US proposes new fertility insurance rule, expanding employer benefits
Workers could buy fertility coverage without joining a company health plan, but only if employers opt in and the benefit stays capped at $120,000.

Workers whose employers never offered fertility care outside major medical coverage could soon get a standalone benefit, but only if their companies choose to provide it. The Labor, Health and Human Services, and Treasury departments proposed a rule on May 10 that would create a new category of limited excepted benefits for fertility care, letting employers offer coverage more like dental and vision, without requiring enrollment in the company’s main health plan.
The proposal would give employers broad choice, not a mandate. It would set a combined lifetime maximum of up to $120,000 for the participant and their beneficiaries, with the cap indexed for inflation for plan years starting after 2028. Employers would have to give workers a notice clearly describing the coverage, and the public will have 60 days after Federal Register publication to comment. The administration said the goal is to ease statutory and regulatory burdens that have kept fertility benefits fragmented and hard to offer.

That design could matter most for small and medium-size employers, which the White House singled out as gaining new options. But the coverage gap would remain substantial: workers whose employers do not adopt the benefit would still be left out, and the proposal does not automatically extend fertility care to people covered by public programs that generally do not pay for IVF.
The move builds on President Donald Trump’s Feb. 18, 2025 executive order on expanding access to in vitro fertilization. Federal agencies had already issued FAQs on Oct. 16, 2025, pointing employers to existing pathways, including fully insured specified-disease policies for infertility, excepted-benefit HRAs, and EAP-style coaching and navigation services. Those same agencies said they planned additional rulemaking, and this proposal is the result.
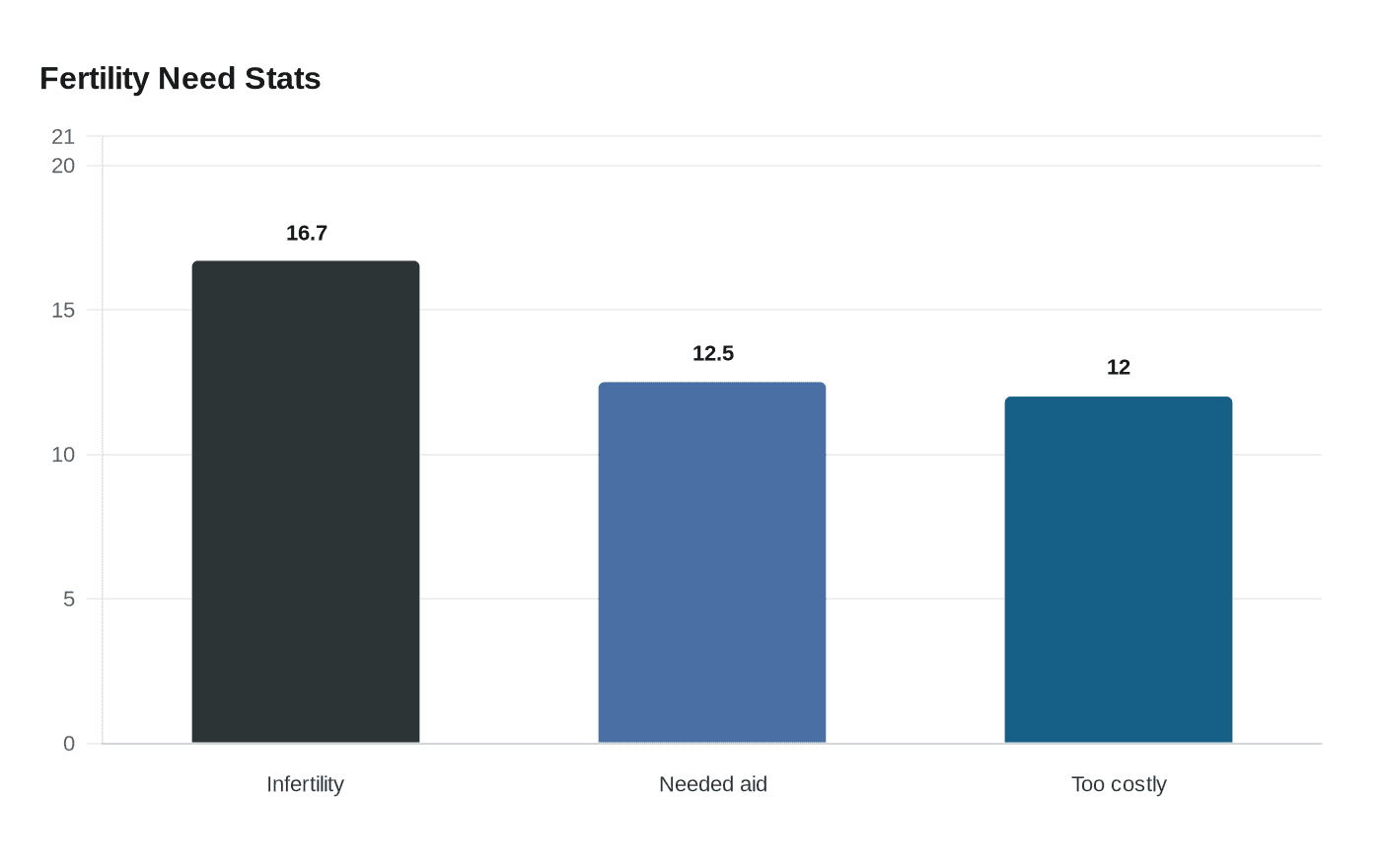
The policy arrives amid stark need. The American Society for Reproductive Medicine says about one in six adults experiences infertility during their lifetime, and KFF says one in eight women ages 18 to 49 report that they or their partner needed fertility assistance services. Cost remains the biggest barrier, with KFF finding that 12% of those who needed services did not get them because they were too expensive.
The administration has paired the rule with broader cost-cutting promises, including a White House fertility initiative that said drug discounts could save women up to $2,200 per cycle on medications that often cost more than $5,000. It also said EMD Serono will manufacture IVF drugs in the United States for the first time under the deal. Even so, the practical impact of the new insurance rule will depend on how many employers choose to offer it, and how many workers can use it.
Know something we missed? Have a correction or additional information?
Submit a Tip