How Tracking Glucose Every Day Changes the Way You Live
Strapping a glucose sensor to your arm doesn't just track data; for many healthy users, it rewires how they eat, sleep, and think about food in ways science is still catching up to.

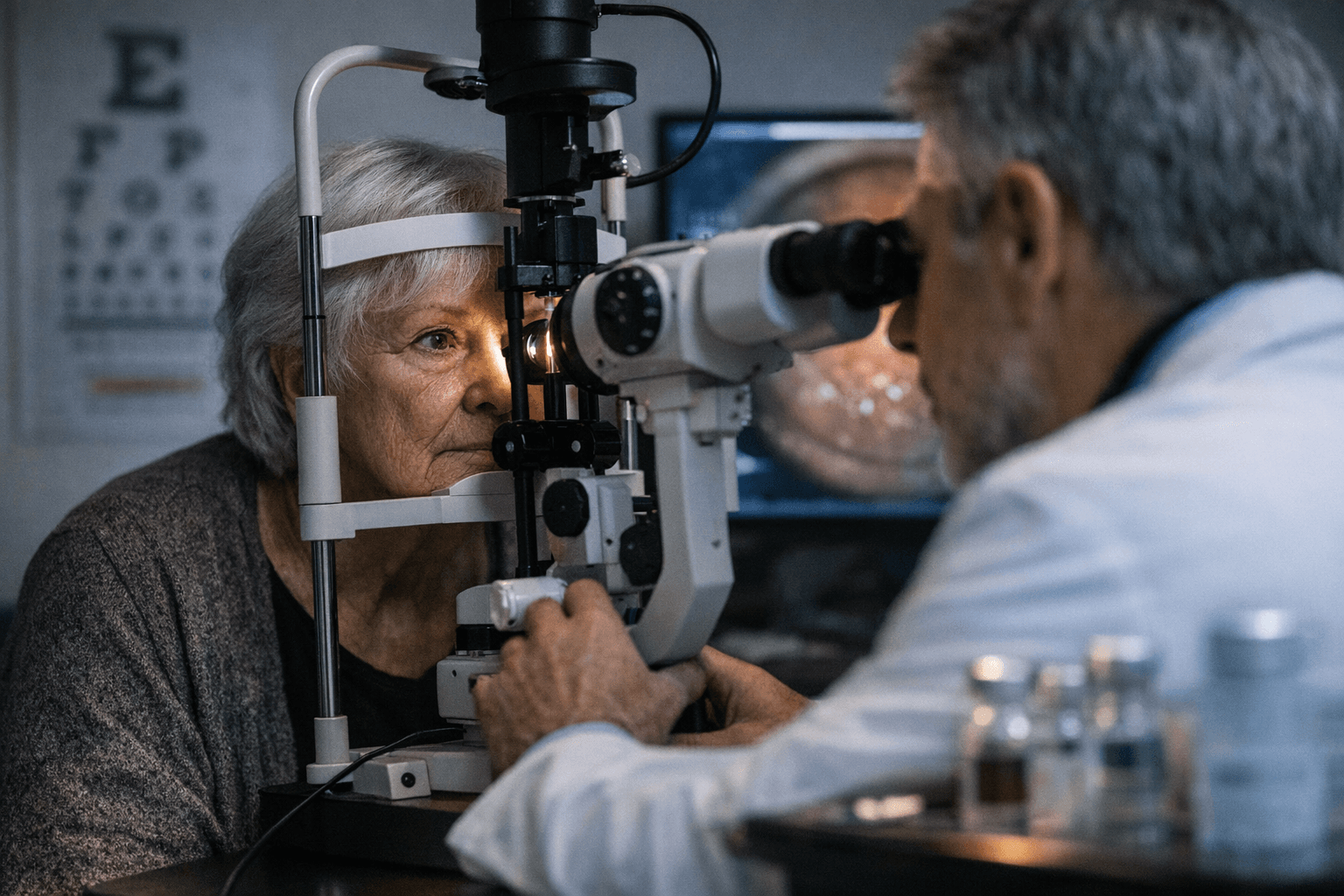
Before the Uber arrived, there was one more thing to do. Tearing open an isopropyl alcohol wipe, swabbing a patch of skin on the back of the arm, and pressing a small applicator into place until a biosensor clicked in. Only then was it time to leave for the airport. That ritual, repeated every ten to fifteen days, is now a fixture of life for a rapidly growing number of people who have never been diagnosed with diabetes and, by most clinical measures, don't need a continuous glucose monitor at all.
The devices have existed since 1999, when the FDA first cleared them for people managing diabetes. What has changed is the market. In June 2024, Abbott gained FDA approval for two new over-the-counter continuous glucose monitoring systems, the Lingo and the Libre Rio, making it possible for any adult to monitor blood glucose in real time, diabetes or not. Dexcom's Stelo is available without a prescription for about $100 a month, and Abbott's Lingo runs around $49 per sensor, with each lasting roughly two weeks. Platforms like Levels, Nutrisense, and Signos have built subscription businesses around interpreting that data, bundling sensors with coaching apps and metabolic health scores. The result is a new category: the medical-grade wearable sold as a lifestyle product.
