Community health workers help aging Americans stay home, get care
Community health workers are the quiet bridge keeping older adults at home, while Medicare and Medicaid slowly expand coverage around a much bigger aging crisis.
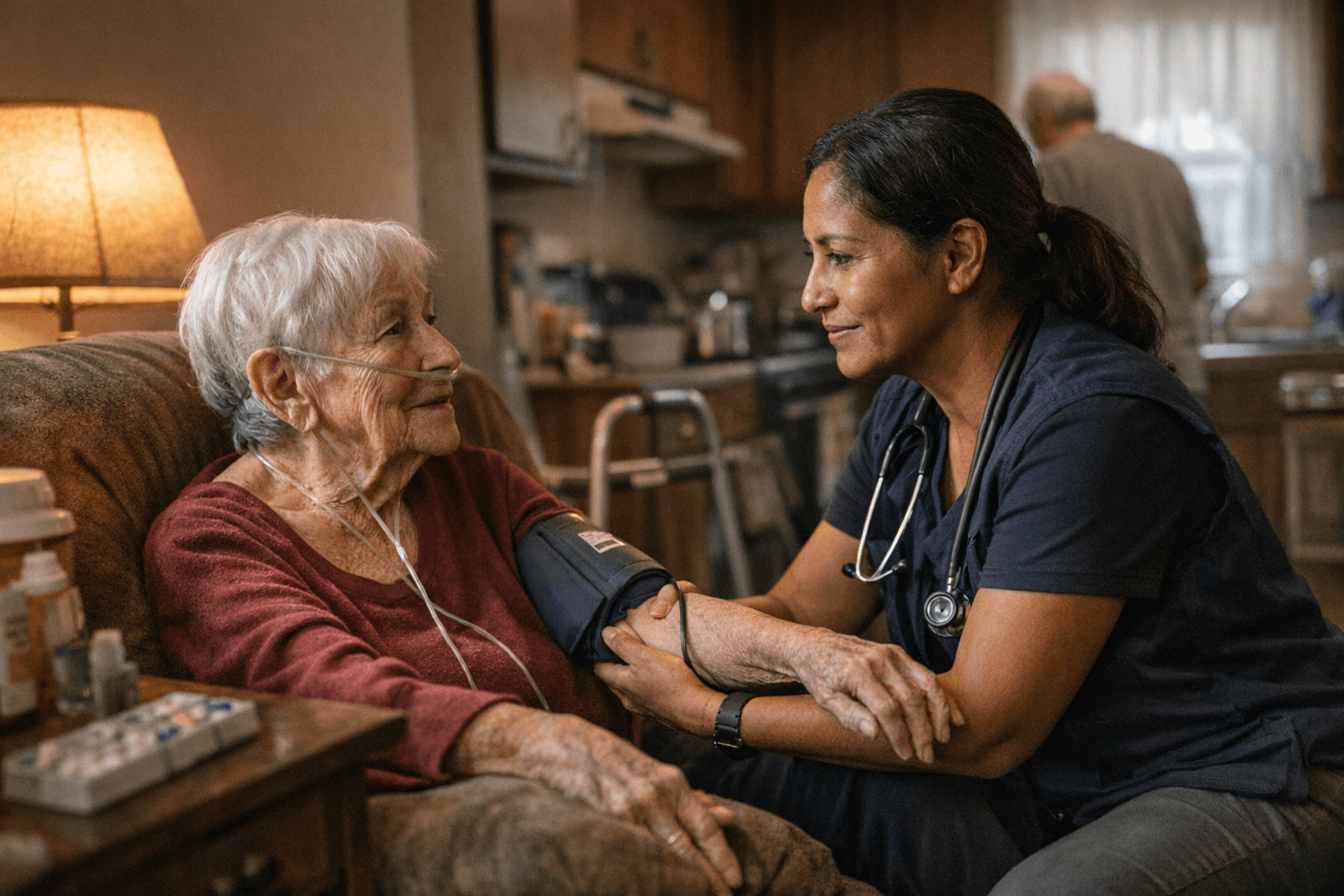
The quiet workforce keeping older adults out of crisis
Community health workers are becoming one of the most important, least visible parts of the aging-care system. They help older adults navigate health and social services, solve practical barriers, and stay connected to care when doctors, nurses, and family caregivers are stretched thin. As more Americans age into longer, more complex years of need, this layer of support is becoming central to whether people can remain at home or end up in hospitals and nursing homes.
