Bangladesh measles outbreak overwhelms hospitals, kills 336 children
Measles turned deadly because coverage slipped, clinics lagged and the virus outran the response. Bangladesh has now reported 336 child deaths and more than 50,000 suspected and confirmed cases.

Bangladesh’s deadliest measles outbreak in decades has exposed a preventable failure in routine child immunization, not an unavoidable surge. Children have filled pediatric wards across the country as doctors race to keep them breathing and hydrated, while government data put the death toll at 336 since March 15 and total confirmed and suspected cases above 50,000.
The spread has been swift and nationwide. The World Health Organization said Bangladesh notified it on April 4 that measles cases were rising across all eight divisions and in 58 of 64 districts. Between March 15 and April 14, WHO reported 19,161 suspected cases, 2,973 laboratory-confirmed cases and 166 measles-related deaths, with 79% of cases in children under 5. WHO assessed the national risk as high because of ongoing transmission, a large susceptible child population and immunity gaps.
UNICEF painted the same picture a few days earlier. As of April 7, it reported 9,883 suspected cases, 1,398 laboratory-confirmed cases, at least 128 suspected deaths and 21 confirmed deaths. Children under 5 made up 81% of cases, and infants under 9 months accounted for 34%, a reminder that the youngest children are the least protected when vaccination coverage slips. UNICEF also said 72% of cases were among zero-dose children and another 16% among partially vaccinated children.

The government launched an emergency measles-rubella campaign on April 5, targeting more than 1.2 million children ages 6 months to 5 years in 30 upazilas across 18 high-risk districts. The campaign expanded to four city corporations on April 12 and was set to go nationwide from May 3. By April 18, WHO said more than 1.492 million children had been reached, a sign of how aggressively officials were trying to catch up with an outbreak that had already taken hold.
On the ground, the strain has been visible in crowded wards and anxious households. One mother, Begum, said her daughter Afia was improving after oxygen treatment, a small relief in a crisis that has left families traveling long distances for care. Measles spreads through coughs and sneezes, has no specific cure once infection sets in, and can be especially dangerous for malnourished or medically vulnerable children, causing brain inflammation, long-term damage or death.
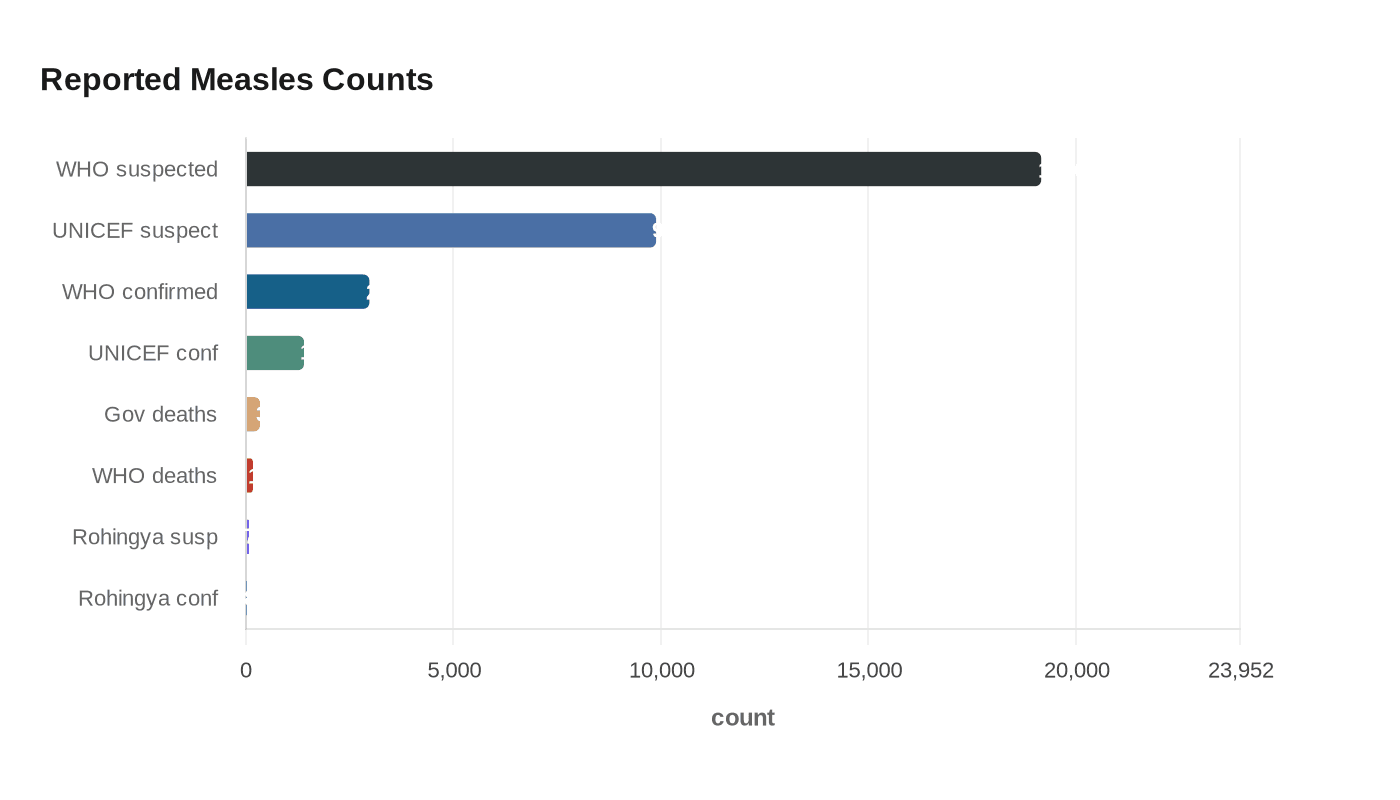
The outbreak has also touched Rohingya camps, where UNICEF reported eight laboratory-confirmed cases and 70 suspected cases in Cox’s Bazar and Bhasan Char. The broader warning is stark: UNICEF, WHO and Gavi had already said in April 2025 that nearly half a million children in Bangladesh were missing full immunization despite 81.6% coverage, with the biggest gaps in urban slums and hard-to-reach areas. This outbreak now stands as a test of whether a low-cost preventive tool can still be deployed quickly enough after the virus has already spread.
Know something we missed? Have a correction or additional information?
Submit a Tip

