Condom Use Declined Sharply Among Single Americans From 2008 to 2019
The share of never-married women using condoms at last sex fell from 52% to 43% in a decade, as sexual networks shifted and barrier use eroded among high-risk groups.

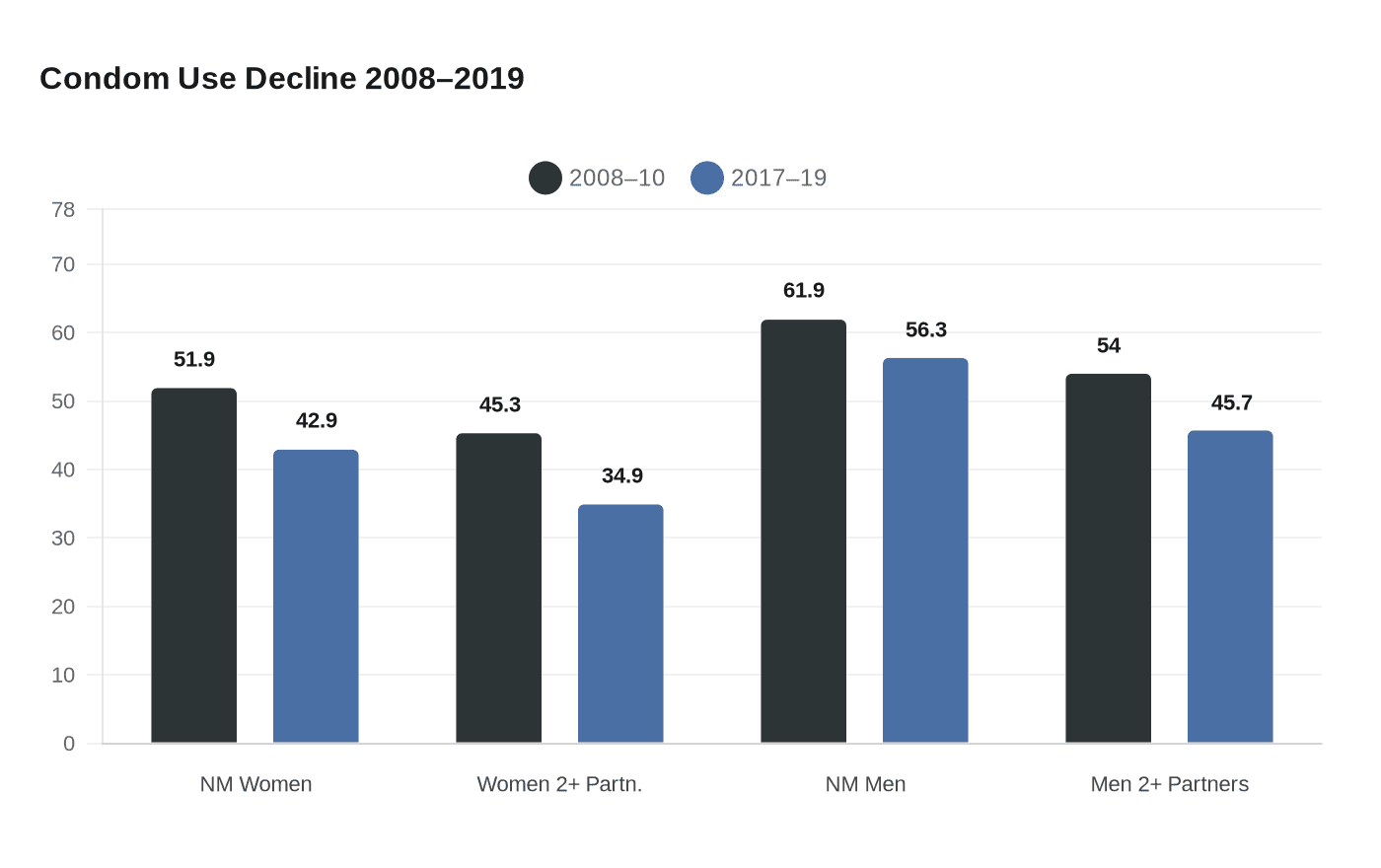
The share of never-married American women who used a condom at their last vaginal sex fell from 51.9% to 42.9% between 2008-10 and 2017-19, a nearly 9-point drop that tracks closely with the country's ongoing STI epidemic, according to a large national study published in PLOS ONE.
The decline was steeper among women with two or more opposite-sex partners in the prior year, dropping from 45.3% to 34.9%, meaning fewer than one in three multiply partnered women were using condoms by the end of the study period. Never-married men showed similar erosion, from 61.9% to 56.3%, while men with multiple partners fell from 54.0% to 45.7%.
The analysis, led by David A. Katz and colleagues, drew on pooled National Survey of Family Growth data covering 28,027 females and 23,479 males between the ages of 15 and 44. By stratifying trends along marital status and partner count across 2008 to 2019, the researchers produced a more granular picture of who is driving STI risk than previous surveillance reports had offered.

The timing matters. Even as these condom use figures fell, combined cases of chlamydia, gonorrhea, and syphilis declined 9% from 2023, but more than 2.2 million were still reported in 2024, a figure 13% higher than a decade ago. The years the Katz study covers capture precisely the period when PrEP (pre-exposure prophylaxis) scaled up as an HIV prevention tool and when researchers began documenting risk compensation, the tendency toward reduced condom use associated with adopting new protective measures.
The study also documents a doubling in the share of never-married women who reported sex with male partners who also have male partners, from 2.5% to 5.1%. For never-married males, the same measure rose from 3.8% to 5.5%. That shift in network structure carries direct STI implications: sexual connections bridging higher-prevalence and lower-prevalence populations increase transmission pathways even when individual behavior appears unchanged.
Testing trends offered a partial counterweight. Past-year chlamydia testing rose among married females (from 13.0% to 17.1%), previously married females (27.6% to 45.8%), and people with a single partner (21.7% to 25.4%). The jump among previously married women suggests targeted clinical screening campaigns have had measurable reach. But those gains did not uniformly cover the groups where condom use fell most sharply, leaving a gap between risk exposure and detection.
The paper also noted declines in the frequency of vaginal sex among cohabiting females (from a mean of 9.46 acts to 7.40 in the four weeks before interview) and never-married males (4.11 to 3.40), a finding that complicates a straightforward risk narrative without offsetting the protective loss from reduced barrier use.
Katz and colleagues wrote that "understanding trends in sexual behaviors, networks, and testing by marital/cohabiting status and partner number can contextualize their contributions to the STI epidemic and support sexual health services tailoring and prioritization." The practical prescription embedded in that language is targeted intervention: chlamydia screening programs have shown they can reach married and previously married women, but public health messaging, clinic outreach, and digital health platforms have yet to arrest the condom use erosion among never-married and multiply partnered Americans who carry the greatest exposure burden.
Sources:
Know something we missed? Have a correction or additional information?
Submit a Tip