Upstate measles surge grows to 646 cases as dozens face quarantine
South Carolina health officials reported 88 new measles cases, raising the Upstate cluster to 646 and prompting hundreds of quarantines across schools and campuses.

South Carolina health officials reported 88 new confirmed measles cases on Jan. 20, bringing the Upstate outbreak total to 646 and intensifying pressure on public health and local institutions to contain spread. The two state updates over the past week together add 212 cases, a sharp acceleration that has propelled the cluster into one of the largest U.S. outbreaks in recent memory.
The outbreak is centered in Spartanburg County, a northwestern community of roughly 39,000 residents, where the Department of Public Health (DPH) has linked multiple public exposures to schools, grocery stores and college campuses. DPH identified exposures at Starr Elementary, Global Academy and Boiling Springs High School among other sites. At least 15 schools now have students in quarantine, and DPH has reported 538 people currently under quarantine and 33 in isolation.
Higher education settings have been drawn into the disruption. Clemson University and Anderson University each have reported one confirmed measles case and have quarantined 34 and 50 students respectively, reflecting the outbreak’s capacity to strain campus health operations and residential life.
Public exposures at two grocery stores have widened the circle of concern. DPH flagged an infectious visit to a Publix in Duncan on Jan. 16, with exposed people advised to monitor for symptoms through Feb. 6. Infectious visits to a Food Lion in Inman on Jan. 11 and Jan. 12 prompted monitoring windows running through Feb. 1 or Feb. 2. These retail exposures complicate containment because they involve transient contacts and diffuse notification challenges for public health officials.
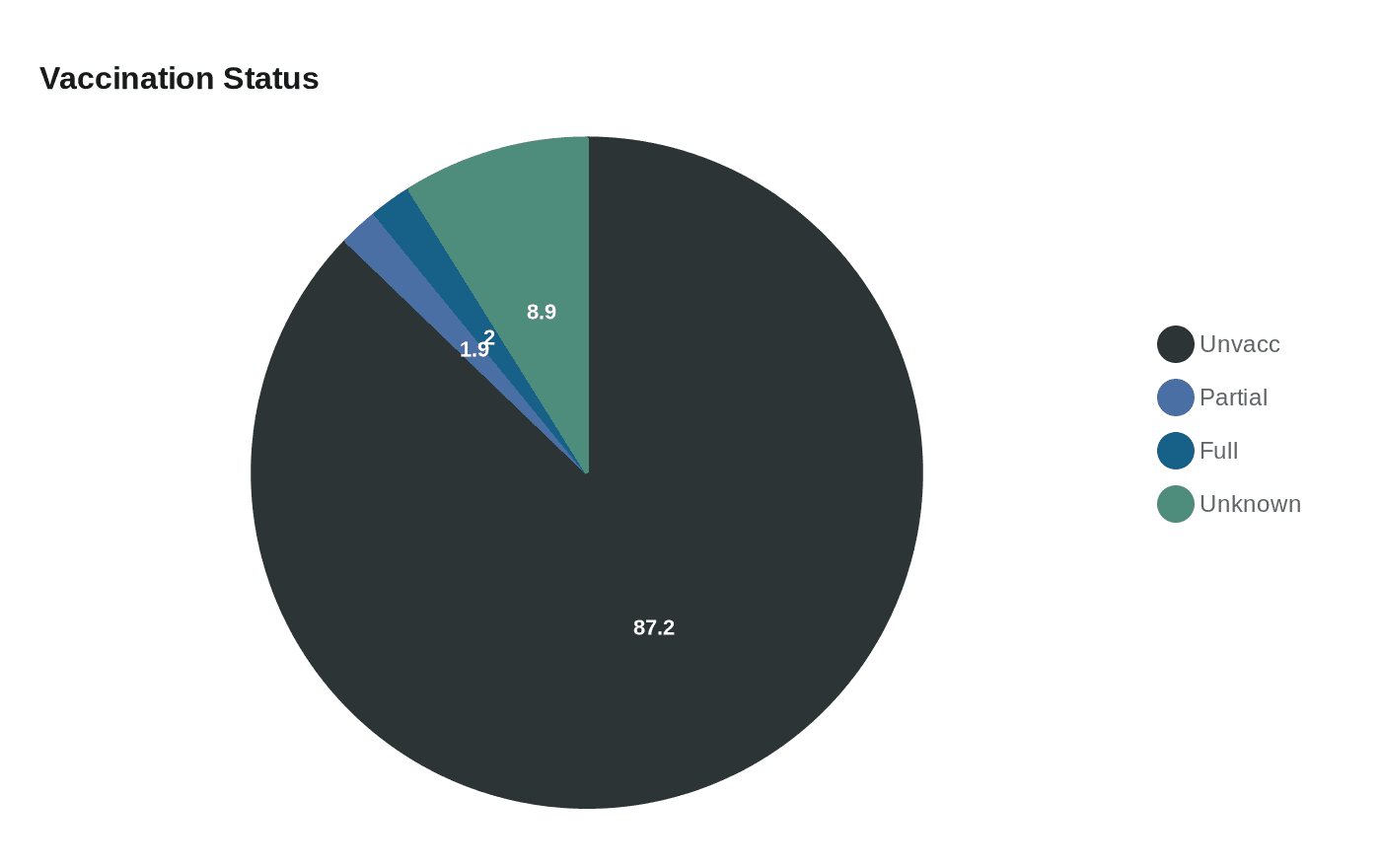
DPH’s case data underscore the outbreak’s link to insufficient immunity. Among the 646 reported case-patients, 563 were unvaccinated, 12 were partially vaccinated, 13 were fully vaccinated and 58 had unknown vaccination status. Children account for a large share of infections: 155 patients are under 5 years old and 419 are aged 5 to 17. National guidance reiterates that two doses of the measles-mumps-rubella vaccine provide the strongest protection, with one dose about 93 percent effective and two doses about 97 percent effective.
Beyond immediate containment, the outbreak raises policy and institutional questions. The size and speed of case increases expose gaps in vaccination coverage and in the public-health infrastructure that supports outbreak response, including contact tracing capacity and quarantine enforcement. Local health departments and school systems face decisions about mandatory exclusion policies, resource allocation for vaccine clinics, and communication strategies to rebuild community trust.
The cluster also has broader implications for national measles control. More than 2,000 U.S. infections reported over the past 12 months and several recent deadly clusters have renewed debate over whether the nation can sustain its measles elimination status without stronger vaccination programs and tighter control of exemption pathways.
DPH has emphasized vaccine access through primary care providers, pharmacies and county health departments and is urging eligible people to receive MMR vaccination. As quarantines stretch across classrooms and dormitories, elected officials and public institutions will confront choices that could reshape local public-health policy and civic engagement in coming weeks. The outbreak’s trajectory will hinge on accelerating vaccination, rapid identification of contacts and sustained institutional coordination to prevent further spread.
Know something we missed? Have a correction or additional information?
Submit a Tip

