Genetics, Not Lifestyle, May Be the Bigger Key to a Long Life
New science suggests your grandmother's lifespan may predict yours better than your diet, as genetics increasingly emerges as the dominant driver of how long people live.
For decades, the public health message around longevity has been consistent: eat well, exercise regularly, sleep enough, and avoid smoking. Those habits matter. But a growing body of research is quietly dismantling the assumption that lifestyle choices are the primary engine of a long life. The science now points somewhere far less controllable: your DNA.
Rewriting the Numbers
The traditional scientific consensus, reflected in family studies and cited by the National Institutes of Health via MedlinePlus, held that roughly 25 percent of the variation in human lifespan is attributable to genetic factors. That figure shaped decades of public health messaging, placing the majority of longevity in the hands of individual behavior and environment.
More recent research has revised that estimate significantly upward. A 2022 comprehensive analysis found that genetics accounts for approximately 20 to 40 percent of human lifespan variation across the population. The picture shifts even more dramatically at older ages: after age 60, genetics may account for 30 to 50 percent of variation in extreme longevity. For people who reach their nineties and beyond, classified in research literature as nonagenarians, centenarians, semi-supercentenarians (ages 105 to 109), and supercentenarians (age 110 and older), the genetic signal is particularly pronounced.
The Jackson Laboratory's Landmark Mouse Study
The most direct evidence yet arrived in October 2024, when scientists at The Jackson Laboratory (JAX) in Bar Harbor, Maine published findings in Nature that challenged one of the field's most durable assumptions: that eating less extends life.
For nearly a century, laboratory studies had consistently shown that caloric restriction prolongs animal lifespan. The JAX team designed a study to test this more rigorously, tracking the health of nearly 1,000 genetically distinct mice across a range of diets. The genetic diversity of the mouse population was deliberate, chosen to better mirror the variation found in humans.
When researchers analyzed the full dataset, diet was not the dominant variable. Genetic factors had a far greater impact on lifespan than any dietary intervention. The study identified what the team called "genetically-encoded resilience," specifically the ability to maintain body weight, body fat percentage, and immune cell health under stress or caloric restriction, as a critical factor in survival. Notably, mice that did not lose body fat late in life survived the longest, complicating the conventional wisdom about leanness and longevity.
Gary Churchill, the lead researcher at JAX, distilled the finding pointedly: "If you want to live a long time, there are things you can control within your lifetime such as diet, but really what you want is a very old grandmother."
Identifying the Genes That Shorten Life
Parallel work has moved beyond broad estimates to identify specific genetic culprits. A study by Junyoung Park and colleagues at Stanford Neuroscience Health Center, published in Nature Communications, examined the UK Biobank population and identified eight genes carrying burdens of pathogenic missense variants linked to shorter lifespans. Those genes are DNMT3A, SF3B1, CHL1, TET2, PTEN, SOX21, TP53, and SRSF2.
The pattern that emerges from these eight is telling: most are associated with oncogenic, or cancer-related, pathways. This suggests that cancer-predisposing genetic variants represent a key biological mechanism through which inherited genetic profiles shorten life. It also connects longevity research more directly to cancer biology, two fields that have historically developed on parallel but separate tracks.
Sleep, Genetics, and the Limits of Universal Advice
The genetics-longevity connection extends into areas of health that feel deeply behavioral. Research covered by News-Medical has explored how sleep duration and genetics interact to affect functional health, adding complexity to what might seem like straightforward public health guidance.
The amount of sleep a person needs, and the health consequences of getting too little or too much, appear to be modulated by individual genetic profiles. This means that blanket recommendations about optimal sleep hours may not apply uniformly across the population. How your body responds to sleep deprivation or excess is, in part, written into your genome.

Epigenetics: Where Genes and Lifestyle Meet
None of this renders lifestyle irrelevant. Research published through PubMed Central draws an important distinction between genetic determinism and genetic influence. Epigenetic modifications, changes in how genes are expressed rather than in the underlying DNA sequence itself, are sensitive to both genetic background and lifestyle choices including diet and stress management.
These modifications may serve as biomarkers for the quality of aging, or may actively influence how fast and how well a person ages. The relationship is bidirectional: your genetic background shapes your epigenetic landscape, but lifestyle choices can modulate how genes express themselves over time. This is the space where personal behavior retains meaningful leverage, even if the ceiling of that leverage is set by inherited biology.
