Scientist Receives Experimental ALS Drug He Helped Connect His Family To
A genomics researcher who studies gene switches is now having one silenced in his own spine; Jeff Vierstra has received experimental ALS infusions for three years and remains symptom-free.

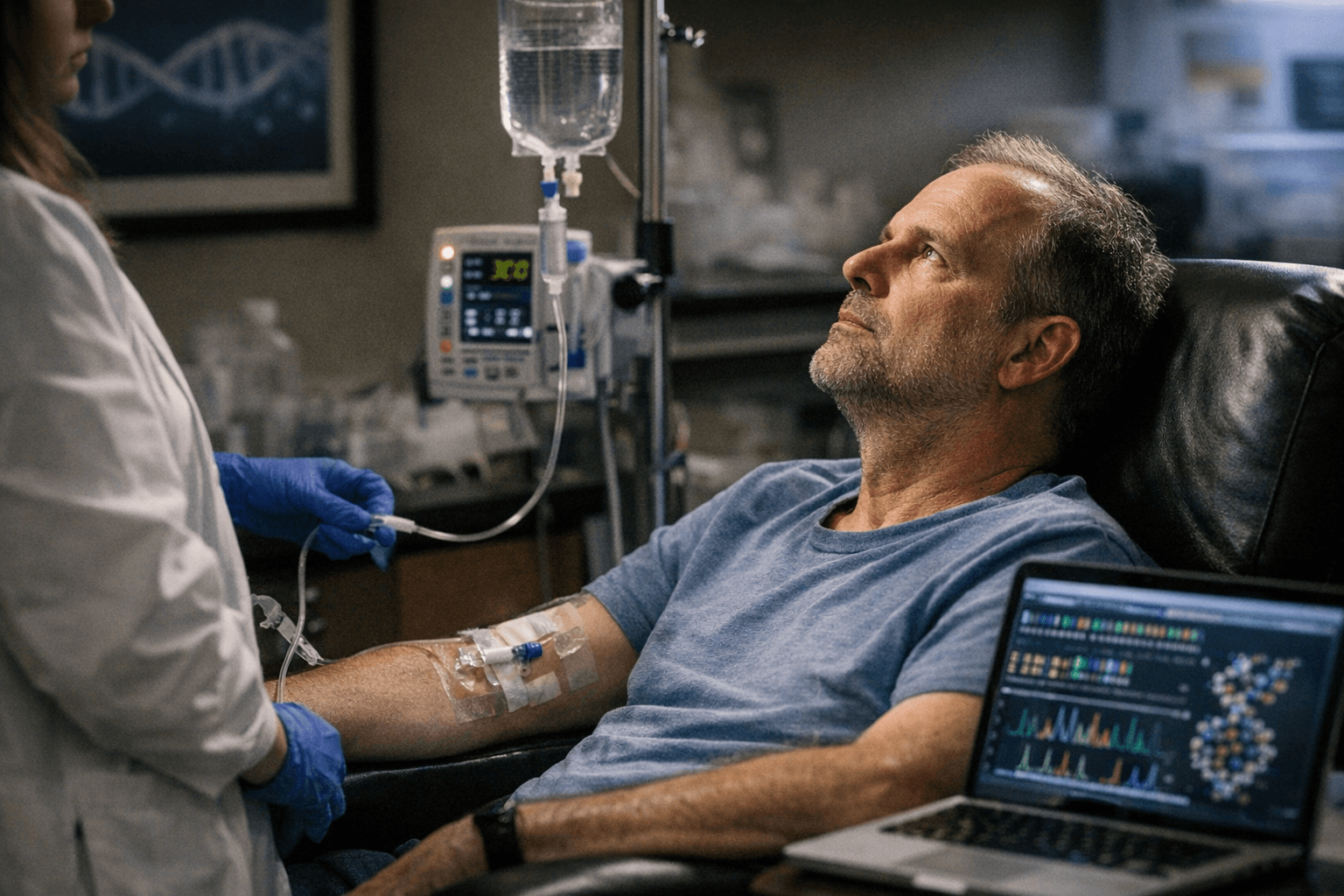
Jeff Vierstra has spent his career studying the molecular switches that turn genes on and off. Every few months for more than three years, that expertise has taken on a deeply personal dimension: he has been traveling to receive spinal infusions of an experimental drug designed to silence a mutated gene that made it likely he would develop ALS.
