Trump administration withholds $1.3 billion in Medicaid funds from California
The Trump administration has frozen $1.3 billion in California Medicaid funds, the largest deferral in CMS history, as Medi-Cal faces fresh fraud scrutiny.
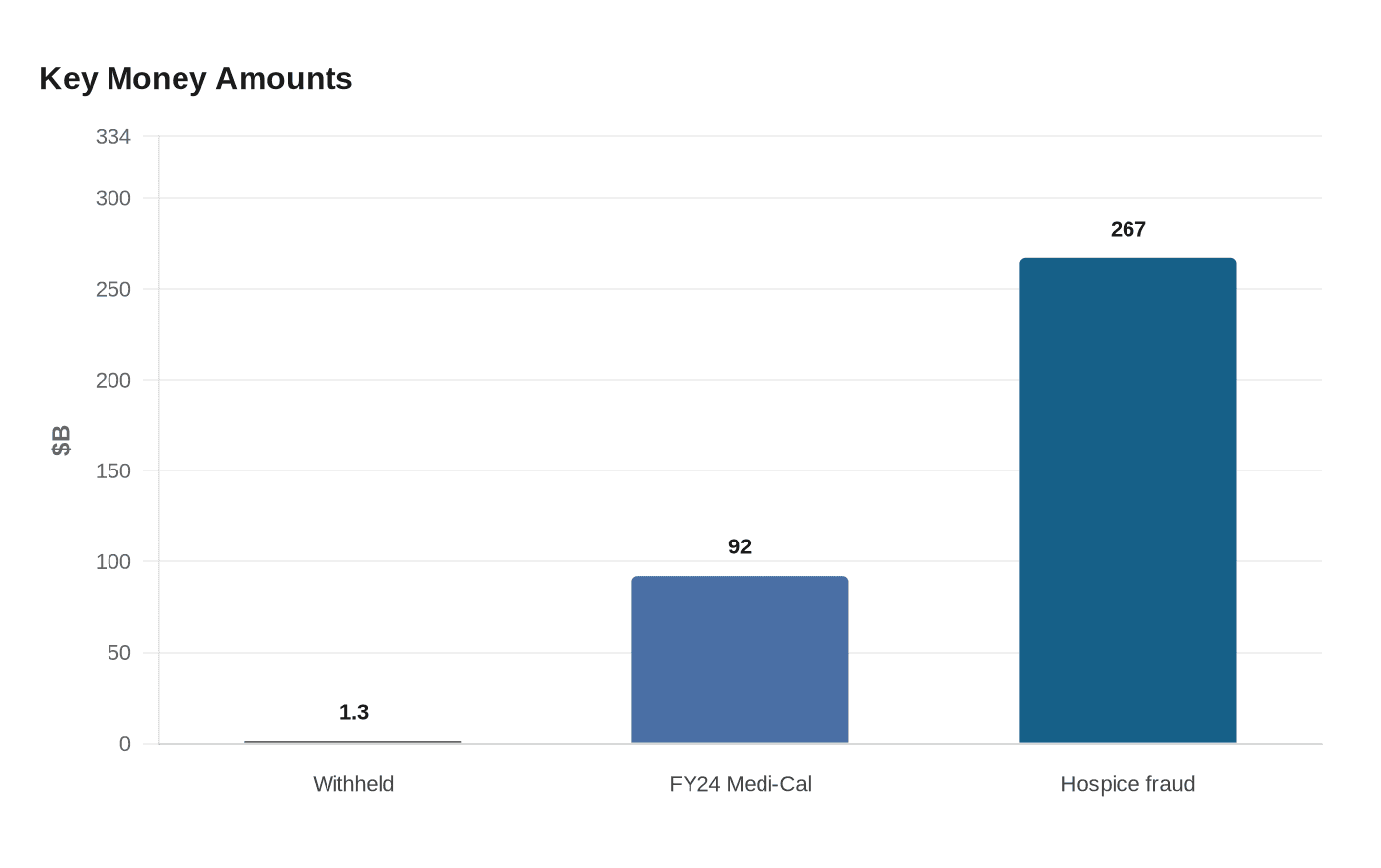
The Trump administration’s decision to withhold $1.3 billion in Medicaid reimbursements from California lands squarely on Medi-Cal, the state program that drew more than $92 billion in federal Medicaid reimbursements in fiscal 2024. CMS called the deferral its largest ever, and officials said the money would not be released unless California shows that eligible patients actually received services and explains what the agency described as questionable expenditures and anomalies.
Vice President JD Vance said California had not done enough to fight fraud in public health insurance, while CMS Administrator Mehmet Oz said the state’s Medicaid records had generated major red flags. The administration said the California move was part of a broader anti-fraud push that also included a six-month freeze on some new Medicare enrollments for hospice and home health agencies, along with warnings to all 50 states that Medicaid fraud control units could lose funding if they do not aggressively investigate and prosecute fraud.

