Surprise billing law spawns multibillion-dollar dispute industry for doctors
A law meant to stop surprise bills now sends hundreds of thousands of cases into arbitration, where providers win most disputes and awards can top Medicare by multiples.

The No Surprises Act was supposed to shield patients from the shock of out-of-network bills. Instead, it helped create a fast-growing arbitration business that has delivered huge payouts to some doctors and medical groups, with costs that could ripple back into premiums and overall health-care spending.
Congress passed the law in 2020, and it took effect in 2022. To keep patients out of the middle, it banned many surprise out-of-network charges and set up a federal independent dispute resolution process for insurers and providers that could not agree on payment after an open-negotiation period. The federal portal launched on April 15, 2022, and the government has since posted quarterly public-use files covering calendar years 2023 and 2024, plus 2025’s first two quarters.

The law has clearly helped patients avoid some of the worst billing abuses. A Health Affairs review said extrapolations from recent data suggest the No Surprises Act protected Americans from more than 25 million surprise medical bills. But the same system has also become an unusually lucrative arena for providers. KFF found that about one in eight disputes in the first year of federal arbitration ended in a payment determination. By mid-2024, nearly two in three disputed services involved emergency room care, and the top 10 parties initiating disputes were all providers or billing consultants. The top three, all backed by private equity, accounted for 53% of payment disputes from the start of 2023 through mid-2024.
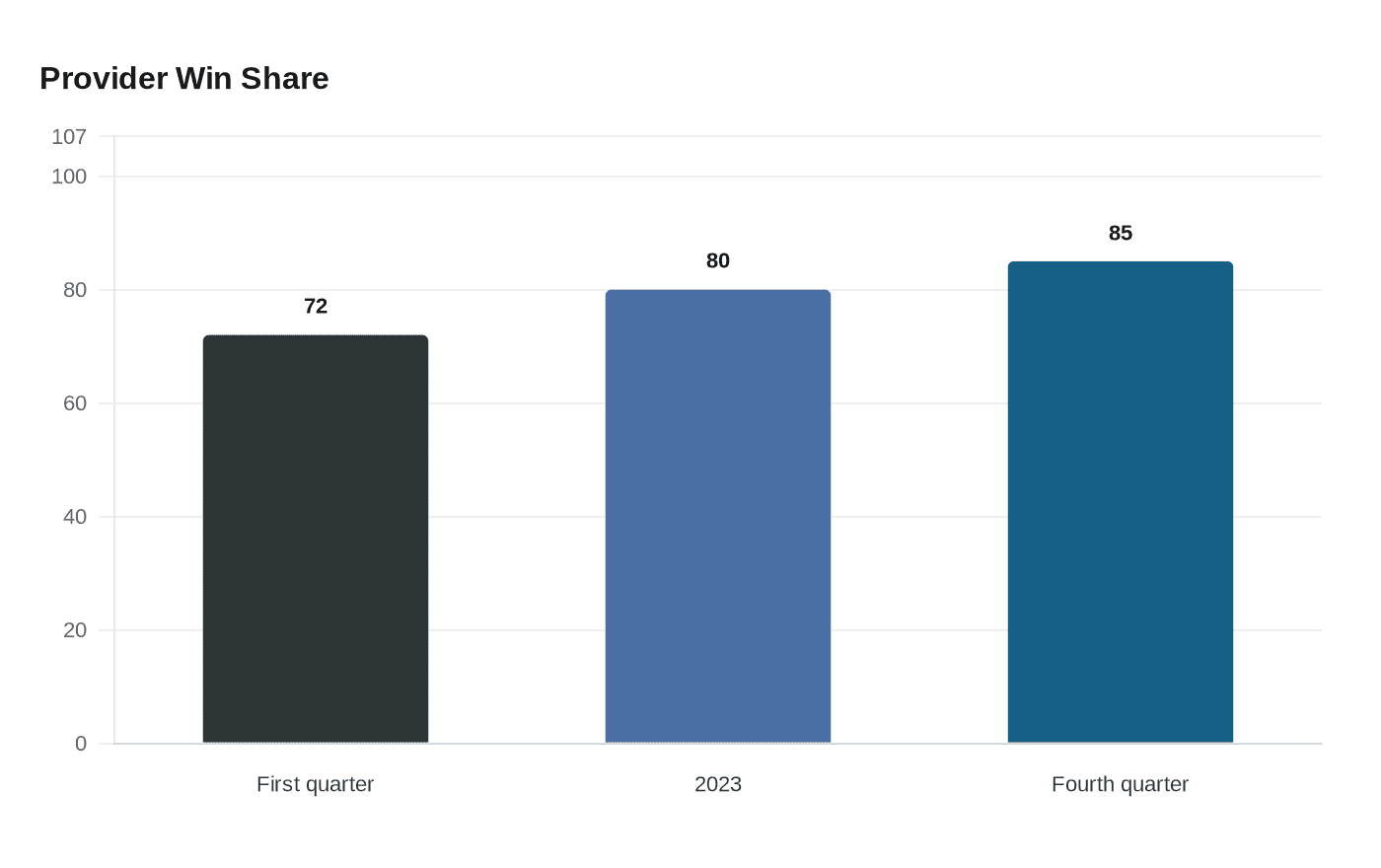
The volume has been staggering. Health Affairs reported 657,040 new cases filed in 2023, with roughly 70% tied to four private-equity-backed organizations: TeamHealth, SCP Health, Radiology Partners and Envision. About half of those cases came from Texas, Florida, Tennessee and Georgia. Providers also prevailed often once disputes were resolved, winning 80% of challenges in 2023. Their share of wins climbed from 72% in the first quarter to 85% in the fourth quarter. In some service categories, the median arbitration decision was at least 3.7 times what Medicare would pay, and one 2024 analysis found median awards above 300% of contracted in-network rates.
Those payouts have drawn sharp criticism from policymakers and insurers who say the system is no longer a rare backstop but a business model. Health Affairs found 586,581 cases filed in the first half of 2024 alone, nearly matching all of 2023, though some of that surge may have reflected portal suspensions. CMS has since kept expanding the machinery, adding Dane Street, LLC as a 16th certified IDR entity in January 2026 and announcing in March that the process would shift to a new IDR Gateway later in 2026. The law that was meant to protect patients has become a major battleground over who profits from out-of-network care, and who ultimately pays.
Know something we missed? Have a correction or additional information?
Submit a Tip