From Clinic to Consumer
The clinical case for CGMs in people with diabetes is well established. Wearing a CGM has been used not only for diabetes management, but with goals of improving glucose patterns to avoid diabetes, improving mental or physical performance, and promoting healthy behavioral changes. For people who use insulin, the devices are genuinely life-saving, providing alerts when blood sugar drops dangerously low and giving clinicians a detailed picture of glycemic control over time.
But the evidence base does not transfer cleanly to healthy populations. A narrative review led by researchers at UCL and Birmingham Children's Hospital found there is a lack of evidence to demonstrate the effective use of CGMs in people not living with diabetes. The researchers concluded there is currently little published evidence on how accurate CGMs are in measuring blood glucose levels in this group, nor sufficient evidence of what the health benefits might be. That evidence gap has not stopped companies from filling it with marketing. Abbott's Lingo brand released a 2025 wellness report asserting that "Americans are facing a metabolic health crisis," claiming that nine out of ten deaths in America are linked to chronic metabolic conditions. Critics noted the underlying study that report cited does not mention metabolism, and that the broad category of metabolism implies non-diabetics are inherently unhealthy.
The Data Feedback Loop
For users without diabetes, putting on a CGM for the first time is often described as revelatory. Watching a number rise sharply after eating a bowl of pasta, or dip unexpectedly during an afternoon meeting, creates a visceral sense of cause and effect that nutrition labels and annual bloodwork never provide. CGM data can be used as a biofeedback tool to drive behavior change in otherwise healthy individuals. Research backs up the behavior-change effect to a degree: compared with control groups, CGM users showed a significantly lower proportion of energy intake from carbohydrates, although no significant differences were observed in total energy intake or in the proportions of energy from fat or protein.
The question is whether that behavioral shift is always beneficial, or whether the constant signal starts to distort the relationship between a person and food. Calorie and fitness monitoring has been linked to the development of anxiety, compulsive behaviors, and disordered eating patterns, though the consequences of CGM data on exacerbating these issues has not been extensively explored. Researchers and clinicians are beginning to describe a specific pattern: the pursuit of a "flat" glucose line as a goal in itself, regardless of whether glucose variability is actually causing any harm.
The Anxiety Problem
The psychological risks are real and documented, even if still underweighted in the marketing. Cases of adverse mental health outcomes developing alongside CGM use have been documented, with people not living with diabetes who use continuous glucose monitoring potentially experiencing obsessive thinking or developing anxiety. One study author endorses preassessment and providing psychoeducation, or combining CGM initiation with therapy, mindfulness, and exposure response prevention.
The UCL-led review also found evidence that CGM use in people not living with diabetes could cause anxiety about what is normal in terms of diet and blood sugar levels. Researchers said this could present a risk of developing eating disorders, such as orthorexia, an unhealthy obsession with eating healthily. One study noted a significant increase in self-reported anxiety levels related to food choices in a subset of healthy CGM users who engaged in competitive tracking, and the pursuit of perfectly flat glucose curves was found to lead to highly restrictive and unsustainable eating patterns.
