Mindfulness Helps Nursing Students Reduce Stress, Build Resilience, Avoid Burnout
With 65% of nursing students and interns reporting high burnout, mindfulness is showing up as a practical stress tool, not a wellness buzzword.

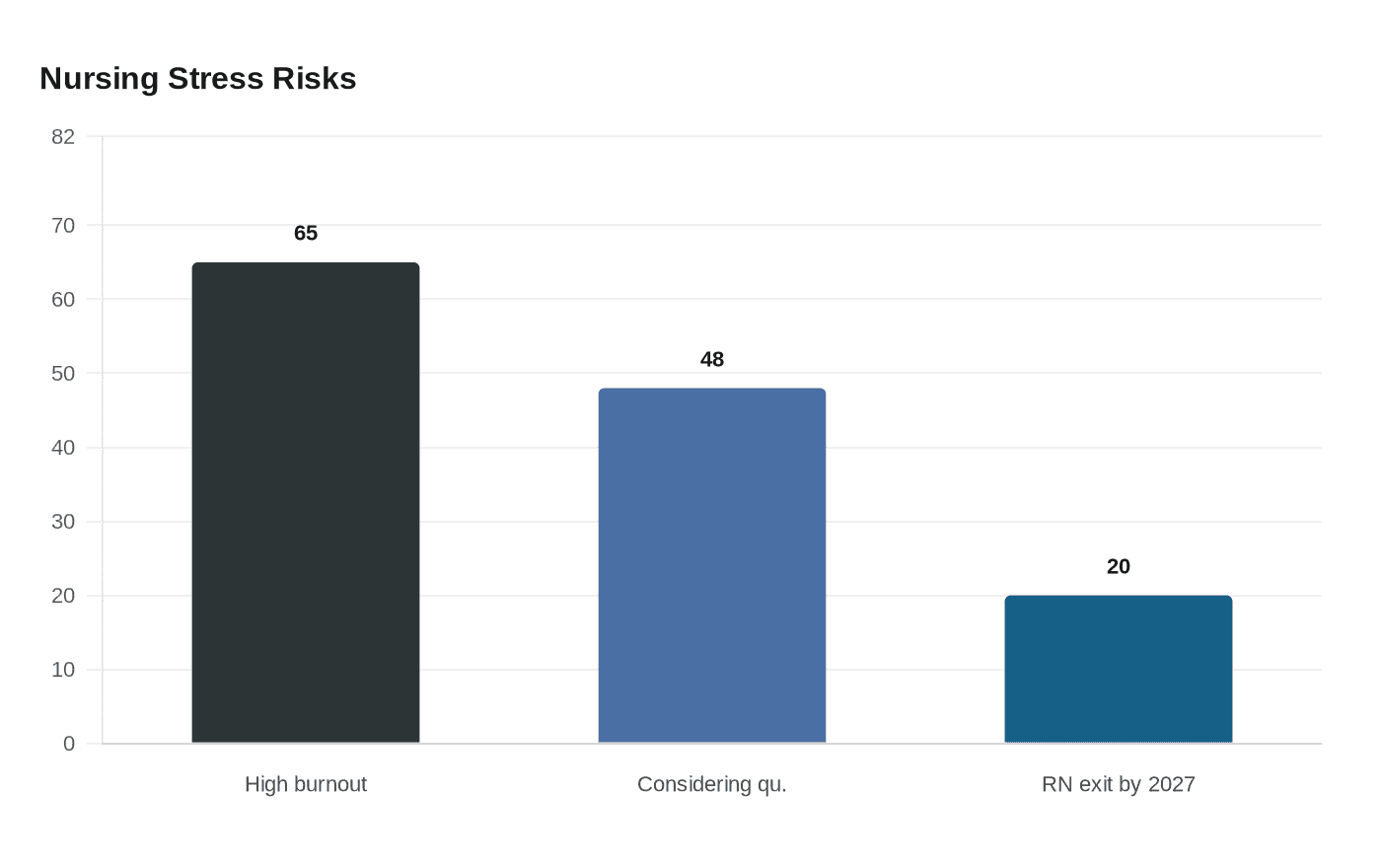
Nursing school can feel like a pressure cooker, and the most compelling thing in the mindfulness research is not a vague promise of calm. It is the hard number that should stop every dean and clinical coordinator in their tracks: in one study of 564 nursing students and interns, 65% reported high burnout, and 48% of clinical-level students were considering quitting their nursing program.