The Long Arc of Life Expectancy
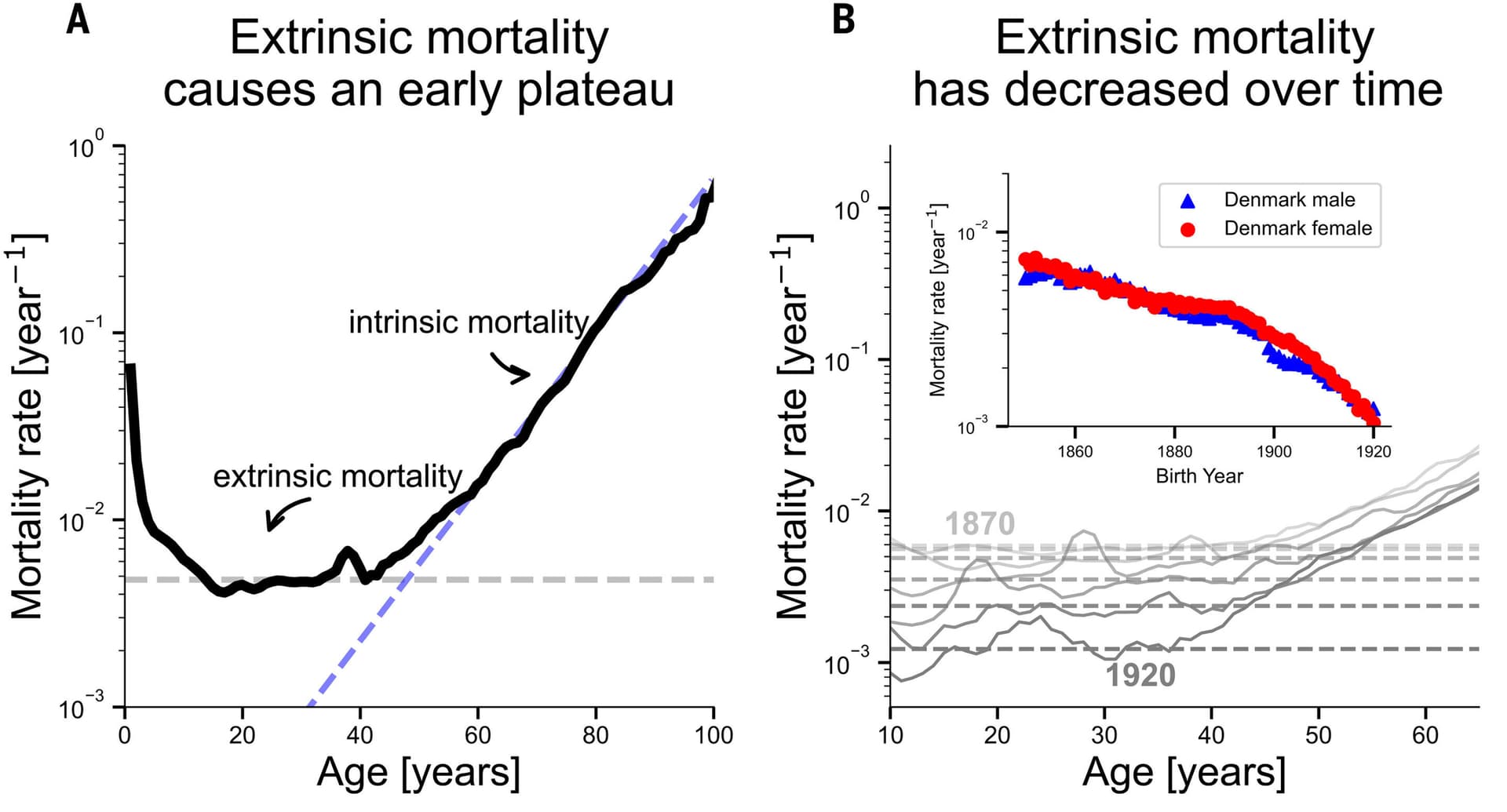
Understanding why genetics matters more at the extremes of lifespan requires some historical perspective. Environmental and public health improvements beginning in the early twentieth century dramatically extended average life expectancy through better access to food and clean water, improved housing conditions, reduced exposure to infectious disease, and advances in medical care. People in the United States now live approximately 80 years on average, a milestone driven largely by these population-level environmental gains.
Those gains are not going away. But researchers now argue that once the major environmental obstacles to survival are removed, genetic endowment plays an increasingly decisive role in determining who reaches 90, 100, or beyond. The low-hanging fruit of public health has largely been picked; what remains is more biological.
Who Reaches 100 and Why
Studies of the longest-lived individuals do reveal some shared lifestyle characteristics. Many centenarians and supercentenarians are nonsmokers, do not have obesity, cope effectively with stress, and women make up the majority of the group. These traits look behavioral on the surface.
Researchers caution, however, that these characteristics may themselves be partially heritable. Genetic variants that predispose someone to healthy weight regulation, stress resilience, or reduced cancer risk could manifest as the very "lifestyle" traits researchers observe. The causality is harder to untangle than it appears.
Longevity is also polygenic, meaning it is not controlled by a single gene or small set of genes but by hundreds of genetic variants, each with small individual effects, combining to influence lifespan. This explains why longevity runs visibly in families without following the predictable inheritance patterns of single-gene disorders.
A Field Still in Motion
Not all researchers are prepared to declare genetics the dominant force. Commentators at Fight Aging!, a research-focused site, highlighted data as recently as February 2025 continuing to suggest only a modest role for genetics in life expectancy, with some scientists emphasizing that the distinction between genetic variation within a species and between species is critical to interpreting animal study results.
A 17-year prospective cohort study posted to medRxiv in 2025 is actively examining how genetic predisposition to longer lifespan and lifestyle factors interact in their combined effect on all-cause mortality. Its results, when finalized, could recalibrate the debate once more.
What is clear is that the science of longevity is no longer a simple story about jogging and salads. The question of how long any individual lives is embedded, at least partly, in biological architecture built long before birth. The research emerging from labs in Bar Harbor and Stanford is not an invitation to abandon healthy habits; it is a corrective to the overconfidence that those habits alone hold the answer.
Sources:
Know something we missed? Have a correction or additional information?
Submit a Tip