UnitedHealth and CVS standardize prior authorization to cut delays
UnitedHealth and CVS Health said more than half of prior authorizations now use standardized rules, but patients still face the same gatekeeper: insurer approval.

Standardizing prior authorization may cut paperwork, but the harder question is whether it will speed care or simply make denials more efficient. UnitedHealth and CVS Health said on April 24 that they had aligned data and submission requirements for more than half of their prior authorization requests, a move aimed at smoothing one of the most frustrating delays in American health care.
UnitedHealthcare, UnitedHealth’s insurance arm, said more than 70% of prior authorization requests are expected to fall under the standardized process by the end of the year. That scale matters because prior authorization often determines whether a patient gets therapy, imaging, surgery, or even certain medicines on time, after a doctor has already decided treatment is needed.
The push fits into a broader federal and industry effort to reduce the administrative burden without abandoning utilization review. The Centers for Medicare & Medicaid Services finalized its interoperability and prior authorization rule on January 17, 2024, covering Medicare Advantage, Medicaid managed care, CHIP managed care, and Affordable Care Act marketplace plans on the federal exchanges. CMS said the rule would reduce patient, provider and payer burden and estimated about $15 billion in savings over 10 years. Some operational provisions generally begin on January 1, 2026, with API development and enhancement compliance dates generally set for January 1, 2027.
The April 24 announcement also followed a June 23, 2025 pledge, when more than 50 health plans agreed with the U.S. Department of Health and Human Services and CMS to streamline prior authorization. HHS said those plans cover nearly eight out of 10 Americans. AHIP later said the commitments included eliminating 11% of prior authorizations, equal to 6.5 million fewer requests, and moving toward handling 80% of electronic prior authorization requests in real time.

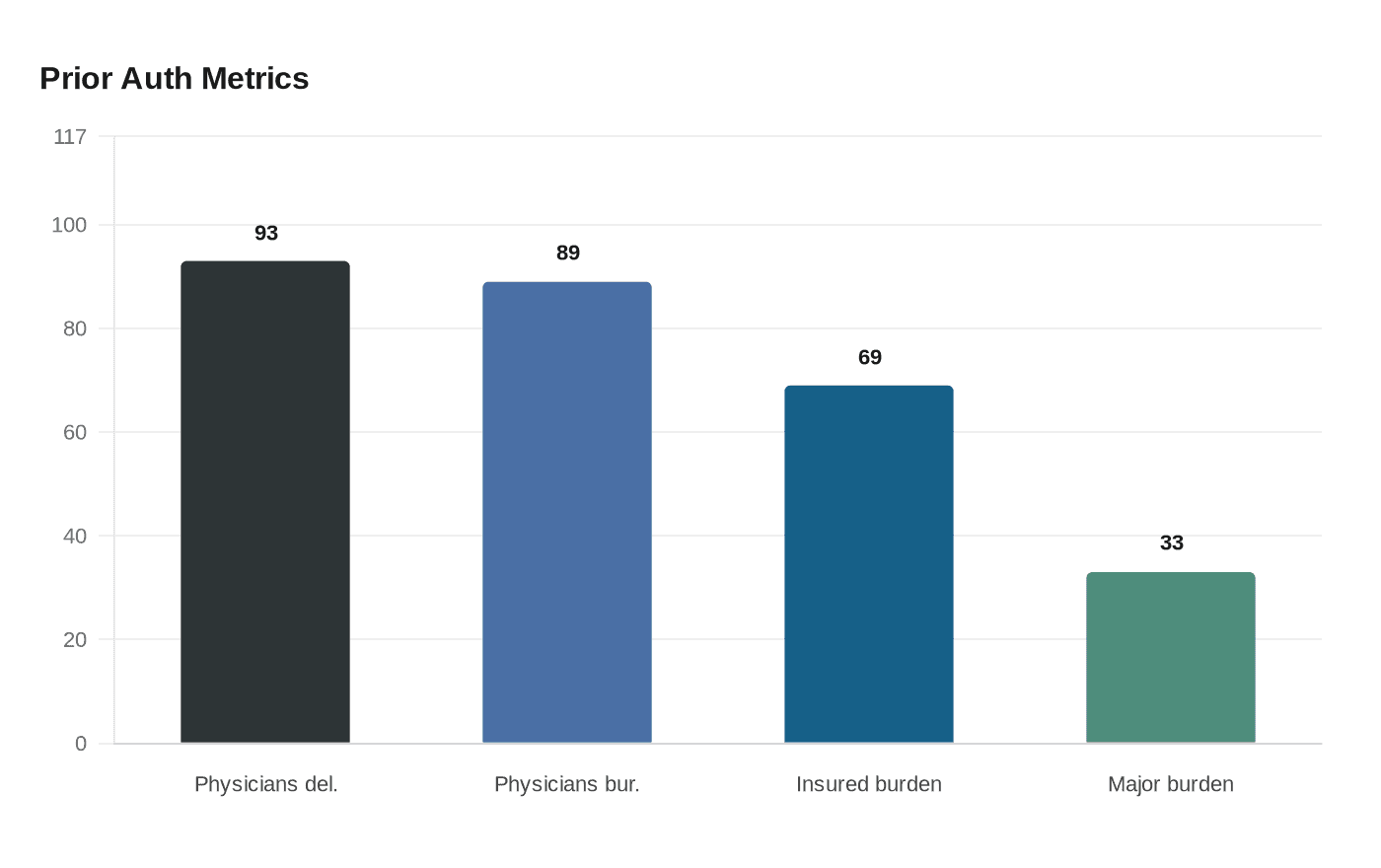
Pressure on insurers has only grown as physicians and patients describe the process as a barrier to care. The American Medical Association’s 2024 survey found 93% of physicians said prior authorization delays patient care and 89% said it contributes to burnout. KFF reported in 2025 that about 69% of insured adults said prior authorization is a burden when accessing care, including one in three who called it a major burden.
That is why the new standardization steps will be judged less by the language of simplification than by measurable results: fewer forms, faster approvals, fewer appeals. Insurers, including UnitedHealth and CVS Health, are trying to show that standardization can reduce friction for doctors and patients. Providers, who still have to live inside the system every day, will be watching to see whether the process becomes easier to use or merely more uniform in refusing care.
Know something we missed? Have a correction or additional information?
Submit a Tip

