Family caregiving surges, 63 million Americans juggle rising costs and crisis
One in 4 U.S. adults now provides care, and many are spending thousands a year while retirement and housing plans bend under the strain.

Family caregiving has moved from a private burden to a national financial pressure point. AARP and the National Alliance for Caregiving say 63 million Americans, or 1 in 4 adults, are now providing ongoing care for older adults, people with serious illnesses or people with disabilities. That is up by 20 million since 2015, a jump that shows how many middle-class households are quietly absorbing the costs of aging, illness and disability without much room to spare.
The scale of the problem has been building for decades. The Caregiving in the U.S. survey series began in 1997 and has been fielded every five years since 2004, making it one of the most authoritative national datasets on the issue. AARP says the 2025 edition is its most comprehensive to date, and the findings point to a caregiving system that increasingly depends on family members doing work that once would have fallen to paid services or institutions.
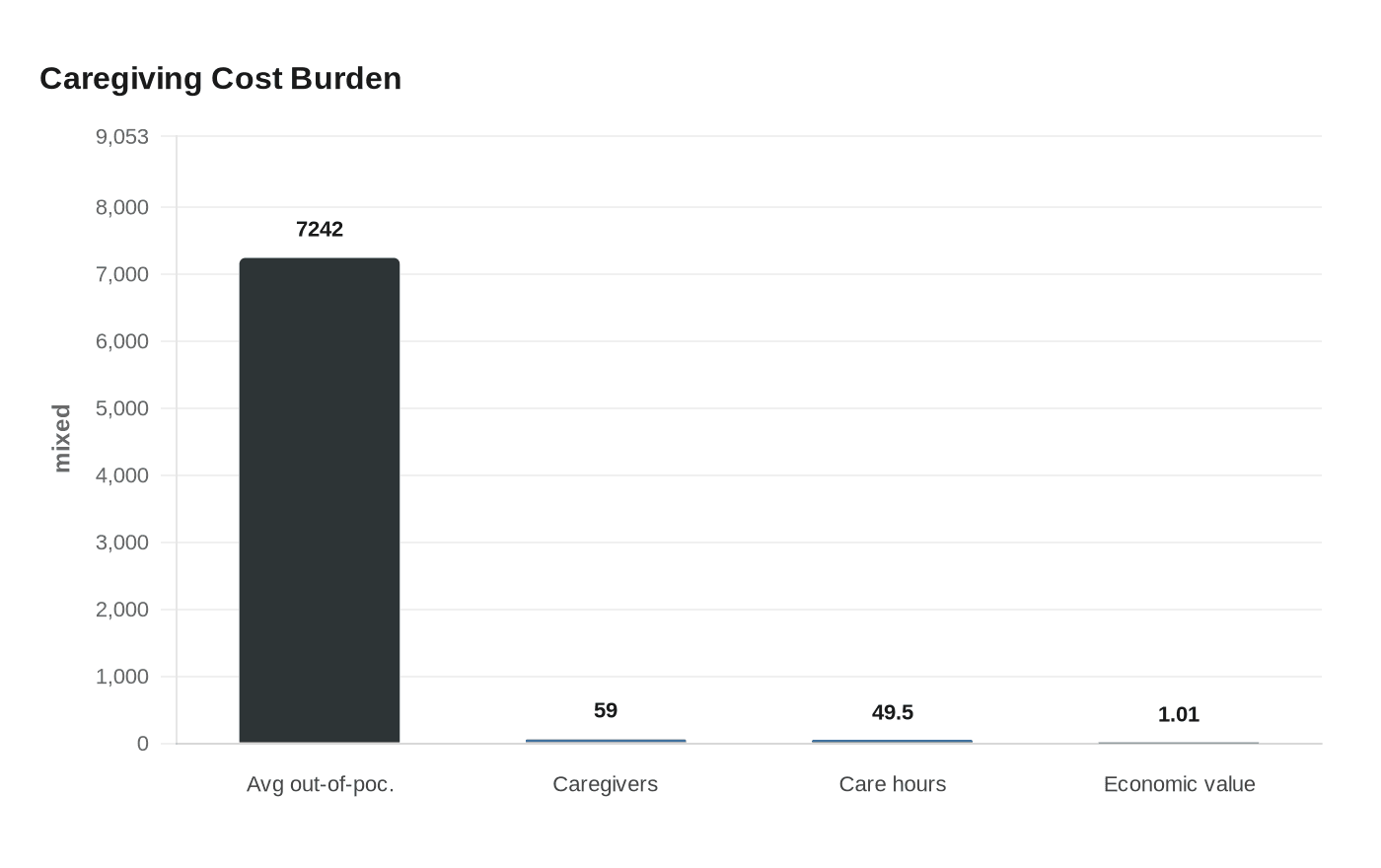
The financial toll is immediate and uneven. AARP has reported that three-quarters of family caregivers surveyed spent an average of $7,242 a year out of pocket on caregiving, a sum that can rattle savings, stretch credit cards and force hard choices about rent, mortgages and retirement contributions. Those costs hit hardest for Hispanic/Latino and African American caregivers, younger caregivers and people caring for loved ones with dementia, underscoring how caregiving pressure falls unevenly across race, age and diagnosis.

The unpaid labor is immense. AARP reported in March 2026 that about 59 million caregivers provided 49.5 billion hours of care in 2024, with an estimated annual economic value of $1.01 trillion. Nancy LeaMond, AARP’s chief advocacy and engagement officer, has said caregivers need an agenda of solutions to meet the substantial financial pressures they face, especially as working caregivers are pushed to choose between staying employed and caring for a parent, spouse or friend.
Longevity is driving much of that strain. The Social Security Administration says retirement planning must account for longer life expectancy, and its planner notes that a worker can typically begin retirement benefits at 62 after paying Social Security taxes for at least 10 years. But starting early reduces monthly benefits. For people reaching 65 on April 1, 2025, SSA puts life expectancy at 84.3 for men and 86.9 for women, a reminder that retirement money often must last far longer than many households plan for.
The federal policy response has begun to catch up. The Administration for Community Living, which oversees programs that advance independence and inclusion for older adults and people with disabilities, issued a 2024 report to Congress on progress under the National Strategy to Support Family Caregivers. That strategy was developed by the Family Caregiving Advisory Council and the Advisory Council to Support Grandparents Raising Grandchildren. But the numbers make the challenge plain: families are already carrying the load, and the country’s retirement, housing and long-term care systems still rely on that unpaid work to hold together.
Know something we missed? Have a correction or additional information?
Submit a Tip

