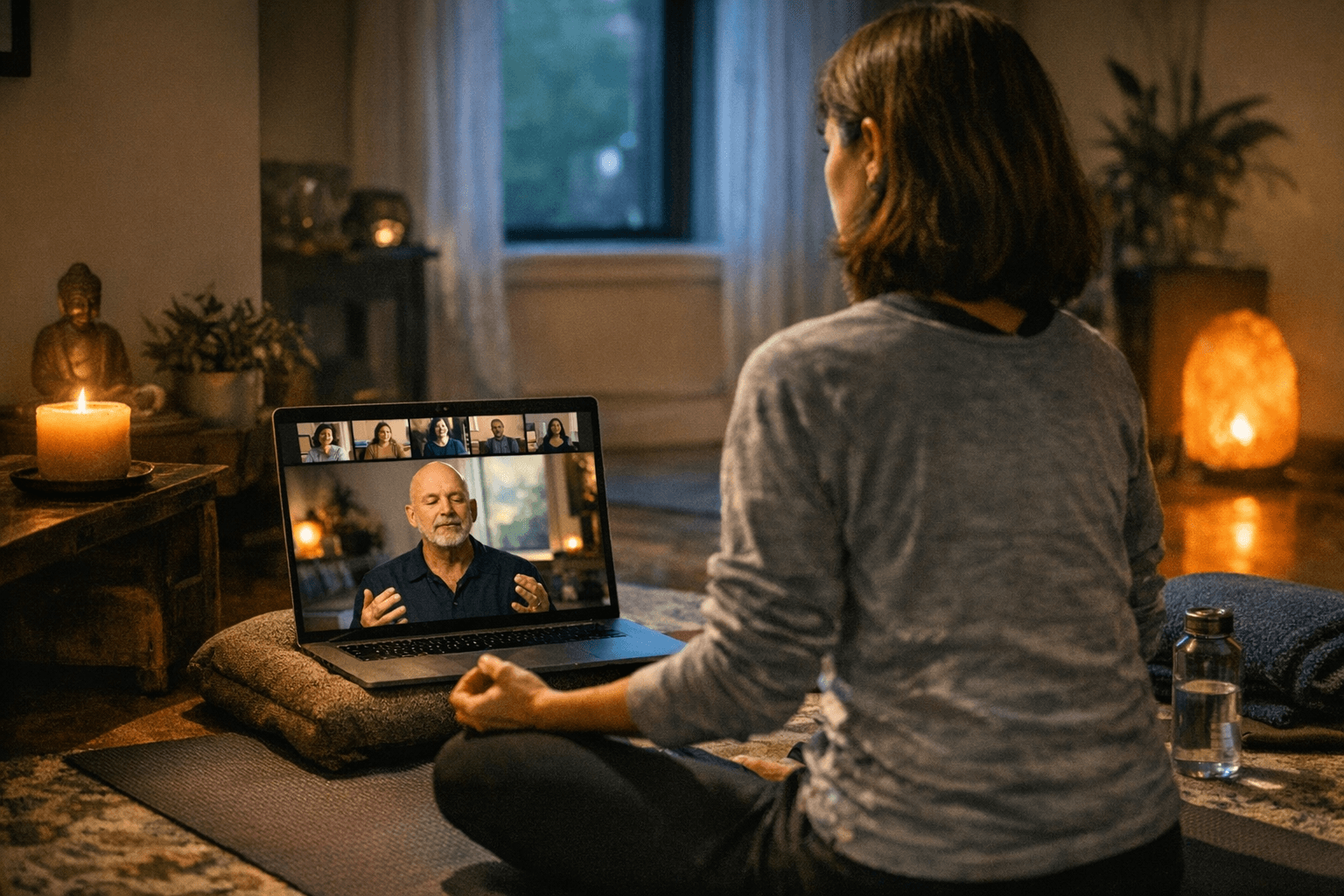
Mindfulness Reduces Burnout and Stress in Fever Clinic Nurses, Study Finds
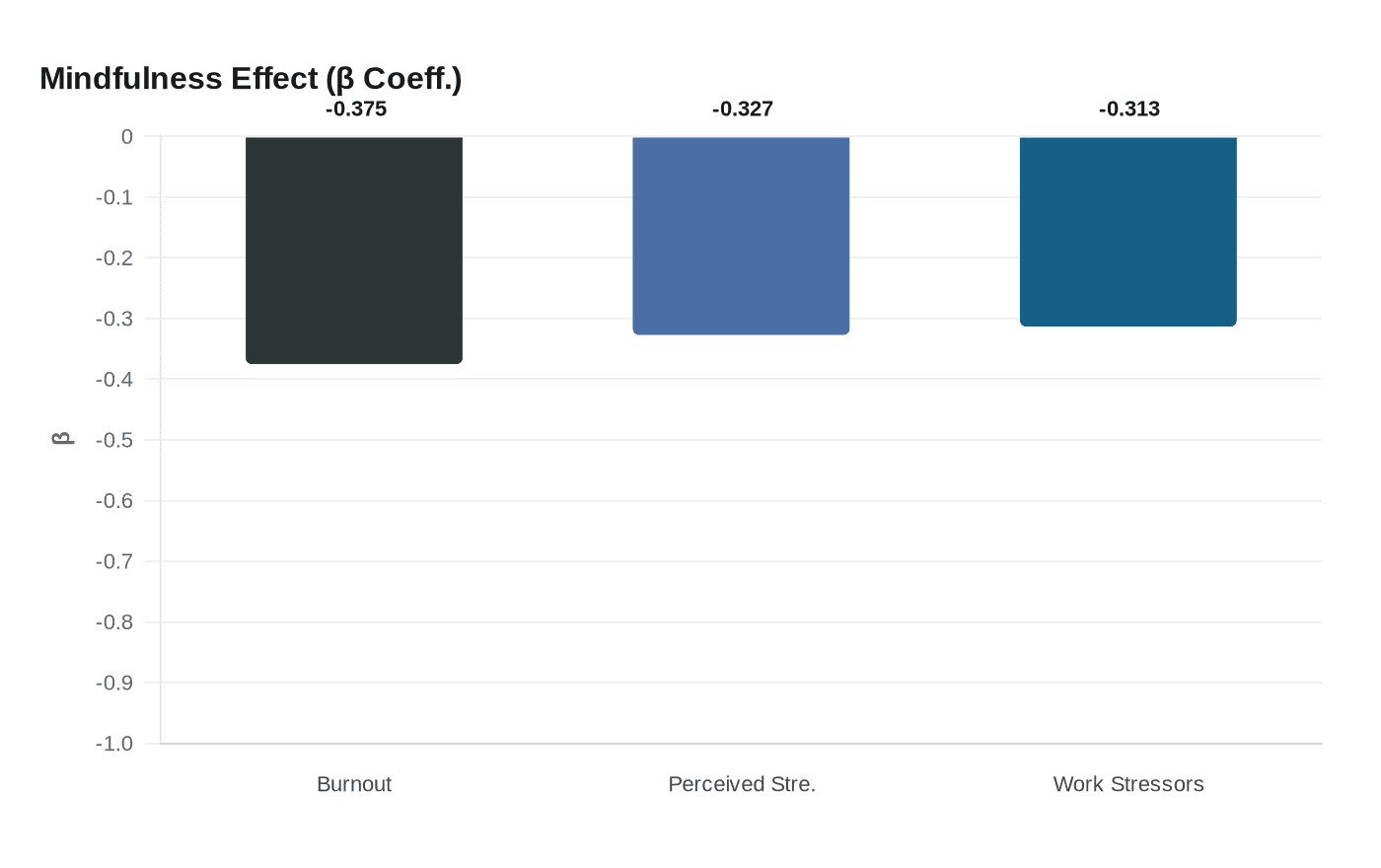
A path coefficient of β = −0.375 links trait mindfulness to lower burnout in fever clinic nurses, with workload and time pressure identified as the primary stressors.

A structural equation model tracking 375 fever clinic nurses found that higher trait mindfulness predicted significantly lower burnout, with a path coefficient of β = −0.375. The same model placed mindfulness's negative effect on perceived stress at β = −0.327 and on workplace stressors at β = −0.313, suggesting that moment-to-moment attentional awareness shapes how nurses experience pressure from multiple directions simultaneously.
The study was published April 4, 2026 in Humanities and Social Sciences Communications, led by Dandan Zhang alongside co-authors Yongjun Chen, Yitong Jia, Qingqing Liao, Lichun Huang and Shuangyan Yi. Participants completed validated Chinese-language instruments between July 1 and September 30, 2022, including the Maslach Burnout Inventory, the Chinese Perceived Stress Scale, the Mindful Attention Awareness Scale (MAAS) and a custom Stress Source Scale. Workload and time pressure ranked as the primary stressors reported across the sample.
Pearson correlations revealed that mindfulness carried its sharpest protective association with emotional exhaustion (r = −0.344, p < 0.01) and with reduced personal accomplishment (r = −0.298, p < 0.01), two of the three core dimensions of the Maslach burnout framework. All structural equation modeling effects cleared the p < 0.001 threshold.
