FDA Approves IsoPSA Blood Test, Aids Prostate Biopsy Decisions
The U.S. Food and Drug Administration granted Premarket Approval on December 1, 2025 for Cleveland Diagnostics' IsoPSA in vitro diagnostic kit. The blood based test is intended to help clinicians decide whether men aged 50 and older with elevated PSA should undergo prostate biopsy, a development that could reduce unnecessary procedures and influence screening and coverage decisions.
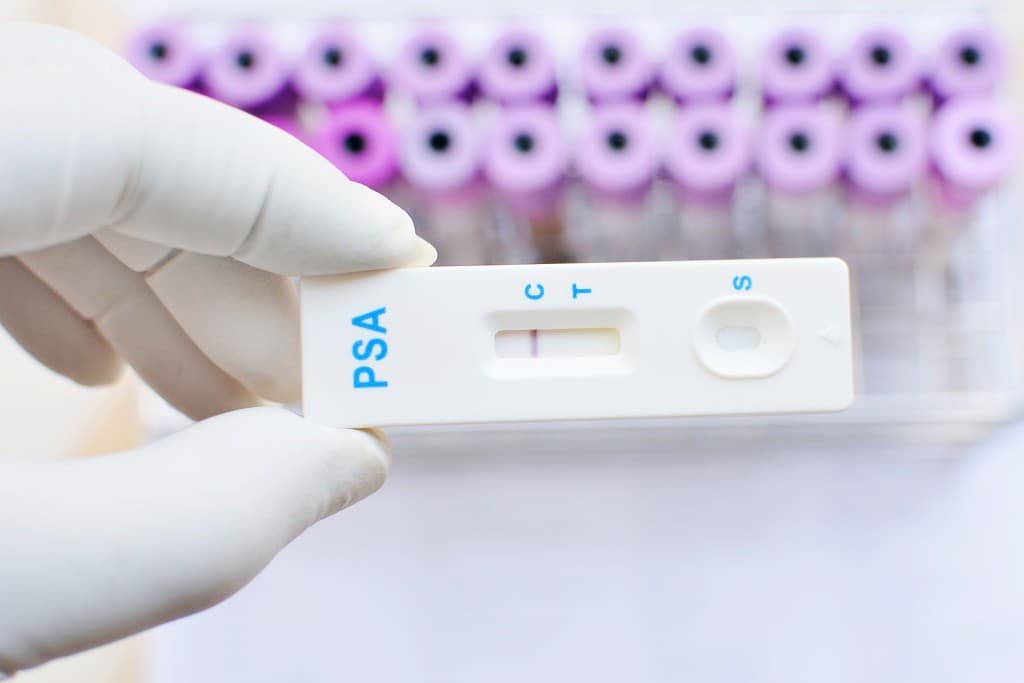
The Food and Drug Administration on December 1 granted Premarket Approval to Cleveland Diagnostics for IsoPSA, a blood based in vitro diagnostic intended to guide biopsy decision making for men aged 50 and older with elevated prostate specific antigen. The company said the clearance was based on a large prospective multi center clinical study together with analytical validation studies performed across 14 U.S. sites, and it referenced full clinical data appendices in its announcement.
Premarket Approval is the agency's most stringent pathway for medical devices and diagnostics, requiring demonstration of safety and effectiveness. For clinicians and patients, the IsoPSA decision support test promises to refine a common clinical crossroads. Many men with elevated PSA face a choice between surveillance and prostate biopsy, an invasive procedure that can carry pain, bleeding and, in some cases, serious infections. Cleveland Diagnostics said the test could reduce unnecessary biopsies while improving early detection of clinically significant prostate cancer.
Public health experts greeted the approval as potentially meaningful but urged measured adoption. A blood based biomarker that reliably distinguishes aggressive disease from indolent conditions could limit harms from overdiagnosis and overtreatment, saving health systems money and reducing patient exposure to procedure related complications. At the same time, independent review of the clinical data will be essential to determine the test's performance across diverse populations and care settings.
Equity and access will determine whether potential benefits reach communities that bear the heaviest burden of prostate cancer. Black men in the United States experience higher incidence and mortality from prostate cancer than other groups, and men in rural or low income areas often face delayed diagnosis because of limited specialty care. A readily deployable blood test could expand access in primary care and community clinics, but experts cautioned that coverage and cost barriers could limit uptake if payers do not establish reimbursement policies quickly.
Policy implications extend to payers, guideline committees and federal programs. With PMA in hand, Cleveland Diagnostics is positioned to pursue reimbursement discussions with commercial insurers and Medicare, which often look to regulatory determinations when setting coverage. Clinical societies and screening guideline panels will also weigh the new evidence as they consider recommendations for men with elevated PSA.
Advocates called for transparency and further evaluation. The company referenced detailed clinical appendices and industry reporting provided regulatory context, but independent reassessment and peer reviewed publication of the trial results will help clinicians and policymakers judge reliability across age groups and racial and ethnic subgroups. Without equitable coverage strategies and targeted community engagement, a promising diagnostic could fall short of reducing disparities.
The FDA clearance marks a regulatory milestone for blood based prostate diagnostics. Whether that milestone translates into broader public health gains will depend on how rapidly clinicians adopt the test, how payers respond on reimbursement, and how well public health efforts ensure access for the patients most at risk.
Sources:
Know something we missed? Have a correction or additional information?
Submit a Tip

