Intermittent fasting shows little advantage over standard weight-loss diets
A Cochrane review finds intermittent fasting yields minimal extra weight loss versus other diets, prompting calls for clearer evidence and equitable obesity care.

A rigorous review of randomized trials found that intermittent fasting produces only minimal weight-loss benefits and does not reliably improve quality of life compared with other dietary approaches, challenging popular claims that timing alone is a superior strategy for obesity.
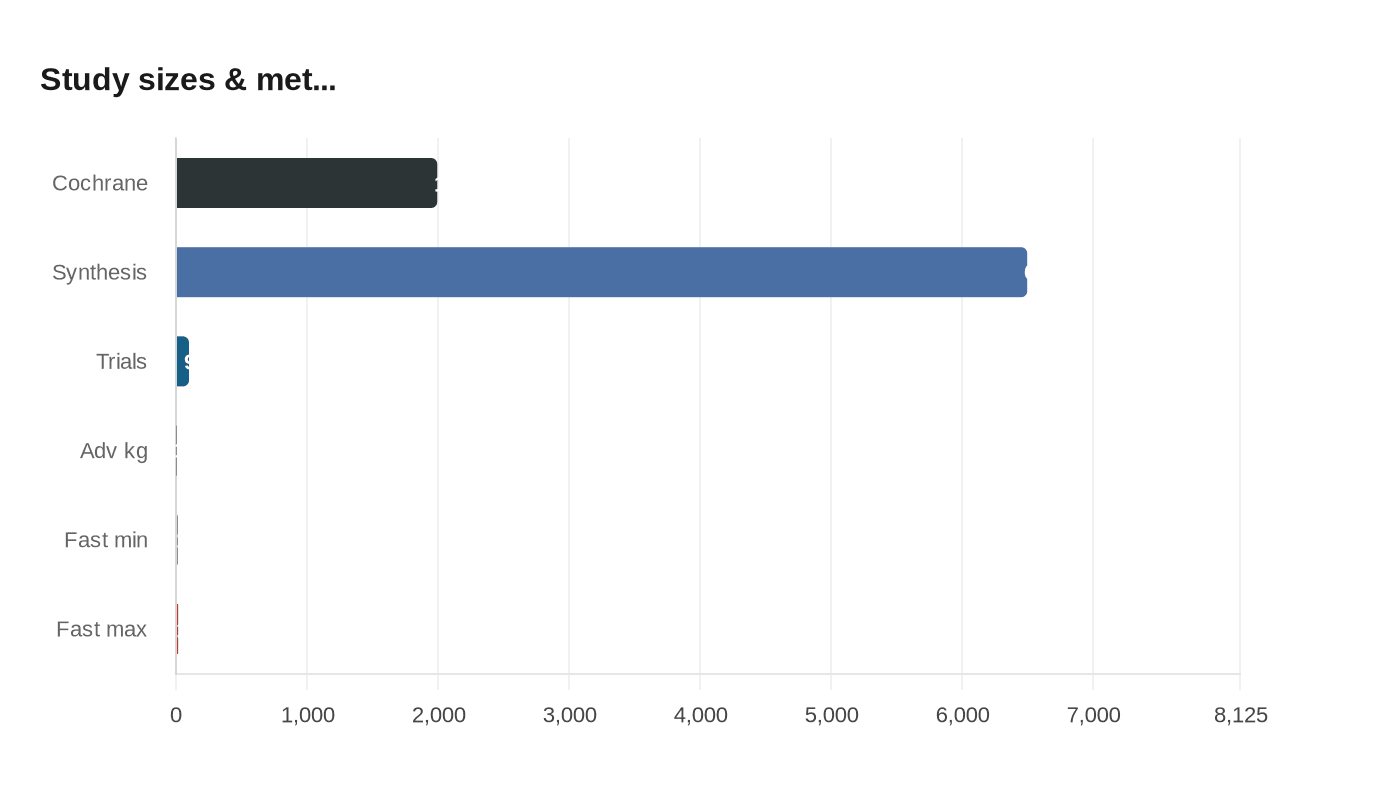
The Cochrane review pooled data from randomized clinical trials involving 1,995 adults across Europe, North America, China, Australia and South America and examined alternate-day fasting, the 5:2 diet and time-restricted eating. Its conclusion of limited benefit contrasts with a larger synthesis of 99 trials including more than 6,500 participants that concluded intermittent fasting and traditional calorie-restricted diets were broadly comparable, and that alternate-day fasting produced a modest advantage of about 1.3 kilograms and some improvements in waist circumference, lipids and C-reactive protein.
Researchers and clinicians say those different findings reflect variation in trial design rather than a single definitive verdict. There is no universal definition of intermittent fasting: studies vary by fasting duration, whether nonfasting days are ad libitum or calorie-limited, and whether exercise or other interventions are included. Time-restricted trials often target a 16-hour fast with an eight-hour eating window; reviews report that in practice many participants average about 15.8 to 16.8 hours of fasting. Dropout rates across trials ranged widely, from 0 to 65 percent, and adherence was not consistently better than with continuous calorie restriction.

"The benefits of intermittent fasting may be affected by timing, since the body's circadian rhythms are so deeply connected to metabolism. Studies in animals suggest fasting can change how fat reserves are used, improve insulin sensitivity - which is important for diabetes - and reduce inflammation and oxidative stress. It may also be good for ageing and longevity, she said, by triggering a process called autophagy, the body's recycling mechanism. One problem is that there is no universal definition of intermittent fasting, making it hard to understand its effects," said Dr Zhila Semnani-Azad of the National University of Singapore.
Other investigators highlight biological limits to short fasts. "Maik Pietzner, a professor of health data modelling at the Berlin Institute of Health at Charité, was surprised that weight loss from fasting was so small compared with doing nothing. But he said the finding fits with evidence that people are less physically active when fasting and that weight loss is hard without drugs." His work also suggests that short complete fasts of up to two days produce little change in blood markers, while a seven-day water-only fast showed widespread shifts in blood proteins only after three days.
Trials offer mixed evidence about exercise and fasting. A 2013 study of 64 obese patients reported that adding exercise to intermittent fasting roughly doubled weight loss, whereas a smaller 2019 trial of 31 participants found no exercise benefit. Mechanistic studies point to possible cardiometabolic gains from certain fasting patterns, but whether those translate into sustained health improvements across diverse populations remains unresolved.
For clinicians and policymakers the message is pragmatic: intermittent fasting is not a magic solution and calorie deficit remains central to weight loss. Guidelines caution that fasting is not appropriate for people under 18, those with eating-disorder histories, pregnant or breastfeeding people, and that people with diabetes should seek medical advice. Equity concerns are acute: communities facing food insecurity, limited time, or lack of clinical support may not benefit equally from time-focused diets, and policy responses should prioritize accessible, evidence-based obesity care and long-term studies that include underrepresented groups.
Researchers call for standardized definitions, longer trials and attention to timing, physical activity and social determinants so that recommendations reflect both biology and the realities of people's lives.
Sources:
Know something we missed? Have a correction or additional information?
Submit a Tip

