New Gene Editing Technique Reactivates Fetal Hemoglobin Gene to Fight Disease
A CRISPR-based therapy eliminated sickle cell pain crises in 27 of 28 patients by reactivating a fetal hemoglobin gene silenced since birth.
Twenty-seven of 28 patients with severe sickle cell disease experienced zero painful vaso-occlusive events after receiving a single infusion of an experimental gene-editing therapy, according to results published in the New England Journal of Medicine in April 2026.
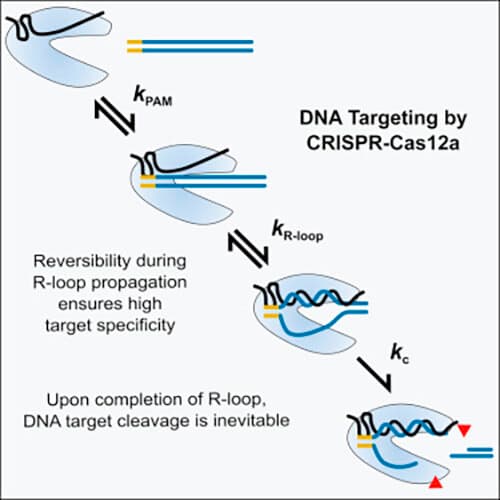
The therapy, renizgamglogene autogedtemcel (reni-cel), works by editing patients' own blood-forming stem cells to reactivate a hemoglobin gene the body naturally silences after birth. Using CRISPR-Cas12a technology, a more precise variant of the gene-editing tools currently in clinical use, researchers targeted the promoters of the HBG1 and HBG2 genes, disrupting binding sites for BCL11A, a protein that suppresses fetal hemoglobin production in adults. The result mimics a rare naturally occurring genetic condition, hereditary persistence of fetal hemoglobin, in which individuals carry lifelong elevated levels of the fetal protein and are largely protected from sickle cell complications.
The phase 1-2 multicenter study, known as the RUBY trial, enrolled 28 patients between the ages of 12 and 50 who had experienced at least two severe vaso-occlusive events per year. Four of those patients were treated at Cleveland Clinic Children's, whose division chair, Rabi Hanna, MD, led the research.
By six months after treatment, average total hemoglobin levels rose from 9.8 g/dL to 13.8 g/dL, approaching the range seen in people without the disease. Average fetal hemoglobin reached 48.1% and remained stable over time. Most patients saw key blood cells recover within a single month of receiving the infusion.
"This is remarkable for these patients, most of whom had numerous severe VOEs requiring an average of nearly five hospital admissions each year," said Hanna, chair of the Pediatric Hematology, Oncology and Blood and Marrow Transplant Division at Cleveland Clinic Children's. "In addition, these patients have reported improvements in their physical and social functioning."

Sickle cell disease distorts red blood cells into a rigid crescent shape that blocks blood vessels and ruptures prematurely, causing intense recurring pain, organ damage, and a life expectancy typically cut short in the mid-40s. Medications can manage symptoms, but a cure has historically required a bone marrow transplant, a procedure available to fewer than 20% of eligible patients due to the scarcity of matched sibling donors.
Two FDA-approved gene therapies for sickle cell disease already exist: exagamglogene autotemcel (Casgevy), developed by Vertex Pharmaceuticals and CRISPR Therapeutics, and lovotibeglogene autotemcel (Lyfgenia), made by bluebird bio. Reni-cel, sponsored by Editas Medicine, uses the Cas12a variant rather than the Cas9 enzyme employed in Casgevy, a distinction its developers argue produces more consistent and predictable editing results.
The procedure harvests a patient's own CD34+ hematopoietic stem cells, edits them outside the body, and reinfuses them, eliminating the immune rejection risk associated with donor transplants. Updated data presented at the American Society of Hematology annual meeting in late 2025 showed 38 of 40 treated patients were pain-free at a median follow-up of approximately 13.5 months. The RUBY trial remains active as researchers continue monitoring whether those hemoglobin gains hold over years, not just months.
Know something we missed? Have a correction or additional information?
Submit a Tip
