CMS Proposes Hospice Scoring System to Boost Transparency, Combat Fraud
CMS proposed a nine-metric hospice 'scoring' system that would post provider performance publicly, after 200+ Medicare enrollment revocations in six states for fraud.

The Centers for Medicare & Medicaid Services released a sweeping proposed rule on April 2 that would assign every Medicare-participating hospice a publicly posted score built from nine claims-based measures, a move the agency framed as its most direct strike yet against fraud in a payment system slated to grow by an estimated $785 million in fiscal year 2027.
The scoring mechanism, called the Service and Spending Variation Index (SSVI), sits at the center of proposed rule CMS-1851-P. The SSVI includes a comprehensive scoring system calculated using nine claims-based measures, each representing different aspects of hospice utilization as well as non-hospice spending, identifying providers for increased transparency and oversight.
The index assigns hospices a score based on metrics gathered from claims, including non-hospice spending, the percent of beneficiaries discharged with a length of stay of 180 days or more, average minutes per routine home care day, and the percent of live discharges where beneficiaries return to the same hospice within seven days. While not a direct indicator of fraud, waste, or abuse, a high SSVI score would represent a potential higher level of concern, signaling possible program integrity risks or inappropriate utilization. Provider-level data and each facility's score would be posted on CMS's Hospice Center webpage.
CMS Administrator Dr. Mehmet Oz put the stakes plainly: "Hospices exist to help Americans die peaceful, dignified deaths, not to line the pockets of fraudsters."
The fraud pressure behind the proposal is grounded in recent enforcement history. Enhanced oversight in four states with elevated fraud risk, Arizona, California, Nevada, and Texas, has already produced more than 200 hospice Medicare enrollment revocations for failure to comply with CMS requirements, and the agency has since expanded that targeted approach to Georgia and Ohio.
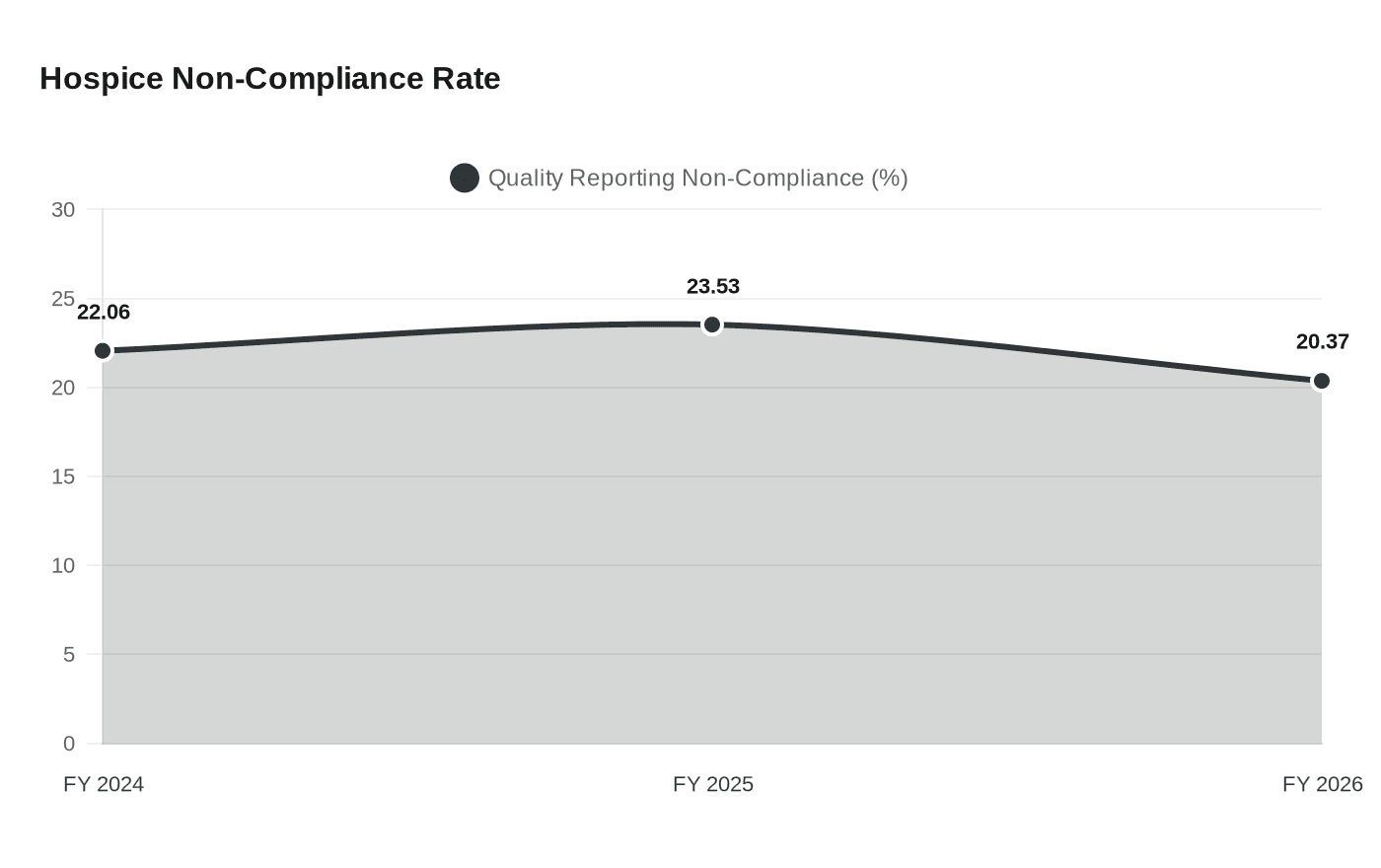
Quality reporting compliance is woven directly into the scoring regime, and the trend data heading into that requirement is not encouraging. In FY 2024, the first year after CMS doubled the annual payment update penalty for non-compliance, 22.06 percent of hospices were still found non-compliant. The rate rose to 23.53 percent in FY 2025, before easing to 20.37 percent in FY 2026. One in five hospices is still failing to submit the quality data that feeds both public accountability tools and the SSVI itself.
To further support consumer transparency, CMS is also proposing a new icon for the Medicare.gov Care Compare site identifying hospices that did not meet requirements under the Hospice Quality Reporting Program. A separate provision would require hospices to make an Addendum available to all beneficiaries at the time of election, giving families clearer information about non-covered items, services, and drugs, a change CMS said could reduce out-of-pocket costs and ease the burden of seeking that information at a vulnerable time.
For FY 2027, CMS proposes to update the hospice payment rate by 2.4 percent, an estimated increase of $785 million in payments from FY 2026, with the proposed per-beneficiary cap rising from $35,361.44 to $36,210.11.
For families navigating one of the most consequential decisions they will ever face, the SSVI could function as a practical shortcut when comparing providers. Its credibility depends entirely on methodology. In the comment period now open to hospice providers, trade groups, patient advocates, and rural and tribal health stakeholders, expect hard questions over how score thresholds are set, whether the metrics adequately distinguish clinical complexity from billing abuse, and what appeals process will exist for providers who believe their score misrepresents the care they deliver. While most hospices are anticipated to receive a low score, facilities with high-end scores could be subject to additional review to assess potential program integrity or compliance issues.
If finalized, a public SSVI score could become as consequential to a hospice's competitive standing as any state survey, making visible to grieving families what has long been legible only to federal auditors.
Know something we missed? Have a correction or additional information?
Submit a Tip

