UnitedHealthcare to end prior approval for some surgeries, tests, therapies
UnitedHealthcare will drop approval rules for some surgeries and tests, but only after regulators and doctors have spent years pressing on delays.

UnitedHealthcare said it will eliminate prior approval for some outpatient surgeries, diagnostic tests, therapies and chiropractic care, a move that trims one of the most criticized gatekeeping steps in U.S. health care. By the end of 2026, the insurer said it will remove an additional 30% of its remaining prior authorizations, including select outpatient surgeries, some diagnostic tests such as echocardiograms, certain outpatient therapies and chiropractic care.
The change still leaves a large share of utilization review in place. UnitedHealthcare said prior authorization is required for only 2% of its medical services, and that about 92% of submitted requests are approved in less than 24 hours on average. The insurer said it will post the full list of affected services on its provider site before the new policy takes effect.

The announcement lands in the middle of a broader industry retreat from rigid prior approval systems. In June 2025, AHIP said health plans had made voluntary commitments to streamline, simplify and reduce prior authorization across commercial coverage, Medicare Advantage and Medicaid managed care, a set of changes the group said would affect 257 million Americans. AHIP also said the plans were working toward a standardized electronic prior authorization framework by January 1, 2027. Separate federal rules finalized by the Centers for Medicare & Medicaid Services in 2024 also aimed to reduce administrative burden, with some requirements taking effect January 1, 2026.
Physician groups have argued that prior authorization delays care and raises costs. The American Medical Association said in a recent survey that nearly 90% of physicians reported the process leads to higher overall health care utilization, and more than one-quarter said it had led to a serious adverse event for a patient in their care. The same survey found that 79% of doctors said a delay or denial at least sometimes forces patients to pay out of pocket.

UnitedHealthcare cast the step as part of a wider effort to reduce paperwork, saying it has expanded its Gold Card program, invested in digital tools for electronic submission and real-time status tracking, and helped standardize electronic prior authorization requirements. The insurer said more than 70% of its prior authorizations will be part of the new standardized submission process by year-end, and it said it has fewer prior authorization requirements in Medicare Advantage than any other insurer.
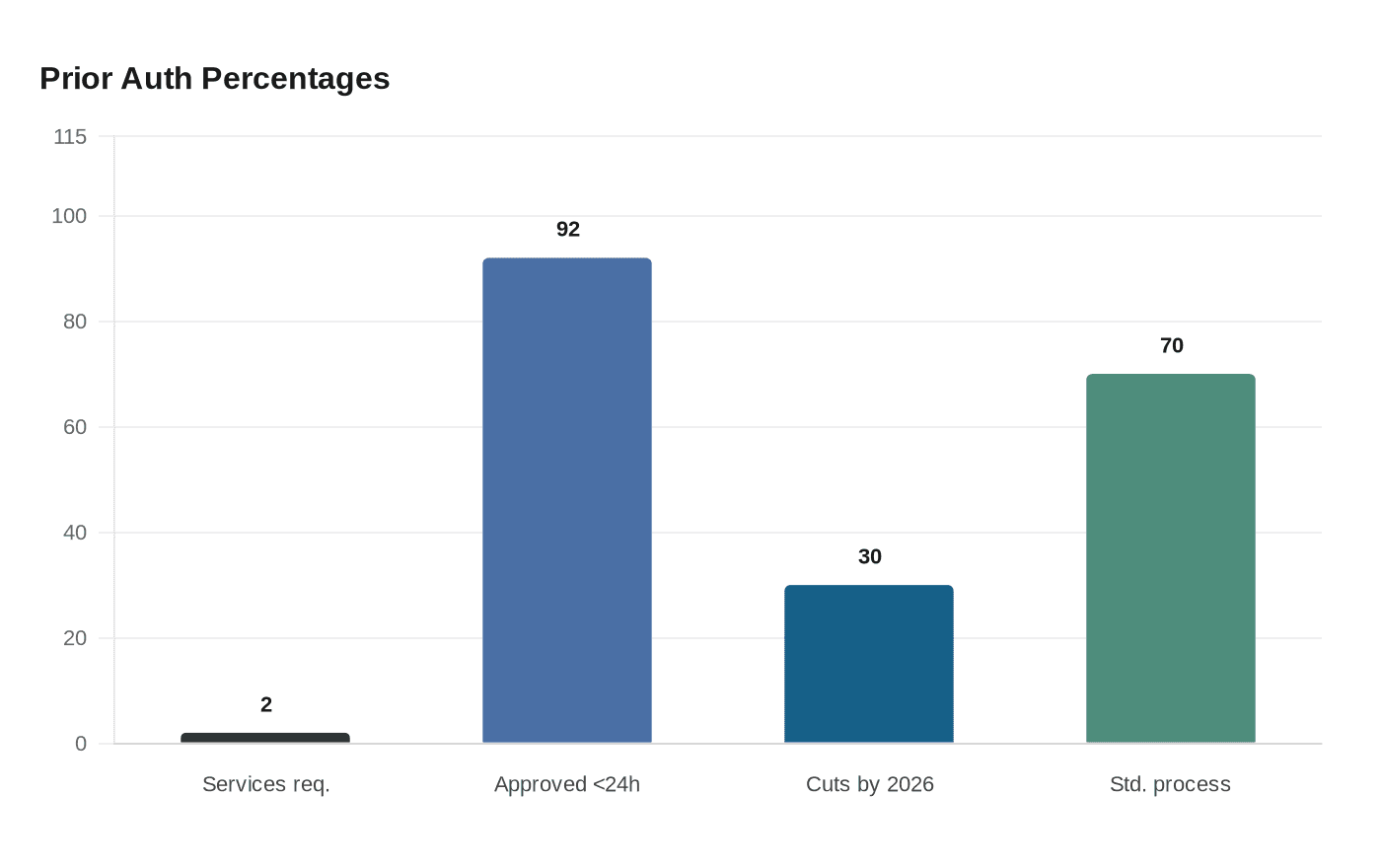
For patients and doctors, the question is not whether the system has become painful enough to force change. It is whether this is the start of a genuine rollback or a limited concession that preserves the insurer’s core control over access to care.
Know something we missed? Have a correction or additional information?
Submit a Tip

