ER doctor says mindfulness cannot fix nurse burnout crisis
An ER doctor’s warning spread fast: yoga, breathing breaks and free coffee may soothe nurses, but they do not fix empty shifts. Canada’s staffing data shows why the critique hit a nerve.

Yoga classes, breathing exercises and free coffee can make a brutal shift feel a little less impossible, but Dr. Megan Miller argues they cannot repair a nurse burnout crisis built on underfunding and empty staffing slots. The Canadian emergency physician’s critique spread widely because it landed on a system already carrying too many overtime hours, too many overcapacity units and too many exhausted nurses.
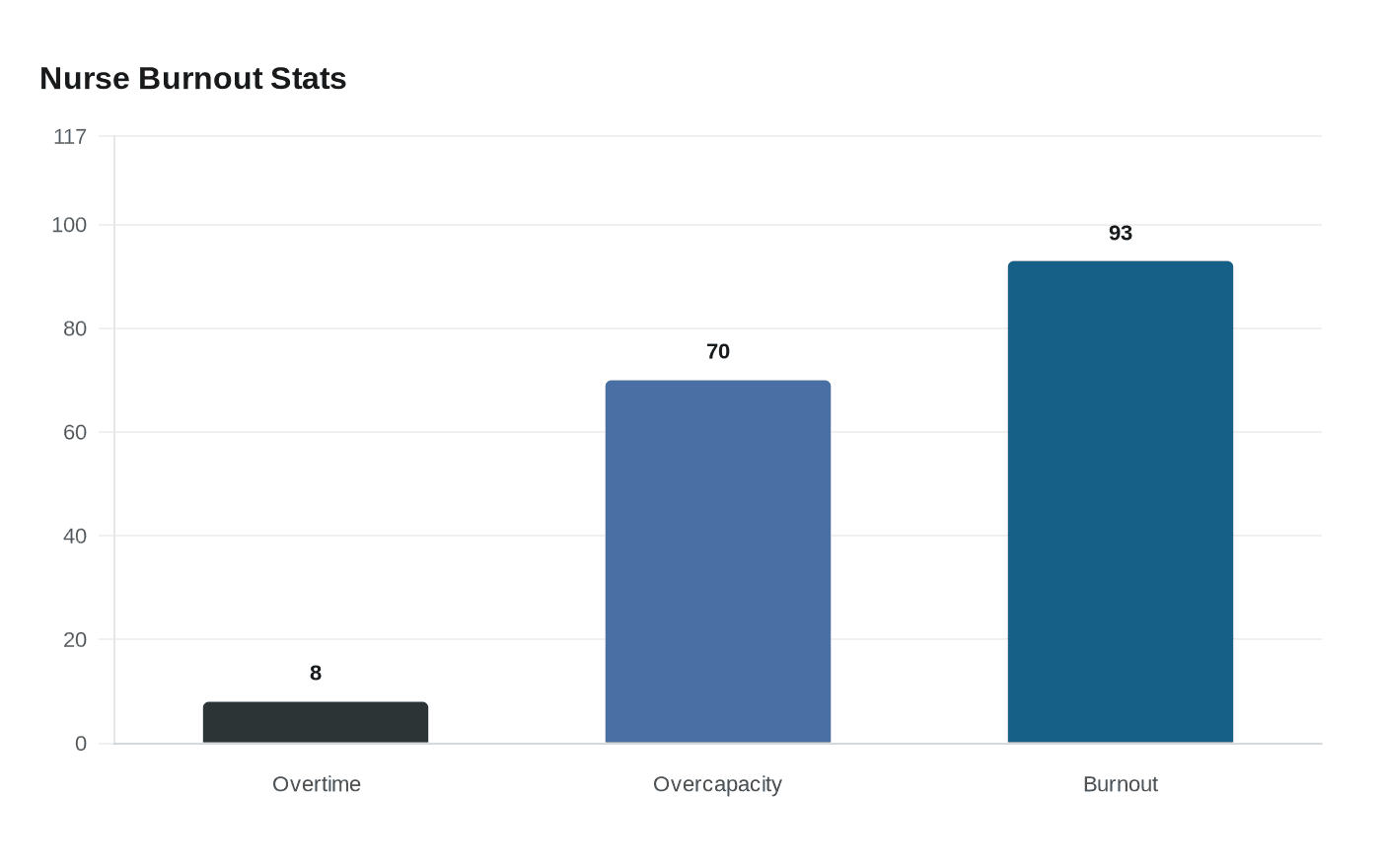
Health Canada said on March 4, 2024, that nurses are the country’s largest group of regulated health professionals, with more than 450,000 members, and that they were facing increased workloads, high rates of burnout, stress, anxiety and depression, and, in some cases, abuse. Statistics Canada had already reported in July 2023 that nurses were working harder and more hours amid a labour shortage. The Canadian Institute for Health Information later found that in 2023-2024, 8% of total hours worked by front-line providers in hospital nursing units were overtime hours. In other words, overtime was not a side issue. It was part of the daily operating model.
