Enhanced ACA Subsidies Expire Jan. 1, 2026 - Premiums Projected to Soar
Enhanced premium tax credits that had substantially lowered Affordable Care Act marketplace premiums expired as 2026 began, leaving more than 20 million enrollees exposed to much higher costs unless Congress intervenes. Analysts warn the lapse could more than double average premiums for subsidized consumers and prompt millions to drop coverage, with state relief plans only partially offsetting the shock.
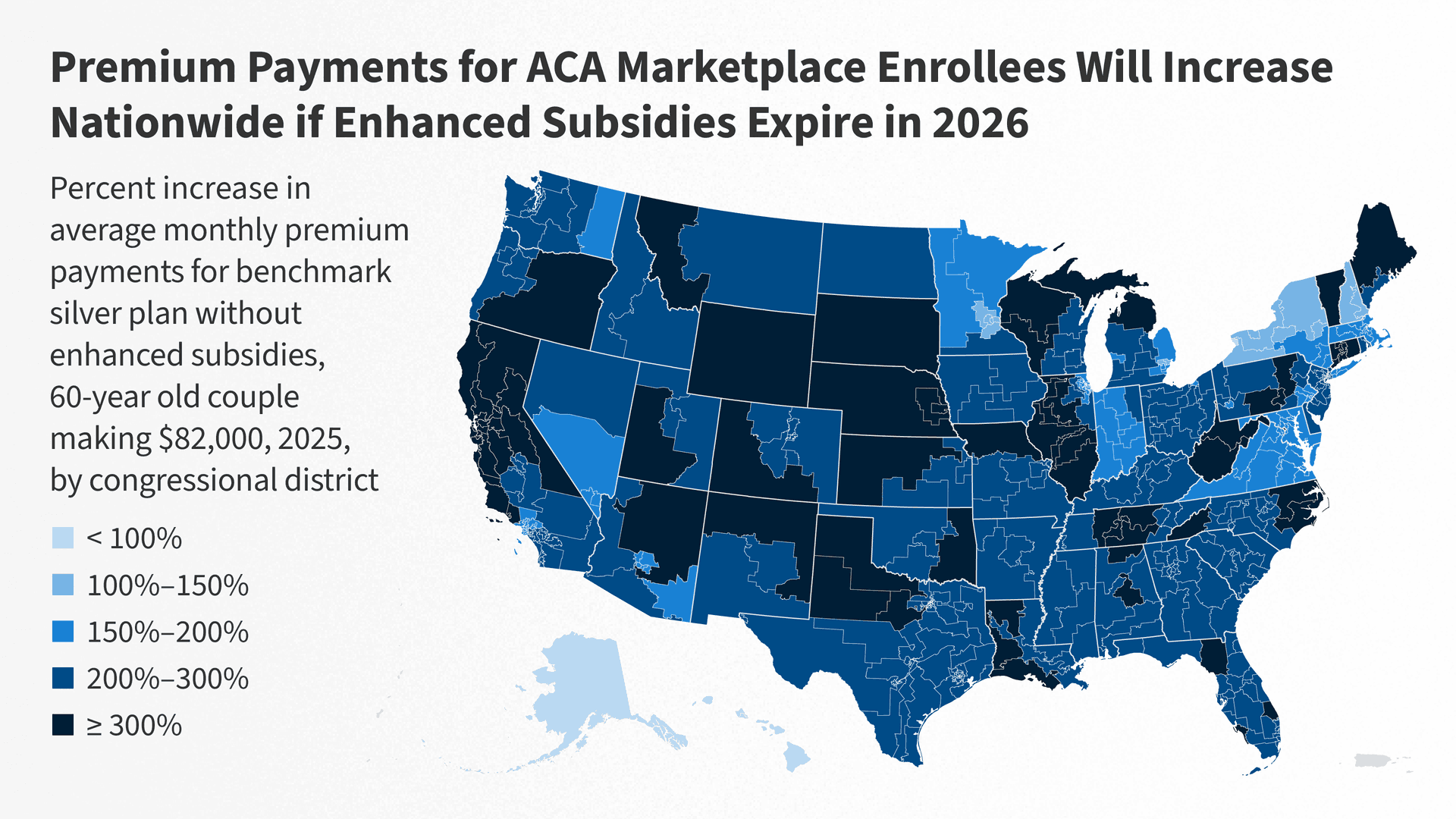
Enhanced premium tax credits for Affordable Care Act marketplace enrollees expired at midnight as 2026 began, ending a temporary program first introduced during the pandemic and extended through 2025 by earlier legislation. The lapse removes an extra layer of subsidies that had sharply reduced monthly and annual premiums for many low- and middle-income Americans.
The Kaiser Family Foundation projects that, if the enhanced credits remain unavailable, the average annual premium paid by subsidized enrollees will more than double, rising from $888 in 2025 to $1,904 in 2026. That 114 percent increase represents roughly a $1,016 jump in average annual cost for subsidized consumers. More than 20 million marketplace enrollees receive subsidies, meaning the change affects a large share of exchange shoppers nationwide.
Analysts say the financial shock could quickly reshape enrollment. An analysis by the Urban Institute and the Commonwealth Fund estimates that higher premiums tied to the subsidy rollback could prompt about 4.8 million Americans to drop marketplace coverage in 2026. Observers expect younger and healthier people to be the most likely to disengage first, leaving a relatively older and sicker enrollee pool that could exert upward pressure on premiums for those who remain.
Final enrollment totals remain uncertain because open enrollment is still under way in many states through Jan. 15, allowing some consumers time to reassess plan choices or enroll despite higher sticker prices. Shoppers who qualify for some remaining post-expiration assistance will face smaller subsidies with an income eligibility cutoff; for 2026 that cutoff is at roughly four times the federal poverty level, about $62,600 for an individual and $84,600 for a couple, narrowing the pool of people who continue to receive aid.

States have moved to blunt the immediate impact, but relief is limited. California has allocated $190 million to replace enhanced subsidies for many of its lowest-income enrollees in 2026, a fraction of the roughly $2.5 billion in federal enhanced subsidies that California enrollees received in 2025. Other states have signaled targeted efforts, but funding gaps at the state level are expected to leave many households facing significant premium increases.
Employers and labor market observers say rising ACA premiums could shift worker demand toward employer-sponsored plans and complicate hiring for positions that do not include benefits. For businesses that already struggle to offer coverage, the change could intensify recruitment and retention pressures.
Whether Congress will move to restore the enhanced credits remains uncertain. Without legislative action this year, the lapse will stand and the marketplace will enter 2026 with steeper costs for subsidized consumers, heightened risk of coverage loss for millions, and an unsettled enrollment picture to be clarified by mid-January.
Know something we missed? Have a correction or additional information?
Submit a Tip

