Trump administration exempts foreign doctors from visa freeze, averting departures
A quiet exemption spared foreign doctors from a visa freeze that had threatened staffing in rural hospitals, primary care clinics and residency programs across the country.

The Trump administration quietly carved foreign physicians out of a visa-processing freeze that had threatened to push doctors out of hospitals and clinics in underserved parts of the United States. Late last week, U.S. Citizenship and Immigration Services updated its website to say applications tied to medical physicians would keep moving, and the Department of Homeland Security later confirmed that physician-related cases would resume.
The reversal came after a broader policy had frozen processing of visa extensions, work permits and green cards for citizens of 39 countries, a move that hit foreign-trained medical workers from Africa, the Middle East and Venezuela. For hospitals already struggling to keep shifts covered, the exemption averted a sudden loss of clinicians in places that rely heavily on international medical talent.

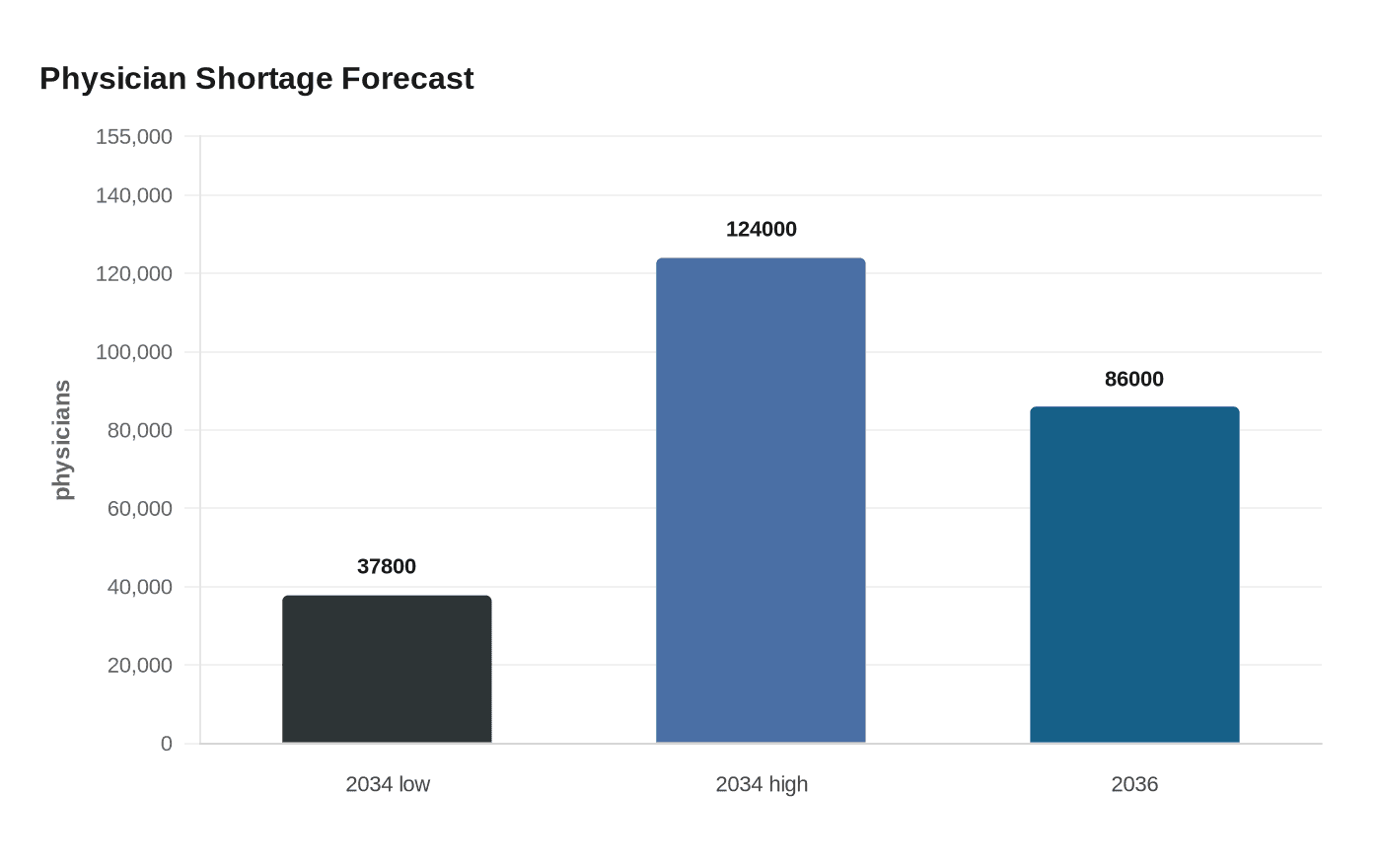
The stakes are high because the country’s physician pipeline is already stretched. The Association of American Medical Colleges has projected a shortage of between 37,800 and 124,000 physicians by 2034, and later said the gap could reach 86,000 physicians by 2036. Roughly 1 in 5 active U.S. physicians were born and attended medical school outside the United States or Canada, according to the AAMC. The American Medical Association says international medical graduates are concentrated in primary care and in health professional shortage areas, exactly the settings that absorb the hardest-to-fill openings.
That means more than 60% of foreign physicians work in primary care fields such as family medicine, internal medicine and pediatrics. Those are the doctors who keep rural clinics open, staff community health centers and help safety-net hospitals maintain round-the-clock coverage. A freeze that delays renewals or blocks work authorization can ripple quickly through small communities where a single vacancy can leave entire patient panels scrambling for care.

The disruption did not start with this year’s freeze. In 2025, the administration slowed new interview appointments for many J-1 visas, the category used by most international medical residents, and hospitals reported gaps when doctors could not arrive in time for July 1 residency start dates. Residency programs depend on that summer turnover; when incoming residents are delayed, the pressure lands on overextended attendings, nurses and emergency departments.
Medical groups pushed back fast. On April 8, more than 20 doctor organizations urged federal officials to create a national-interest exemption for qualified, vetted physicians. Dr. Rebecca Andrews, the board chair of the American College of Physicians, welcomed the reversal.
The episode laid bare a recurring tension in federal immigration policy: hard-line restrictions may satisfy a political promise, but in medicine they can also threaten the staffing that keeps primary care, residency training and hospital services running in communities that already have too few doctors.
Know something we missed? Have a correction or additional information?
Submit a Tip