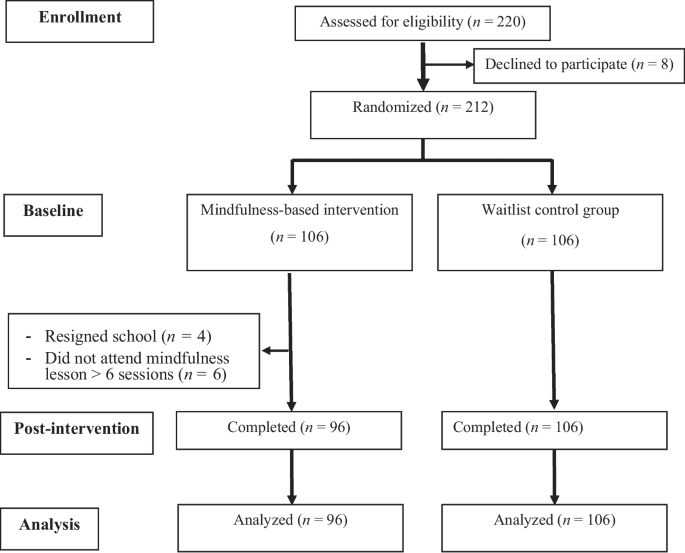
The Canadian Federation of Nurses Unions’ 2024 member survey, based on 5,595 nurses across Canada, put numbers to the strain. Union messaging said 7 in 10 nurses reported workplaces regularly operating over capacity, and about 93% reported symptoms of burnout. Nursing workforce forecasting cited in sector reporting has warned of a shortage of 60,000 nurses nationwide by 2022 and more than 117,000 by 2030, a gap that helps explain why wellness perks can feel so hollow on the floor. A meditation room does not change the fact that the next patient still needs triage, charting and hands-on care.
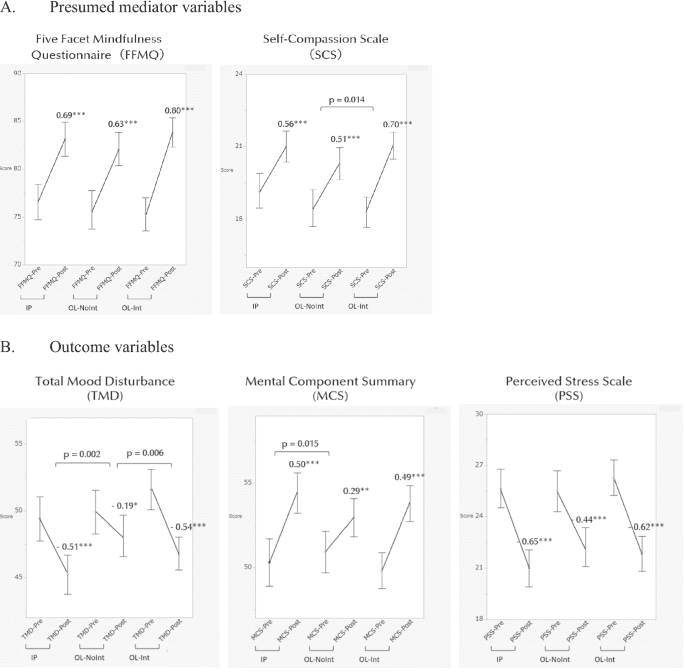
That does not mean mindfulness has no place in nursing. A 2023 systematic review found mindfulness-based interventions could reduce stress and fatigue among nurses, though the evidence was not strong enough to show clear effects on anxiety and depression. The National Center for Complementary and Integrative Health says mindfulness practices are generally low-risk and can be part of mindfulness-based stress reduction. But the real policy response in Canada has moved toward retention and workload fixes, not just coping tools. Health Canada launched a Nursing Retention Toolkit in 2024, and British Columbia introduced the country’s first minimum nurse-to-patient ratio policy in 2024 as part of an effort to improve job satisfaction and retention.
That is the divide Dr. Megan Miller’s argument exposes. Breathing exercises may help one nurse steady herself before walking back into a packed emergency department. They do not fill the vacancy, shorten the overtime list or make an overcapacity unit safe. On a floor where burnout is already measured in hours, symptoms and shortages, the real test is whether the system keeps asking nurses to meditate through what staffing, funding and safer workloads should have fixed.
Know something we missed? Have a correction or additional information?
Submit a Tip