Former KPMG Manager Wins Long-Term Disability Appeal Against Prudential
A former KPMG advisory manager reversed Prudential's long-term disability denial in 40 days, exposing how mental-health claims get challenged and overturned.

A former KPMG advisory manager won a long-term disability appeal against Prudential in roughly 40 days, reversing a benefits denial despite having an approved short-term disability claim already on file. The case, detailed in a specialty disability-law analysis, turns on a pattern disability attorneys encounter repeatedly: a paper review by a psychiatrist who never examined the claimant, pitted against treating providers who did.
The claimant had been under care for severe anxiety and depression, treated by both a licensed clinical social worker and a primary care physician. When the short-term disability claim transitioned to long-term coverage, Prudential cut off benefits, citing insufficient evidence. No in-person examination was conducted on Prudential's behalf. The insurer instead relied on a file review by a non-examining psychiatrist, a practice that is both legal and common for mental-health claims, where objective clinical testing is inherently limited by the nature of the conditions involved.
The appeal succeeded by attacking that asymmetry directly. Counsel reframed and strengthened the existing treating-provider evidence, then pressed a question Prudential could not adequately answer: if the claimant was disabled enough to qualify for short-term benefits one day, what clinically changed when long-term coverage was supposed to begin? Without an answer, the carrier reversed its decision.

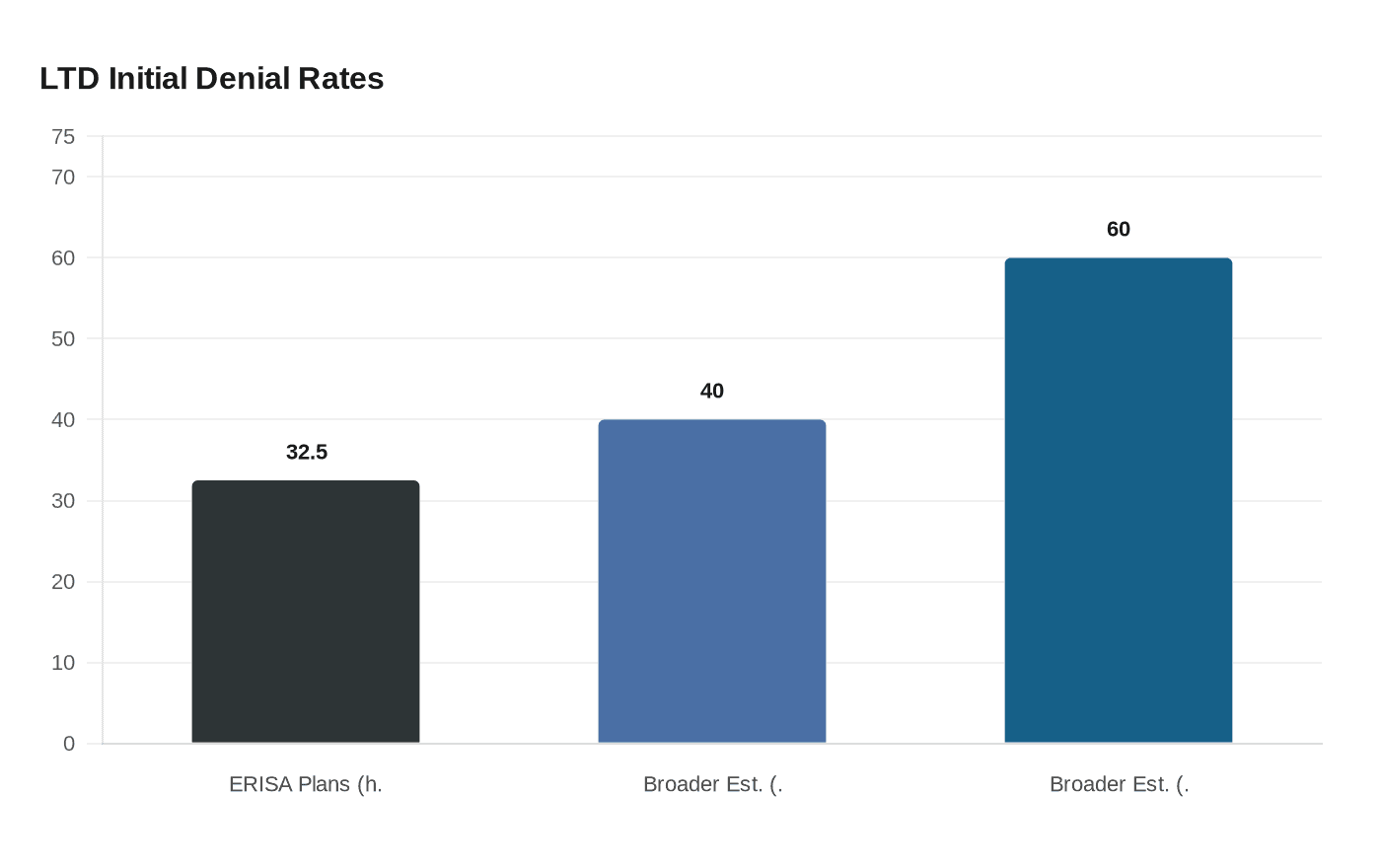
Mental-health LTD claims face disproportionate scrutiny at that transition point. Initial denial rates for private-ERISA disability plans run as high as 32.5 percent, with some broader estimates ranging from 40 to 60 percent, according to a 2025 analysis by disability-benefits attorneys at Bross & Frankel. Mental-health conditions are challenged most aggressively, typically on "lack of objective evidence" grounds that would never be applied to a fracture or a cancer diagnosis.
For KPMG employees navigating that STD-to-LTD window, documentation is the decisive variable. Every appointment with a treating physician or therapist should generate a clinical note that goes beyond a diagnosis code to capture functional limitations: what the claimant cannot do, not merely what condition they carry. Gaps in treatment, even understandable ones, become ammunition for denial. Treating providers need to understand their role in the claim record; a letter from a licensed clinical social worker carries weight in an appeal only when it addresses specific work-function limitations rather than simply confirming ongoing treatment. Involving a psychiatrist early, before a denial arrives, adds clinical credibility that paper reviewers find harder to dismiss. A timeline documenting the full arc of treatment, from initial short-term approval through every subsequent clinical contact, is the scaffolding an appeal is built on.
For HR leaders and benefits administrators, the KPMG case is a process signal. The STD-to-LTD transition is the single highest-risk moment in any disability claim, and most employees do not know that. Proactive outreach to employees approaching that transition, clear internal guidance on assembling a longitudinal medical record, and access to benefits counsel before a denial letter is issued can each shift outcomes materially. Vendor-management protocols should include escalation paths specifically for contested mental-health claims.
The 40-day reversal in this case represents a best-case scenario. Most employees without legal representation never appeal at all, which is exactly the outcome insurers relying on non-examining file reviews are counting on.
Know something we missed? Have a correction or additional information?
Submit a Tip

