Measles Cases Reach Six Year High as Vaccination Rates Fall
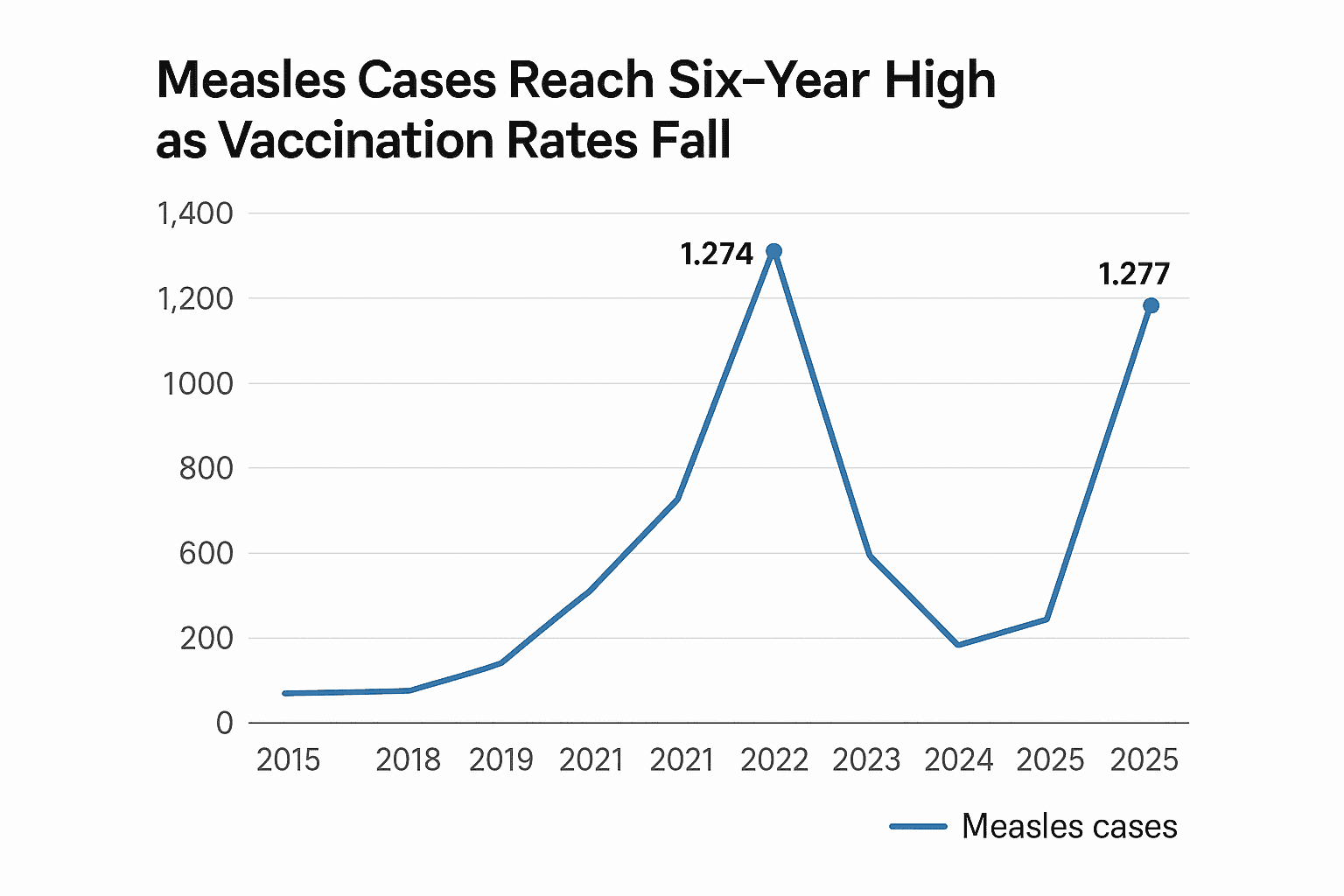
Johns Hopkins outbreak data show about 1,277 measles cases so far in 2025, the highest U.S. total in six years and slightly above the last major outbreak year. Public health officials warn the rise, concentrated in states with falling childhood vaccination, increases risks to vulnerable communities and challenges school and state immunization policies ahead of the winter respiratory season.
