HealthSplash founder convicted in $1 billion Medicare fraud scheme
A Kansas businessman was convicted in a scheme that sent bogus Medicare claims through telemedicine, extracting more than $450 million and targeting hundreds of thousands of seniors.

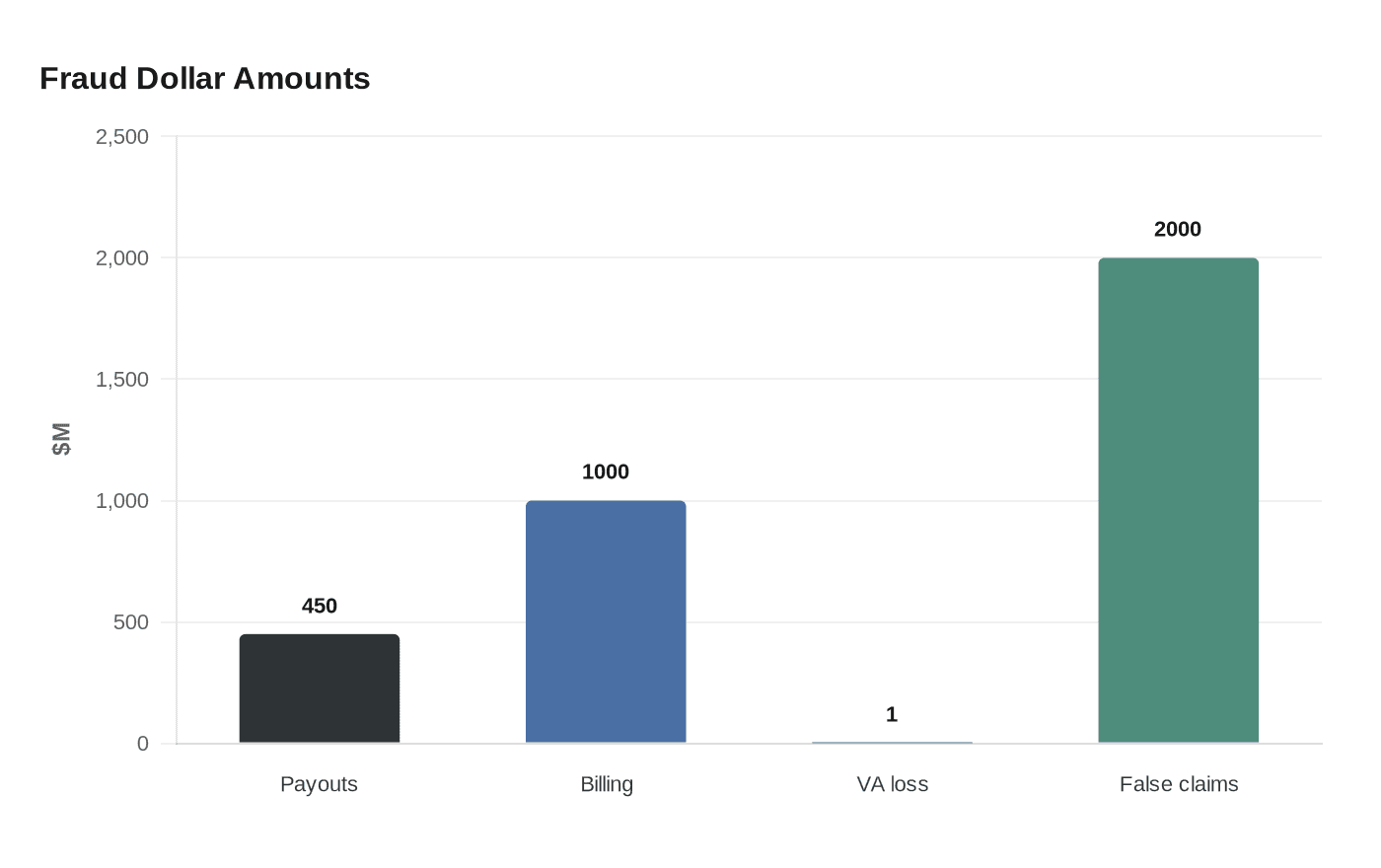
A federal jury convicted Brett Blackman in a scheme that prosecutors said turned Medicare’s payment system into a cash machine, with false claims generating more than $450 million in payouts and more than $1 billion in fraudulent billing overall.
Blackman, 42, of Johnson County, Kansas, was the founder, owner and CEO of HealthSplash. Prosecutors said HealthSplash acquired Power Mobility Doctor Rx, LLC, known as DMERx, in September 2017 and used the internet-based platform to generate false doctors’ orders and prescriptions that were billed to Medicare and other federal health care benefit programs.
The jury in the Southern District of Florida found Blackman guilty on May 13, 2026, of conspiracy to commit health care fraud and wire fraud, conspiracy to pay and receive health care kickbacks, and conspiracy to defraud the United States and make false statements in connection with health care matters. He faces up to 20 years in prison on the fraud and wire-fraud count, five years on the kickback count and five years on the false-statements count. Sentencing is set for August 26, 2026.
The case exposed a familiar weakness in federal health spending: distant marketing, fast approvals and layered contractors can make it easier to push unnecessary care onto beneficiaries before regulators catch up. Prosecutors said the operation targeted hundreds of thousands of Medicare beneficiaries through telemarketing, spam mailers, television ads and offshore call centers, steering them toward medically unnecessary orthotic braces, other durable medical equipment, prescription creams and similar items. Purported telemedicine doctors then signed bogus orders, often without meaningful interaction with patients and sometimes with no interaction at all.
The fraud did not stop at Medicare. The scheme also touched other federal programs, and investigators from HHS-OIG, the FBI, VA-OIG and the Defense Criminal Investigative Service helped build the case. The Veterans Affairs inspector general has said the loss to VA alone was more than $1 million.
Acting Attorney General Todd Blanche called it “one of the most egregious fraud schemes in Florida history” and said it targeted “hundreds of thousands of Medicare beneficiaries.” The broader case has already reached other defendants, including Gregory Schreck, who pleaded guilty in February 2025. Prosecutors said the overall indictment accused the participants of pushing nearly $2 billion in false claims, with the business operating from Overland Park, Kansas, before the state later forfeited it.
Know something we missed? Have a correction or additional information?
Submit a Tip