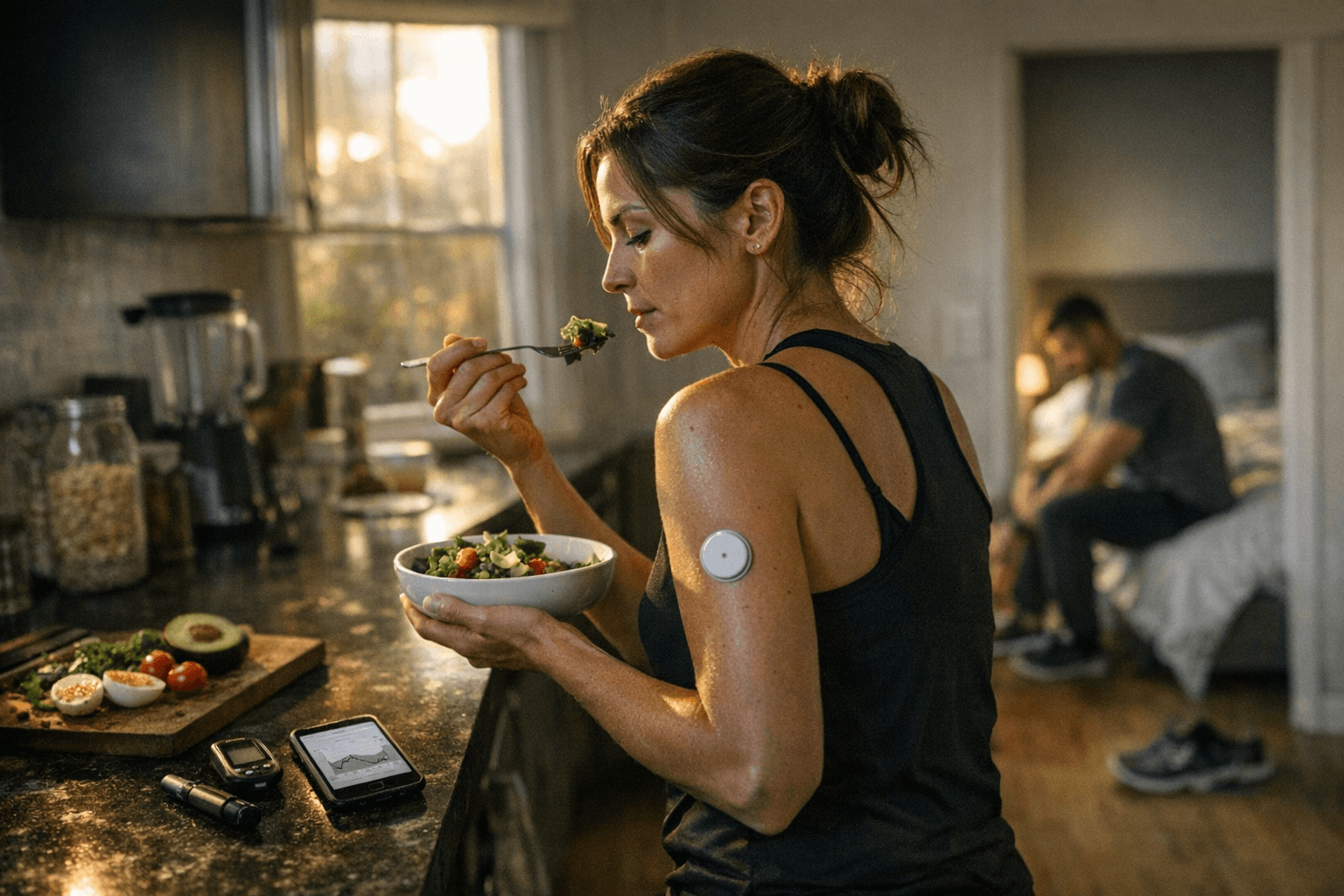
Earlier research on CGMs in clinical populations offers a preview. Studies of youth using CGMs reported greater general anxiety and greater depressive symptoms compared to control populations, and all patients using CGM reported greater negative affect and poorer communication around blood glucose levels. Translating those findings to self-directed adults using consumer apps involves different variables, but the direction of the signal is consistent: more data does not automatically mean better mental or physical health.
What the Device Can't Tell You
There is also a fundamental measurement problem that the wellness framing tends to obscure. CGMs do not measure blood glucose. CGM systems measure glucose in interstitial fluid, not in blood. Rapid changes in one compartment are not accompanied by similar changes in the other, but follow with some delay, and this time lag hampers detection of events like hypoglycemia. Typically there is a five-to-ten minute lag between interstitial and blood glucose levels, and this should be communicated to clinicians and patients. In practice, this means the spike you see on your app after breakfast is a delayed, estimated approximation of what was actually happening in your bloodstream.
The lag is not merely a technical footnote. The lag time between blood glucose and interstitial glucose can range from two to twenty minutes, and the difference is most noticeable during increased rates of change, such as after a meal, after treating a low glucose event, during and immediately after exercise, or after taking certain medications. For a person with diabetes relying on the device for insulin dosing, these limitations are managed with clinical training. For a wellness consumer watching a number tick upward after eating a banana and wondering whether fruit is now the enemy, the data lacks the interpretive context that would make it useful rather than alarming.
For athletes without diabetes, what is considered "healthy," "suboptimal," or "optimal" in terms of CGM metrics remains unclear. The same ambiguity applies to any person without a metabolic condition striving to optimize numbers that have no established target range for their population.
Who Actually Benefits
Clinicians are not uniformly opposed to expanded CGM use, but they are increasingly specific about who stands to gain from it. People with prediabetes, those with a strong family history of type 2 diabetes, and individuals working with a physician on documented metabolic concerns represent a different clinical calculus from someone who is healthy by every available measure and wants to experiment with biohacking. Health care professionals need to ascertain which patients can most effectively use CGM by understanding the emotional, cognitive, and behavioral characteristics of people who want to use the technology, allowing providers to assess and assist patients in managing expectations.
If a monitoring system sometimes provides inaccurate information or false alarms, unnecessary anxiety, calls or visits to the doctor, emergency room visits, and even inappropriate treatment may follow. That calculus looks very different when the person wearing the sensor is managing a chronic condition versus optimizing a fitness routine.
The sensor clicked into place, the Uber arrived, and the data continued to stream. Numbers are easy to generate. What remains harder, and what no algorithm has yet solved, is knowing when a number means something, when it doesn't, and whether watching it round the clock is the same thing as understanding your health.
Sources:
Know something we missed? Have a correction or additional information?
Submit a Tip