What the MAAS actually measures is not meditation frequency but moment-to-moment attentional awareness during ordinary activity: noticing sensations, noticing emotional tone, catching when the mind has drifted into rumination. That specificity points directly to short, practicable interventions. A 60-to-90-second body scan between patient rooms, naming three physical sensations before opening the next chart, targets exactly the attentional register the scale captures. A one-minute breathing anchor at a natural handover point requires no setup: observe the breath without controlling it, locate the present. A 90-second end-of-shift body check, explicitly labeling accumulated tension as workload stress rather than personal failure, addresses the reduced-personal-accomplishment dimension the correlations flagged most sharply.
Each of those practices maps most cleanly onto nurses, but the β coefficients apply broadly to any high-demand shift environment where workload compression and time pressure are the dominant stressors, a description that fits emergency medicine, overnight logistics operations and acute care settings well beyond fever clinics.
The findings carry a methodological ceiling Zhang and co-authors stated plainly: cross-sectional data establish correlation, not causation. The pandemic context of mid-2022 also limits direct extrapolation to non-crisis conditions. The authors recommended pairing any mindfulness-based program with structural reforms including revised staffing ratios, adjusted schedules and workload management, framing individual resilience training as complement rather than substitute for organizational change.
The path coefficients offer administrators a concrete reference point: mindfulness's β of −0.375 on burnout operated independently alongside measured workplace stressor levels, not instead of them.
Know something we missed? Have a correction or additional information?
Submit a Tip