Blood test for tuberculosis nears key accuracy target, study finds
A blood-based TB test is closing in on the WHO accuracy bar, a potential boost for children, HIV patients and clinics where sputum testing breaks down.
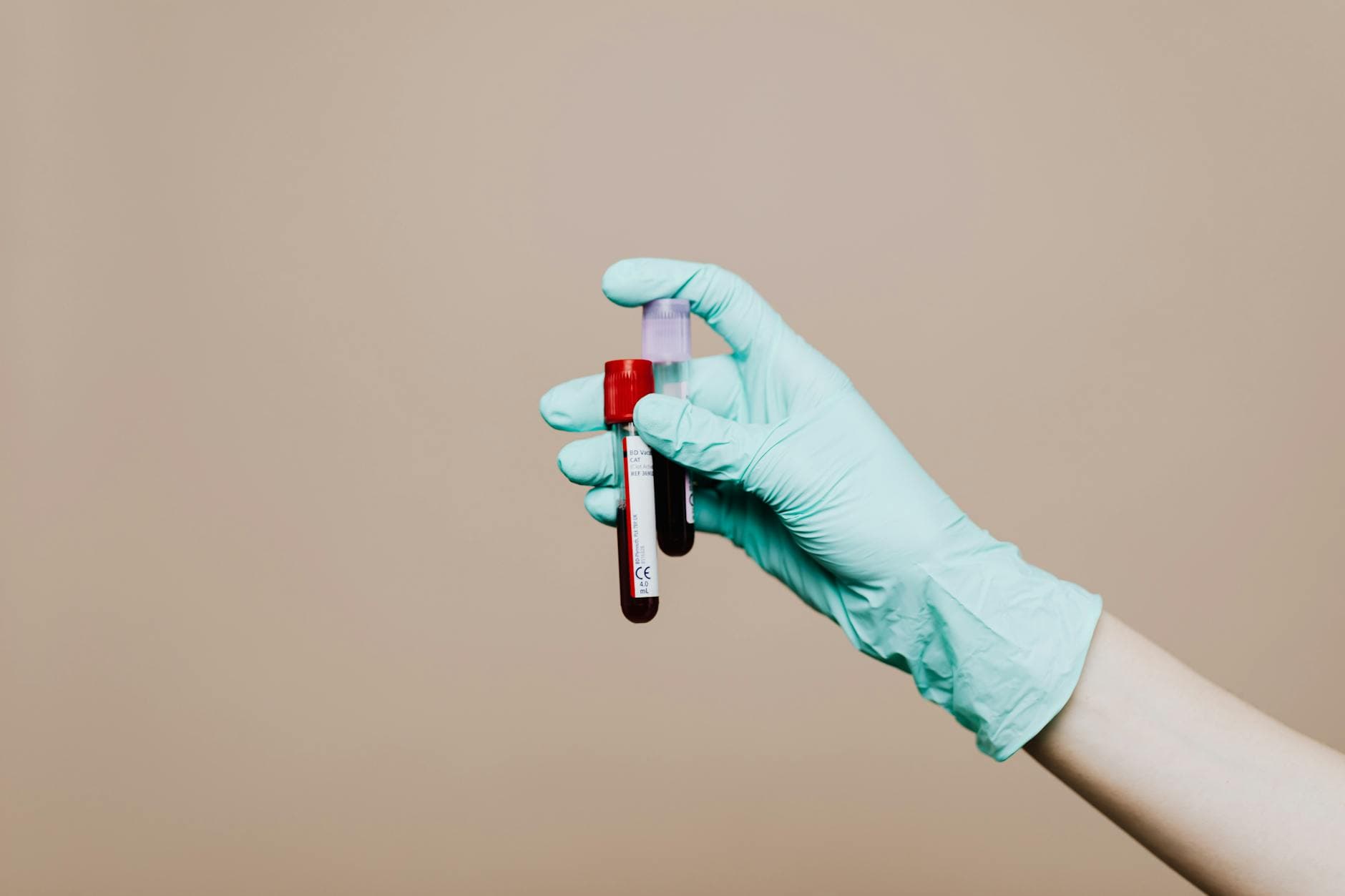
A blood test that can screen for tuberculosis in under half an hour could change who gets diagnosed first, especially in places where sputum samples are hard to obtain from children, people living with HIV and patients in rural clinics. The larger challenge is not only improving accuracy, but getting a faster triage tool into overburdened health systems where delays still let cases slip through.
Researchers said Cepheid’s prototype Xpert MTB Host Response, or Xpert HR, was the first blood-based TB assay to come close to the World Health Organization’s minimum diagnostic targets for a triage test, which call for 90% sensitivity and 70% specificity. In a prospective diagnostic accuracy study across outpatient clinics in Viet Nam, India, the Philippines, Uganda and South Africa, the late-prototype test was run on either capillary or venous blood from adults 18 and older with cough lasting at least two weeks. Related work in Pakistan also tested the prototype GeneXpert MTB-HR cartridge in people with TB-like symptoms.
The appeal is straightforward: TB testing has long leaned on sputum, which is slow to collect and often unreliable when patients cannot produce enough phlegm. That problem is especially acute in young children and many patients with HIV. A blood-based triage test could cut down on missed cases, reduce unnecessary confirmatory testing and speed patients toward treatment sooner, all of which matter in countries carrying the heaviest burden.
The new result lands against a stubborn global backdrop. The World Health Organization said the world’s TB incidence rate fell only 1.7% from 2023 to 2024 and stood just 12.3% below 2015 levels, still far from the End TB Strategy milestone. Rapid testing coverage improved, but only from 48% in 2023 to 54% in 2024, underscoring how slowly diagnostics are being deployed where they are needed most.
The U.S. picture is also a reminder that TB has not disappeared from high-income countries. The U.S. Centers for Disease Control and Prevention said 10,260 TB cases were provisionally reported in 2025, a 1% decline from 2024, when case counts topped 10,300, the highest level since 2011. CDC guidance says blood testing is a standard option for TB infection screening and requires only one visit, while the Xpert MTB/RIF assay can detect TB and rifampin resistance in less than two hours, far faster than standard culture, which can take two to six weeks for the bacteria to grow.
The public health prize is clear. Since 2011, rapid molecular tests have transformed TB diagnosis compared with older microscopy and culture methods. The next step is making sure a faster, non-sputum test reaches clinics that need it most, before another patient cycle of delay, missed diagnosis and ongoing transmission takes hold.
Know something we missed? Have a correction or additional information?
Submit a Tip