New research finds hidden awareness in many unresponsive brain-injury patients
One in four apparently unresponsive brain-injury patients showed hidden awareness on brain tests, forcing a new look at pain control, rehab and family consent.
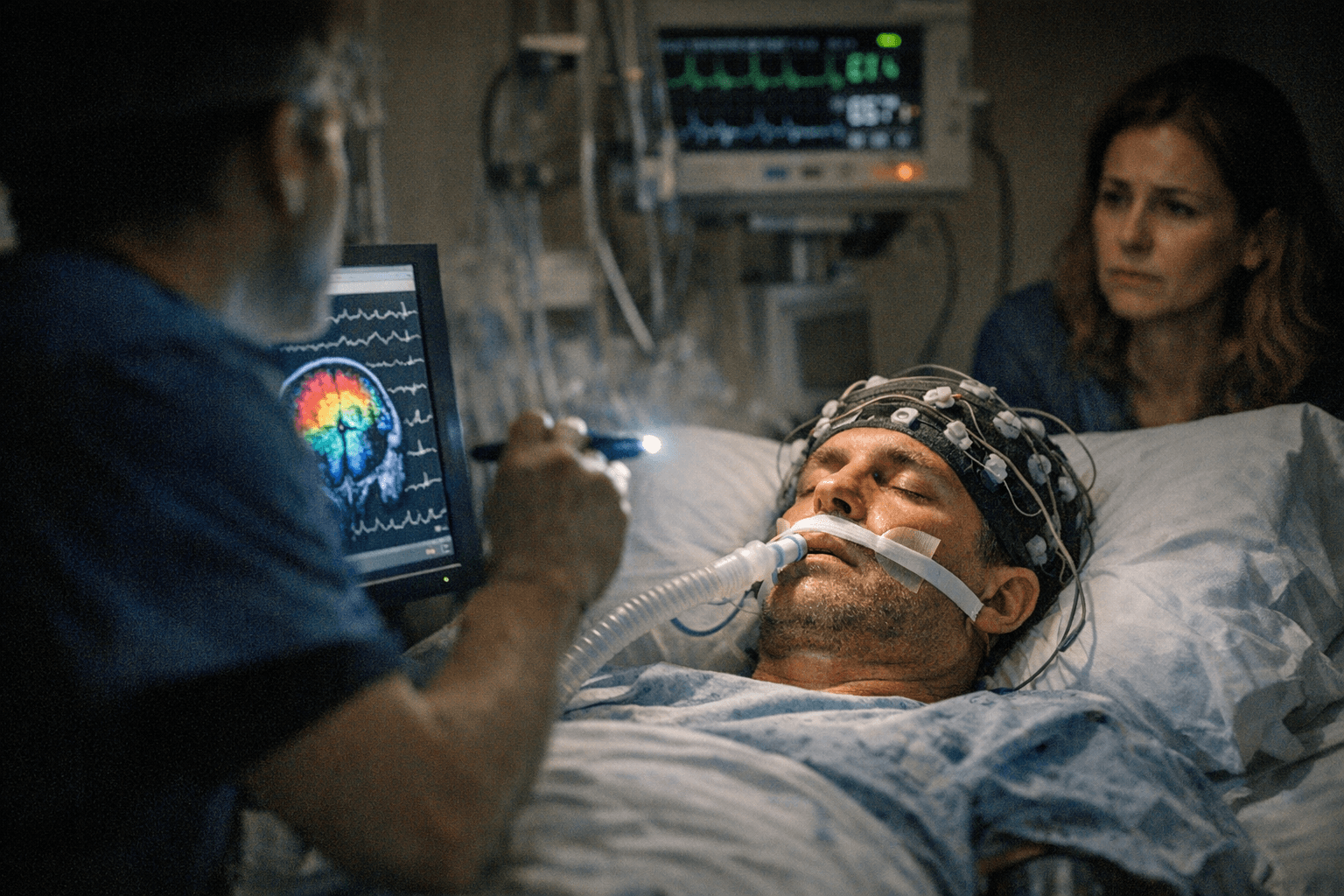
Hidden awareness may be far more common than bedside exams have long suggested. In a 2024 international study highlighted by Harvard Medical School and Weill Cornell Medicine, about one in four patients with severe brain injury who appeared unresponsive showed covert responses on EEG or brain scans, indicating they could follow instructions internally even when they could not move or speak.
That finding carries immediate medical and ethical consequences. Covert consciousness is residual awareness that evades routine bedside behavioral detection, and a 2024 commentary in The Lancet Neurology said recognizing it could help identify patients who are more likely to emerge from coma. If a patient can understand a voice, register pain or process a command without any outward response, then decisions about sedation, pain management, rehabilitation and even whether to continue aggressive treatment become far more complicated.
The stakes are not abstract. A Lancet review cited a classic series in which 17 of 40 patients referred with a diagnosis of persistent vegetative state were later found to be aware. Older diagnostic guidance had already warned that the diagnosis is not always simple and urged consultation by several experts. Some neurologists and ethicists have argued that the term persistent vegetative state is misleading because the condition is often not truly permanent, and that language itself can shape how families and clinicians think about prognosis.
Researchers at institutions including Columbia University Irving Medical Center, NewYork-Presbyterian and Western University have helped push the field toward better assessment standards and emerging diagnostic tools. Adrian Owen, Jan Claassen, Jennifer Welsh and Keith Andrews are among the names long associated with work showing that patients can sometimes demonstrate cognition without movement. Weill Cornell Medicine has described cases in which patients with severe brain injury showed clear signs of cognitive function on brain scans when asked to carry out complex mental tasks.
The ethical question now extends beyond diagnosis to disclosure. Ethics literature has argued that scientifically valid results showing covert awareness should be shared with family members, because the information may alter communication plans, rehabilitation goals and end-of-life decisions. For families already facing uncertainty, knowing that a loved one may still be aware can change how they interpret silence in the room.
The public health significance is broad. Hospitals that rely too heavily on brief bedside observations risk missing a vulnerable group of patients whose suffering, cognition and prospects for recovery are all being underestimated. As the evidence grows, the standard for severe brain injury care may need to move from assuming absence of awareness to proving it is truly absent.
Sources:
Know something we missed? Have a correction or additional information?
Submit a Tip

