Cold Weather Linked to 40,000 Extra Cardiovascular Deaths Per Year, ACC Study Finds
Cold kills far more hearts than heat: a 20-year study of 14M+ U.S. deaths pins cold at 40K extra cardiac deaths yearly, vs. just 2,000 for heat.

The number that stops cold-plunge enthusiasts mid-breath: cold weather accounted for about 40,000 excess cardiovascular deaths each year during a 20-year study period, about 6.3% of all cardiovascular deaths, amounting to a total of 800,000 deaths over two decades. That finding, presented at the American College of Cardiology's Annual Scientific Session in New Orleans, is now the most comprehensive accounting of temperature-related cardiac mortality ever assembled for the United States, and it lands with particular weight for anyone whose wellness routine involves deliberately dropping their body temperature.
The study, titled "County-Level Temperature-Attributable Cardiovascular Disease Mortality in the U.S.," was led by Dr. Pedro Rafael Vieira De Oliveira Salerno, an internal medicine resident in the Icahn School of Medicine of Mount Sinai program at NYC Health + Hospitals/Elmhurst. Mount Sinai collaborated with NYU Health, Houston Methodist and Case Western Reserve University for the analysis. Researchers analyzed more than 14 million cardiovascular deaths of people over 25 years old across 819 counties in the United States, covering 80 percent of the country's population, between 2000 and 2020.
During that period, researchers found that the temperature associated with the lowest rate of cardiovascular death was 23° C, about 74° F, and rates gradually increased as temperatures deviated both below and above that level. Cardiovascular death rates followed a lopsided U-shaped curve: both extreme cold and extreme heat were associated with increased mortality, but the rise was steeper and larger on the colder side of the spectrum. For context on just how lopsided: hot weather accounted for about 2,000 excess deaths each year, about 0.33% of all cardiovascular deaths, or 40,000 deaths over two decades. Cold outpaced heat by a factor of 20 to 1.

The specific causes driving those cold-month deaths are the same ones that come up repeatedly in cardiovascular risk discussions: colder months are linked to significantly higher death rates from heart attacks, strokes, and coronary artery disease compared to milder periods. The physiological mechanism is not mysterious. Exposure to cold weather triggers a cascade of physiological changes including inflammatory processes and the constriction of blood vessels, which can ultimately lead to a greater risk of adverse cardiovascular events.
"This is the first time we have actual numbers for most of the United States, and we found the burden of excess deaths associated with cold is quite substantial," said Salerno. "As rates of chronic conditions like diabetes, heart failure and chronic kidney disease rise in the United States, we can expect to see a rise in the number of people who are more vulnerable to the effects of extreme temperatures," he added.
For the ice bath and cold-plunge community, none of this means the practice is inherently reckless. The study is measuring ambient environmental cold, not the controlled, short-duration immersion sessions most plungers log. But it does supply hard population-level numbers behind what cardiologists have been flagging anecdotally for years. "As clinicians, we see seasonal patterns in cardiovascular events, but this helps quantify how much cold exposure contributes at the population level. This isn't just about extreme weather. Even routine cold exposure, especially in vulnerable patients, can increase cardiovascular risk."
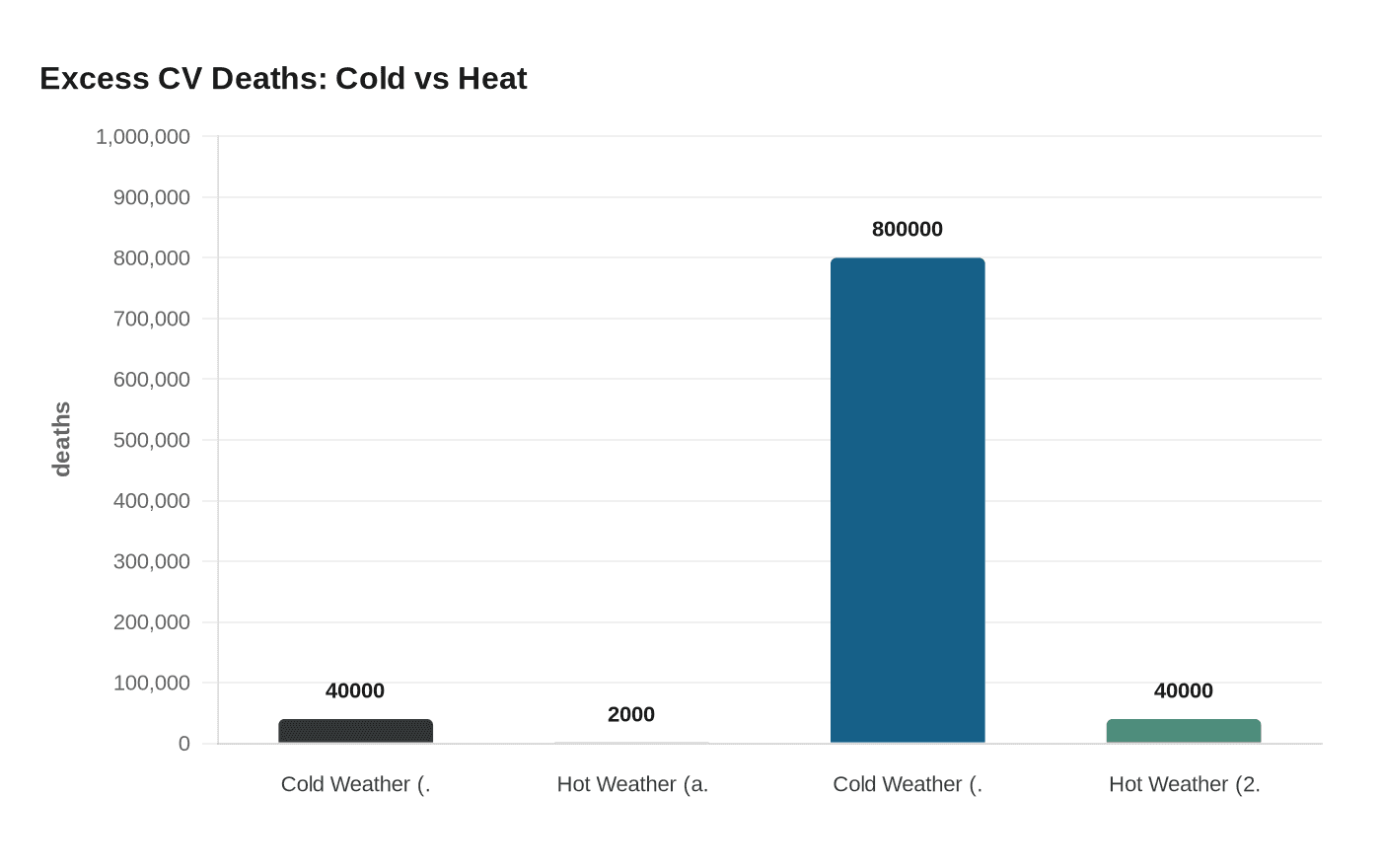
Colder temperatures are responsible for significantly more cardiovascular deaths from heart attacks, strokes, and coronary artery disease than milder months in the United States, and heat consistently gets more attention as a cause for concern, yet this study shows colder weather is the larger and more consistent risk. That asymmetry in public health attention is exactly what Salerno's team is pushing back against, arguing that cold deserves far more weight in how communities and clinicians plan for climate-related health burdens.
Salerno will present the study formally on Monday, March 30, at 9:30 a.m. at the Engage Stage for the Young Investigators Award Competition at ACC.26 in New Orleans.
Know something we missed? Have a correction or additional information?
Submit a Tip