For California, the immediate pressure is not the size of the deferral alone but what it could signal for future payments and oversight. CMS said the withheld amount is still a small share of the state’s total federal Medicaid funding, but the agency singled out faster growth in California’s home care program than in other states as one of the spending patterns it wants explained. California already has a Medi-Cal fraud hotline, and the state Department of Health Care Services says people can report fraud, waste or abuse anonymously at (800) 822-6222.
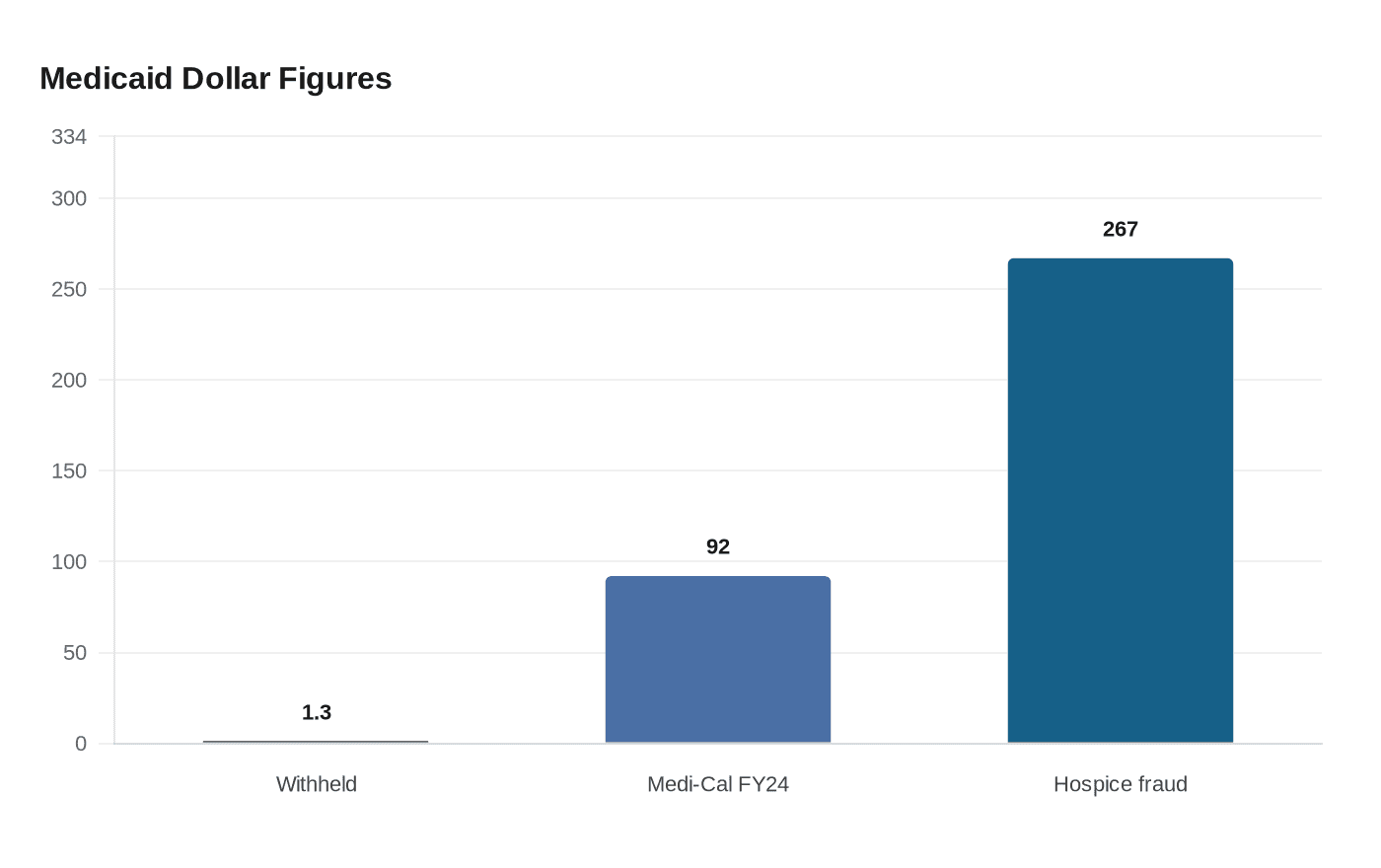
The clash also deepened an existing fight over hospice and home health oversight. CMS has repeatedly criticized California’s hospice sector, and state officials have also faced federal scrutiny over how they police those providers. On April 9, 2026, California Attorney General Rob Bonta and the Department of Health Care Services announced charges against 21 suspects in a Los Angeles hospice fraud case that they said involved $267 million in fraud.
The administration has already pressed other states as well, including Minnesota, where it previously suspended some Medicaid payments over fraud concerns. In California, the dispute turned sharper after CMS formally requested detailed information from Gov. Gavin Newsom’s office on January 27, 2026, seeking records on Medi-Cal program integrity, eligibility verification and provider oversight. What began as an audit-style demand now looks like a broader federal-state showdown over who pays for Medicaid oversight, and how aggressively California will be forced to defend its program.
Know something we missed? Have a correction or additional information?
Submit a Tip
