8-week MBSR improves sleep and reduces academic stress among Chinese adolescents
An 8-week randomized MBSR trial with 46 Chinese adolescents tested sleep quality (PSQI) and academic stress (ASQ), adding to evidence that mindfulness may help students' sleep and reduce academic stress.
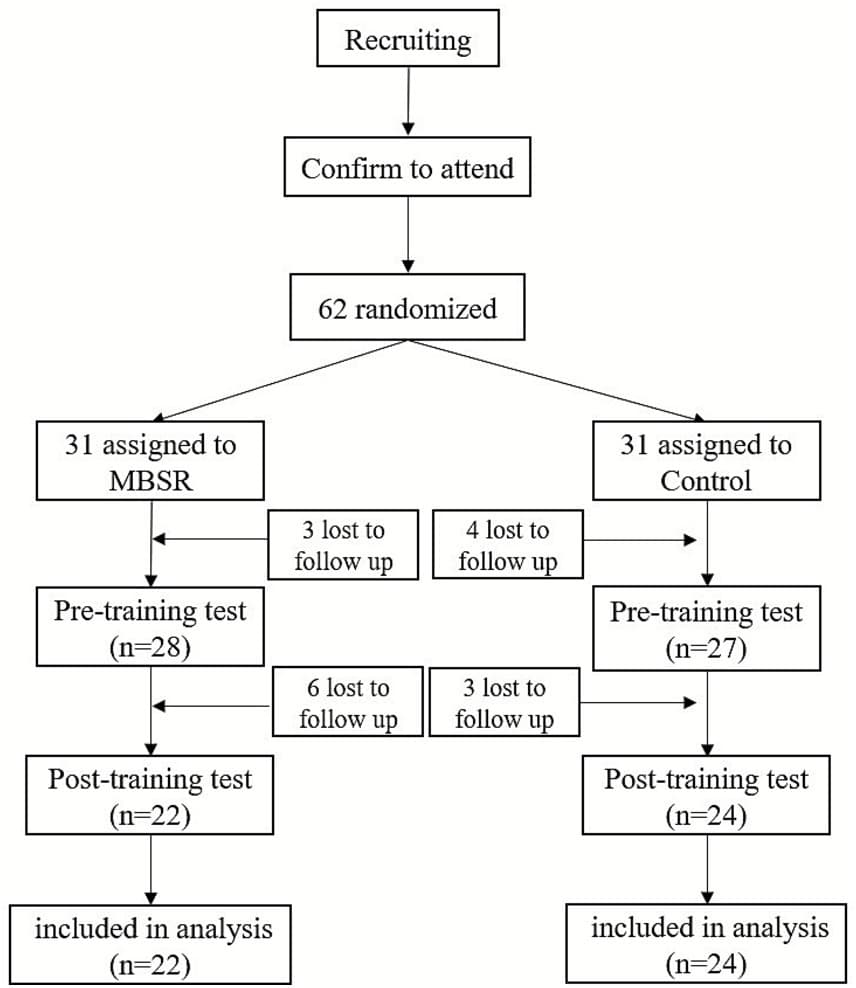
Jingxin Deng and Fang Xu conducted a randomized controlled trial testing an 8-week Mindfulness-Based Stress Reduction program in Chinese school adolescents. The trial enrolled 46 participants, with 22 assigned to the MBSR group and 24 to a control condition, and used the Pittsburgh Sleep Quality Index (PSQI) and an Academic Stress Questionnaire (ASQ) to track outcomes. The extract provided does not list numerical results, protocol details, or participant ages, but the study contributes a focused adolescent data point to a literature dominated by adult samples.
Context matters for interpretation. Evidence from adults is mixed but often positive. A pooled meta-analysis of seven randomized trials including 497 insomnia patients found that MBSR "significantly improved in sleep quality (SMD = -0.69, 95% CI: -1.12~ - 0.26, Z = 3.16, p = .002), depression (SMD = -1.83, 95% CI: -2.81-0.84, Z = 3.63, p < .001), and anxiety (SMD = -1.74, 95% CI: -2.90-0.59, Z = 2.96, p = .003)." Clinical work with health workers in Sichuan also reported benefits: Lu and colleagues concluded that "Mindfulness-based stress reduction can significantly reduce negative emotions, improve sleep quality levels of clinical medical staff members, and contribute to overall psychological and sleep health."
At the same time, reviews of student populations show nuance. "Previous literature has shown that mindfulness-based interventions can improve psychological well-being in university students, decreasing symptoms of depression, anxiety, stress, and insomnia. However, a systematic review showed that evidence on sleep quality is inconclusive." That pattern suggests population differences: strong signals in adult insomnia trials and clinical samples, while sleep outcomes among students and adolescents need clearer, population-specific evidence.

What this means for school programs and meditation practitioners is practical. The Deng and Xu trial is valuable because it applies an 8-week MBSR model to adolescents and uses validated measures such as PSQI and ASQ, but its small sample size (N = 46) and the absence of reported outcome values in the extract limit firm conclusions. Schools, counselors, and mindfulness instructors should treat the trial as promising but preliminary: prioritize program fidelity, track sleep with PSQI or similar tools, and measure academic stress with standard questionnaires before and after training.
For the mindfulness community, the next steps are clear. Obtain the full Deng and Xu report for outcome numbers and protocol details, replicate the protocol with larger samples and varied regions, and compare adolescent results with adult meta-analytic findings. If MBSR reliably improves sleep and academic stress in adolescents, it could become a low-cost, scalable component of school mental health toolkits—helping students sleep better and carry less exam-season baggage into the classroom.
Know something we missed? Have a correction or additional information?
Submit a Tip

