Health insurers post strong quarter, but cost pressures remain risky
Insurers saw medical costs cool in the first quarter, but the real test is whether that relief reaches premiums, deductibles or coverage decisions.
Health insurers are finally getting some relief from medical-cost pressure, but patients still face a bigger question: will lower claims trends translate into cheaper coverage, or just better earnings for Wall Street?
UnitedHealth Group set the tone with first-quarter 2026 medical cost ratio of 83.9%, down from 84.8% a year earlier and roughly 180 basis points below FactSet’s 85.7% consensus estimate. The company raised its 2026 outlook after the quarter, and Centene, Elevance Health and UnitedHealth also lifted profit forecasts after results that pointed to a more stable cost environment than investors had seen in much of the past two years.
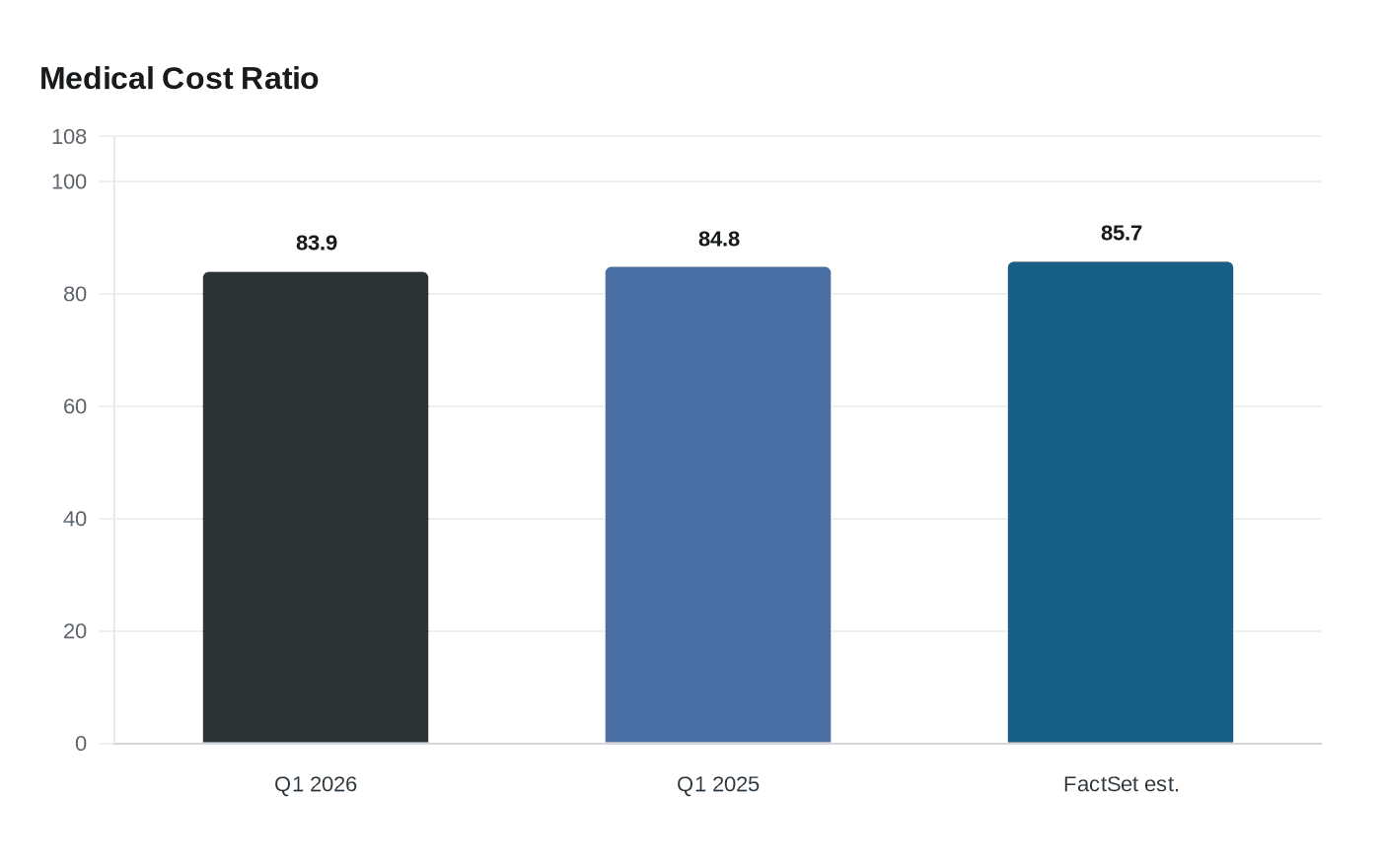
The rebound mattered because the S&P managed care index had fallen more than 12% since July 2023, a sign of how much pressure rising utilization, reimbursement friction and government-backed plans had put on the sector. Analysts said the first quarter was the strongest showing insurers had delivered since the pandemic, but they also warned against reading too much into it. Many members have not yet met their deductibles early in the year, which can make claims look lighter in the first quarter than they will later. Morningstar analyst Julie Utterback said it was probably too early to declare victory, and weaker respiratory illness activity last winter may also have temporarily softened claims.
That seasonal cushion is important for consumers because it means the industry’s improved numbers do not yet answer the hard question of what insurers will do when they set premiums and benefits for the next cycle. The second quarter is often the real stress test, when deductibles are further along, claims patterns become clearer and insurers can see whether the cost relief is durable. UBS analyst AJ Rice said further positive earnings revisions were possible if cost trends stayed constructive, but the uncertainty remains high.
Policy decisions will also shape the next round of pricing. On April 6, the Centers for Medicare & Medicaid Services released its 2027 Medicare Advantage and Part D rate announcement, saying Medicare Advantage plan payments would rise by a net average 2.48%, or more than $13 billion versus 2026. That should help plans heavily exposed to Medicare Advantage, but it does not guarantee lower premiums or fewer coverage restrictions for enrollees.
Medicaid remains another swing factor. The post-pandemic eligibility unwind continues to reshape membership, and the 2024 CMS renewal rule is still working through state systems, leaving some insurers with sicker and more expensive members. Humana, one of the biggest Medicare Advantage players, did not raise its 2026 guidance in the reported quarter, and chief executive Jim Rechtin said the company was where it expected to be while noting that medical-cost trends are still outpacing funding in some areas. For now, the industry’s improving outlook looks real, but patients will need another quarter of evidence before they can tell whether it shows up in their own bills.
Know something we missed? Have a correction or additional information?
Submit a Tip