Vierstra, an investigator at the Altius Institute for Biomedical Sciences who researches gene regulation mechanisms, carries a pathogenic variant of the FUS gene, a mutation shared by two of his siblings. He enrolled in a clinical trial for ulefnersen, an antisense oligonucleotide developed by Ionis Pharmaceuticals in collaboration with Dr. Neil Shneider, director of Columbia University's Eleanor and Lou Gehrig ALS Center, before any symptoms of the disease appeared. As of mid-2025, he remained symptom-free.
His path to the trial began at a family Christmas gathering in Wisconsin in 2019. His oldest sister, Erin, mentioned she could not lift her neck during yoga. When she could not quickly find a neurologist, Jeff emailed a Columbia ALS researcher he had met at a genetics conference: Dr. Shneider himself. Shneider arranged for Jeff, Erin, and a third sibling, Leigh, to come to Columbia for genetic testing. All three tested positive for the FUS mutation.
The mutation is rare but catastrophic. FUS variants account for only 1 to 2 percent of all ALS cases, but they are the most common genetic driver of juvenile ALS, an aggressive form of the disease that can strike people younger than 25. ALS affects approximately 55,000 people across the United States, Europe, and Japan, with more than 40 genes linked to the disease. Up to 10 percent of cases have a known genetic basis; the remaining 90 to 95 percent arise sporadically.
Erin received ulefnersen for roughly three years but continued to slowly decline. Jeff, who began treatment before any symptoms emerged, represents a different clinical calculation: can silencing a disease-causing gene before neurodegeneration begins stop the disease entirely?
The drug carries the weight of another family's grief. It was originally developed for Jaci Hermstad, a 26-year-old Iowa woman whose identical twin sister, Alex, had died from FUS-ALS at age 17. Jaci was diagnosed with the same disease in February 2019. Shneider, whose FUS-targeting research in mice had been published in Nature Medicine, partnered with Ionis to develop the therapy for Jaci under compassionate use. She received her first dose just four months after diagnosis, but her disease had already advanced too far. Jaci Hermstad died in 2020, and the drug was named jacifusen in her memory before its later designation as ulefnersen.
Her case accelerated the science. In 2025, Shneider published a 12-patient case series in The Lancet documenting outcomes for FUS-ALS patients treated with ulefnersen. Two patients showed what the researchers called a "remarkable" or "unprecedented" response; one young woman who began receiving injections in late 2020 remained in good health. Most other symptomatic patients did not survive the aggressive disease, though Shneider noted that progression likely slowed for many, extending their life expectancy. Across the series, the therapy was found safe and well-tolerated, with no serious adverse events reported. Ulefnersen is now in a global, industry-sponsored Phase 3 trial led by Shneider and co-funded by the ALS Association.
The presymptomatic approach Vierstra represents has a parallel in the ongoing ATLAS trial, which is testing tofersen, targeting SOD1-linked ALS (the first ALS gene, discovered in 1993), in mutation carriers before symptoms appear. For Vierstra, the logic of enrolling in a clinical trial before illness takes hold is not abstract. At age 16, he was diagnosed with leukemia and treated through a clinical trial; when the cancer returned, a bone marrow transplant cured it.
What FUS patients can teach medicine extends beyond the narrow slice of ALS they represent. "By comparing these ultra-rare patients and their response to individualized therapy, we hope to learn something about the biology of the disease that will eventually help a larger percentage of ALS patients," Shneider said. Vierstra, still symptom-free, is living evidence of what catching that biology early enough might make possible.
Sources:
Know something we missed? Have a correction or additional information?
Submit a Tip