Why this matters in the nursing pipeline
That kind of strain lands in a profession already under siege. The American Association of Colleges of Nursing says the United States is projected to face a shortage of registered nurses that will intensify as Baby Boomers age and health-care needs grow, while nursing schools are still struggling to expand capacity to meet demand. Add the National Council of State Boards of Nursing estimate that about 100,000 registered nurses left the workforce during the COVID-19 pandemic because of stress, burnout, and retirements, plus its projection that about one-fifth of RNs nationally could leave the health-care workforce by 2027, and the student experience starts looking like a workforce issue, not just an academic one.
That is why mindfulness is being studied here with more urgency than usual. Nursing students are not just stressed out learners, according to a 2024 nursing-education paper, they are an integral part of the future workforce and are at high risk of burnout and increased perceived stress. If they burn out early, the pipeline leaks before those students ever reach patient care.
What the evidence actually shows
The strongest nursing-specific review in the notes, a 2023 systematic review and meta-analysis of mindfulness-based interventions in nurses, pulled together 15 studies with 1,165 randomized participants. Its main finding was straightforward: mindfulness produced moderate post-intervention reductions in stress. In that analysis, the effects on anxiety and depression were not significant, which matters because it keeps the story honest. Mindfulness was not a cure-all, but it did move the stress needle.
A more recent integrative review focusing on nursing students paints a slightly broader picture. It links mindfulness-based interventions with reduced stress, anxiety, depression, and burnout, but the effects were mainly short term. That detail is the real practical takeaway for schools and training programs: a one-off wellness workshop is probably not enough if the goal is to support students through repeated clinical demands, exam blocks, and emotional overload.
The wider student literature points in the same direction. A review of randomized controlled trials in college students found positive effects on depression, anxiety, stress, and sleep quality. That does not replace nursing-specific evidence, but it reinforces the same core idea: mindfulness works best as a real intervention with a schedule, not as a slogan.
What seems to change when mindfulness is used well
The most useful way to think about mindfulness in nursing education is as a recovery and regulation tool. The research summary points to improvements in emotional regulation and coping skills, and that is the kind of benefit that matters when a student is bouncing between coursework, simulation labs, and clinical rotations. It is less about becoming serene and more about staying usable under pressure.
That is also why the best framing is practical, not aspirational. Mindfulness helps students recover between shifts, steady attention before exams, and avoid burning out over the long path into the profession. The best version of it is low-friction and repeatable, something that fits into an already crowded academic day instead of adding another obligation to a packed calendar.
The real test is whether the practice can be embedded where stress actually happens. That means labs, clinical placements, and study routines, not an abstract self-care ideal that only works when life is already calm. When mindfulness is placed inside the training environment, it becomes easier to use as a reset after a hard patient interaction, before a skills check-off, or during the mental churn of exam week.
Why the short-term result still matters
It is tempting to dismiss short-term gains, but in nursing education short-term may be exactly where the leverage is. If a student gets through a brutal semester with better coping, lower stress, and less emotional drain, that can affect attendance, performance, and whether they stay in the program. For a field fighting both shortages and enrollment challenges, that is not a minor outcome.
AACN said in April 2024 that enrollment in baccalaureate and graduate nursing programs continued to be a challenge at U.S. schools of nursing, which makes retention just as important as recruitment. The question is not only how to attract students into nursing, but how to keep them steady enough to finish. In that context, mindfulness looks less like a perk and more like a support layer for the pipeline.
That is also where the ongoing research matters. The University of Michigan and WellNurse protocol work underscores that nursing students sit at the center of future workforce planning and high stress. The names tied to this growing conversation, including Kelley Strout, Robert Rosseter, Qi Wang, Fang Wang, Shurong Zhang, Chaofan Liu, Yue Feng, Junzhu Chen, and Tara Malone, reflect how broad the interest has become across nursing education and workforce research.
Could this model work in other high-pressure training programs?
Probably yes, especially in settings where people are learning while carrying real emotional and cognitive load. The nursing data suggest the important ingredients are not fancy: a repeatable practice, built into the day, aimed at stress regulation and coping rather than perfection. That logic should translate well to other training-heavy fields where burnout starts before the diploma does.
The lesson from the nursing literature is clear: mindfulness is most credible when it is treated as routine support, not a one-time wellness event. If schools and hospitals want better resilience, better attention, and fewer students slipping out of the pipeline, the smartest move is to put the practice where the pressure already lives.
Know something we missed? Have a correction or additional information?
Submit a Tip