The stakes are rising because older Americans overwhelmingly want to age in place. AARP’s 2024 Home and Community Preferences Survey found that 75% of adults 50 and older want to remain in their current homes as they age, and 73% want to stay in their communities. Many still assume a move will be inevitable, but the preference is clear: people want stability, familiar surroundings, and care that comes to them.
Why demand is climbing so fast
The aging of the U.S. population is not a distant trend. The Congressional Budget Office says the country is projected to become older on average from 2025 to 2055, with the number of people age 65 or older increasing markedly. That shift matters because older adults often need more ongoing help, more coordination, and more support for basic daily tasks than the current care system can comfortably absorb.
The health profile of older adults underscores the pressure. The Centers for Disease Control and Prevention reports that in 2024, 24.3% of noninstitutionalized adults age 65 and older were in fair or poor health. The same data show that 9.4% had difficulty with self-care, 47.8% had diagnosed arthritis, and life expectancy at age 65 was 19.7 years. That is not a brief period of support. It is often decades of managing chronic conditions, mobility limits, medication routines, and changing family circumstances.
What community health workers actually do
Community health workers are not a substitute for clinicians. Their value comes from the space they fill between medical visits and daily life. They connect people to health and social services, help break down barriers tied to social determinants of health, and support care coordination, health education, and emotional support. In practice, that can mean helping someone understand a care plan, follow through on appointments, or get linked to resources that make treatment possible.
That role matters because medical advice alone does not solve transportation problems, housing instability, food access, caregiver burnout, or confusion about coverage. Community health workers operate in that gap. They help people turn a prescription or discharge plan into something manageable at home, which is exactly where many older adults want to stay.
The home-care system already depends on this kind of support
The broader home-care system is already carrying a huge load. KFF estimates that more than 4 million people use Medicaid home- and community-based services, known as HCBS. Those services cover help with everyday activities such as eating, bathing, dressing, meal preparation, medication management, and housekeeping. That is the backbone of aging at home for many people with disability, chronic illness, or frailty.
But that backbone is under strain. States have been trying to respond to direct-care shortages by raising Medicaid payment rates and expanding worker opportunities. The Centers for Medicare and Medicaid Services has also issued guidance to states on improving access to HCBS and reminding them of tools that can better connect direct support workers to people receiving Medicaid-covered home care. The policy direction is clear: keep people at home if possible, because the alternatives are costlier, more disruptive, and often less aligned with what older adults want.
What happens if the workforce stays too small
When community health workers are understaffed or underpaid, the consequences are not abstract. People with chronic disease and limited self-care capacity are more likely to fall through the cracks, miss support, or cycle into crisis care. That can mean more reliance on family members who are already stretched, more avoidable strain on emergency and inpatient systems, and more pressure to move people into institutional care sooner than necessary.
The fiscal stakes are just as important as the human ones. Medicare and Medicaid absorb the cost when health problems are not managed early and at home. If support services remain thin, more needs get pushed into higher-cost settings. That is why community health workers are not just a social service add-on. They are part of the cost structure of aging in America.
How policy is starting to catch up
Coverage is expanding, but unevenly. KFF found that as of July 1, 2022, 29 of 48 responding states allowed Medicaid payment for some community health worker services. That means many states have already recognized the value of paying for this work, but access still depends heavily on geography and state policy choices.
Medicare has also started to make room for related services. Beginning in 2024, the program adopted payment codes for community health integration, principal illness navigation, caregiver training services, and physical activity and nutrition risk assessment services. Those codes matter because payment policy shapes whether these services can scale. If a service has no stable reimbursement, it is much harder to build a workforce around it and much harder for patients to count on it.
Why equity has to be part of the solution
The social justice dimension is not separate from the clinical one. Community health workers help reduce barriers that often hit lower-income households, disabled older adults, and people with less family support the hardest. They can be especially important when care systems assume that someone at home has plenty of unpaid help, digital access, and time to navigate bureaucracy. Many older adults do not have that cushion.
That is why underpaying this workforce carries a bigger cost than vacancies alone. It widens the gap between people who can successfully age at home and people who cannot. It also shifts the burden onto families, neighborhoods, and safety-net systems that are already absorbing too much unpaid labor.
The policy lesson is straightforward: if the country wants more older adults to stay home, it has to invest in the workers who make that possible. Community health workers are not a side feature of aging care. They are the hidden infrastructure that keeps the system from breaking.
Know something we missed? Have a correction or additional information?
Submit a Tip

