacing Karen Lynch. CVS said in December 2025 that it was targeting mid-teens adjusted EPS compound annual growth through 2028, and the latest guidance suggests that plan is still intact. With about 185 million consumers, more than 9,000 pharmacies and over 60 health plan clients, CVS sits at the center of U.S. health care spending, where every improvement in margins can also be a warning about how those savings were won.
Know something we missed? Have a correction or additional information?
Submit a Tip