U.S. funding cuts cripple South Africa HIV programs ahead of new drug rollouts
South Africa received its first 37,920 doses of lenacapavir as U.S. aid cuts shuttered clinics, ended outreach and left 8,493 HIV workers without jobs.

South Africa received its first 37,920 doses of lenacapavir just as the network meant to deliver HIV prevention was being dismantled by U.S. funding cuts, leaving clinics closed, outreach curtailed and patients harder to reach across the country with the world’s largest HIV burden.
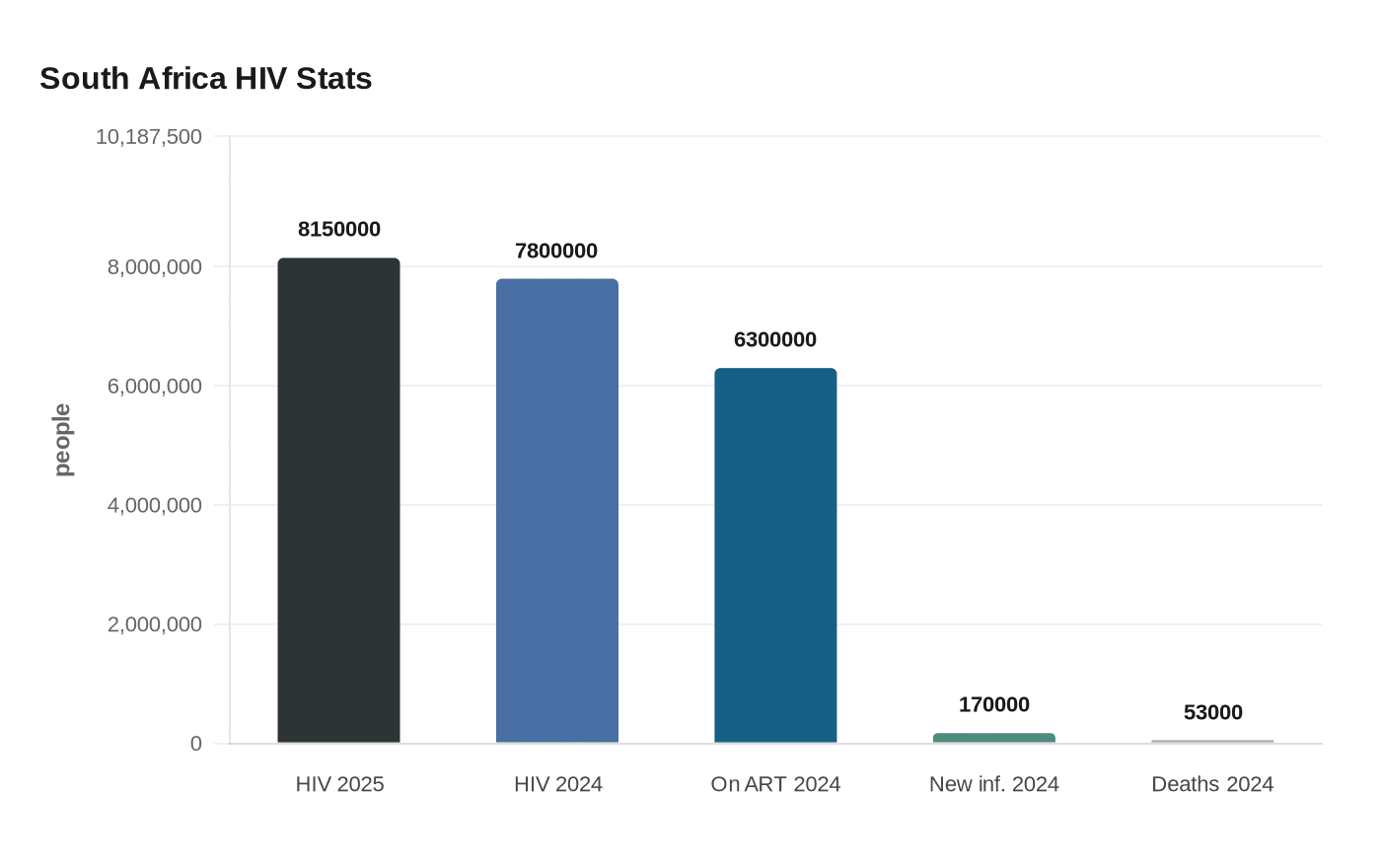
The contradiction is stark. South Africa still had about 8.15 million people living with HIV in its 2025 statistical release, and UNAIDS estimated 7.8 million in 2024. Even with 6.3 million people on antiretroviral therapy in 2024, the country recorded about 170,000 new infections and 53,000 AIDS-related deaths that year, underscoring how much prevention still matters.
That prevention system took a direct hit after the February 2025 U.S. funding freeze. UNAIDS said about 40 USAID-funded health projects in South Africa received termination letters on Feb. 26, and about 8,493 PEPFAR-funded staff involved in HIV response activities stopped providing services. Clinics closed or sharply reduced HIV testing, care, treatment, mobile outreach, drop-in centers and data management, erasing layers of support that had taken years to build.
The funding gap was not minor. UNAIDS said the freeze left South Africa facing a 17% HIV funding shortfall from the United States, while the private sector contributes only about 2% to the country’s HIV response. Physicians for Human Rights, which produced the report, argued that Washington had effectively wasted years of investment by abandoning the research infrastructure and community health systems it had helped build.
The consequences are already visible in communities that depend on outreach and peer-led services. Yvette Raphael of Advocates for the Prevention of HIV in South Africa said many LGBTQI communities, sex workers and young people are not accessing services because of the disruptions. The report also points to weakened data collection, which makes it harder for public-health officials to see where testing, diagnoses and outreach gaps are widening.
At the same time, the World Health Organization recommended injectable lenacapavir for HIV prevention on July 14, 2025, giving South Africa a powerful new twice-yearly PrEP option just as its delivery system was fraying. Emily Bass, a co-author of the report, put the problem plainly: "We have a product that's really powerful, but we don't have a programme to fit it into anymore."
South Africa’s health department said on April 7, 2026, that the first batch of lenacapavir had arrived and that rollout would be phased, with priority groups including adolescent girls and young women, sex workers and men having sex with men. A 2025 government plan reported by Bhekisisa said the drug could reach more than 300 government clinics between April 2026 and March 2028, backed by R513 million from a Global Fund grant, with South Africa among nine early-adopter countries.
The health department has cast lenacapavir as part of its 2026-2030 HIV strategy and a tool to help end AIDS as a public health threat by 2030. But without the outreach workers, clinic staff and data systems that once linked prevention to the people most at risk, the drug’s arrival may not reach the communities that need it most.
Know something we missed? Have a correction or additional information?
Submit a Tip

