Yoga Self-Efficacy Linked to Mindfulness, Body Appreciation, Fewer Eating Disorder Symptoms
UCSF researchers found yoga self-efficacy mattered most, driving mindfulness, self-compassion and body appreciation while easing eating-disorder symptoms.

The most useful takeaway for yoga teachers and anyone in recovery is not that yoga helps, but how it helps: confidence in practice appears to be the key link. In a UCSF mediational model using Hayes PROCESS Model 6, yoga self-efficacy predicted lower body dissatisfaction and fewer eating-disorder symptoms by first strengthening mindfulness, then self-compassion and body appreciation.
That pattern mattered in a sample of 174 college students with previous yoga experience, whose mean age was 20.10 years with a standard deviation of 2.49. The analysis found significant mediation pathways, with p values of .012 and less than .0001. In practical terms, the study suggests that the therapeutic value of yoga in eating-disorder recovery may come less from simply doing poses and more from helping students feel capable enough to stay present, notice internal states and build a less hostile relationship with the body.
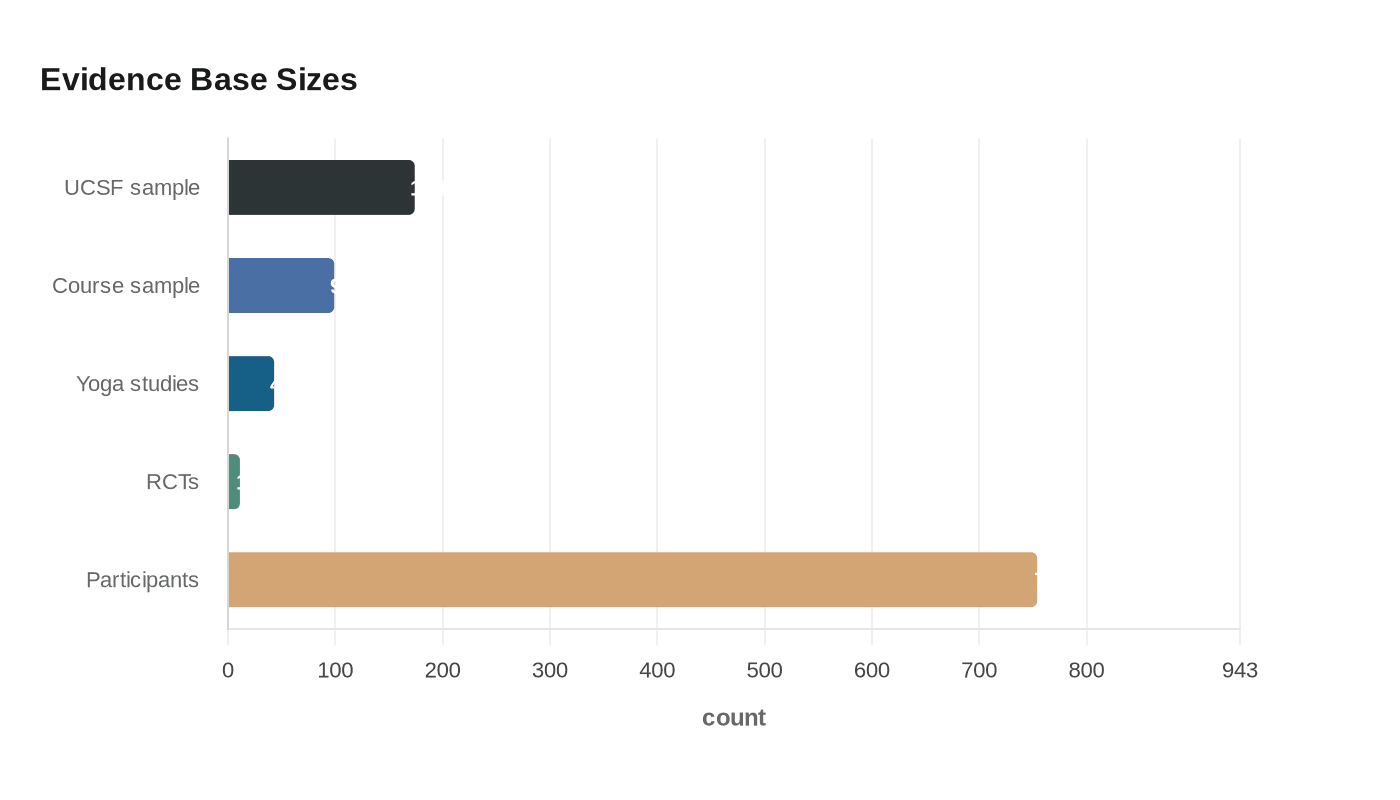
The findings sharpen a conversation that has been building for years inside this research area. A 2020 university yoga-course study followed 99 students through an eight-week program meeting three times a week for 50 minutes. By the end of the course, participants showed lower body dissatisfaction and eating-disorder pathology, along with higher body appreciation, self-compassion and yoga self-efficacy. That earlier work also showed some gender differences, including greater reductions among men in overweight preoccupation and greater improvements in appearance evaluation.
The broader evidence base points in the same direction. A 2020 review and meta-analysis that pulled together 43 yoga studies, including 11 randomized controlled trials with 754 participants, found a small significant effect on global eating-disorder psychopathology, a moderate-to-large effect on binge eating and bulimia, and a small effect on body image concerns. It did not find a statistically significant effect on dietary restraint.
For the field, the message is clear: if yoga is going to play a role in prevention or treatment, the design of the practice matters. The UCSF Eating Disorders Program says it serves patients ages 10 to 25 and has delivered specialized care for more than 30 years, with integrated medical, psychological and nutrition services. Its Reilly Lab says its mission is to improve treatments for people struggling with eating disorders and anxiety. This study adds a sharper target for yoga-based care, putting self-efficacy at the center of the path toward mindfulness, self-compassion and body appreciation.
Know something we missed? Have a correction or additional information?
Submit a Tip