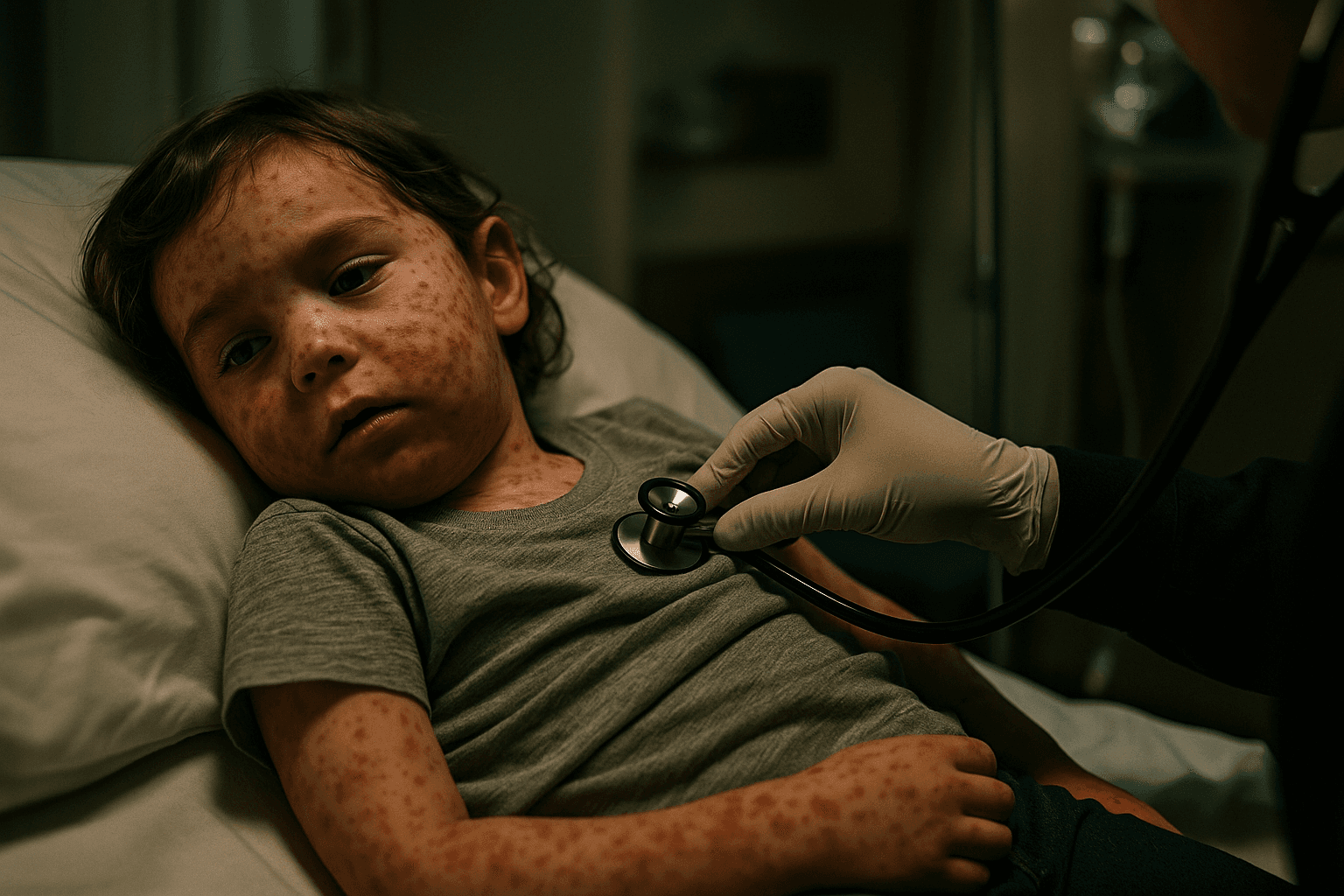
Johns Hopkins University’s outbreak response center reported on December 4 that the United States has recorded about 1,277 measles cases in 2025, marking the highest annual total since 2019 and edging slightly past that year’s tally. The aggregated data point reflects outbreaks centered in several states, with Texas identified as the epicenter where health authorities report several hundred cases, and infections spilling into multiple jurisdictions.
The rise follows a decline in childhood MMR vaccination coverage in parts of the country, public health officials say, leaving clusters of children and adults susceptible to a virus that is among the most contagious known to medicine. Measles can produce severe complications, including pneumonia and encephalitis, and the two dose MMR vaccine is about 97 percent effective at preventing disease when administered according to the standard schedule.
The timing of the surge raises concern because health departments are preparing for the peak of the winter respiratory season, when schools and crowded indoor settings can accelerate transmission. Local health agencies are already adapting responses to contain spread, issuing targeted vaccination drives, isolation orders where required, and temporary school exclusions in communities with low coverage. Those measures impose real costs on families and local economies, particularly on low income households that may lack paid leave or flexible work arrangements.
Beyond the immediate clinical threat, the numbers expose deeper systemic vulnerabilities in vaccine preventable disease control. Public health infrastructure has seen years of underinvestment in many states, and patchwork policies on school entry requirements and non medical exemptions have left uneven protections. Communities with limited access to pediatric care, transportation, or insurance face greater barriers to catching up missed immunizations. At the same time, misinformation and distrust of institutions continue to erode confidence in vaccines in some areas, compounding access problems.
Policy choices now will shape whether this year remains an outlier or a turning point. Strengthening state immunization programs, increasing funding for local health departments, and ensuring Medicaid and community clinics can offer convenient, no cost vaccination are immediate levers. School districts may confront renewed pressure to tighten entry requirements and reduce exemptions to secure herd immunity for students too young to be fully vaccinated.
Public health experts emphasize that expanding MMR coverage now could blunt the winter surge and prevent more widespread outbreaks. That requires coordinated federal guidance, resources for outreach in hard hit neighborhoods, and strategies that address both supply and demand in equitable ways. For families and caregivers the message from health officials and providers is clear, and pragmatic: verify immunization records, speak with a trusted clinician about catch up schedules, and get vaccinated to protect children and the wider community before respiratory season peaks.
Sources:
Know something we missed? Have a correction or additional information?
Submit a Tip

