Mindfulness interventions boost emotion regulation in mental health conditions
A 19-trial meta-analysis shows mindfulness can sharpen reappraisal and lower emotion dysregulation, but expressive suppression barely moved.

A closer read on the evidence
This is not another standalone mindfulness study. It is a systematic review and meta-analysis in JCPP Advances that asked whether mindfulness-based interventions actually improve emotion regulation in people with mental health conditions, and the answer was more specific than a broad wellness claim. Led by Thomas Easdale-Cheele, George Nash, Veronika Filobokova, Chloe Westbury, and Alessio Bellato, the review used a pre-registered protocol, PROSPERO CRD42024618605, and searched Web of Science, PsycINFO, Embase, and PubMed on 4 July 2025.
The team identified 19 randomized controlled trials in people diagnosed by trained healthcare professionals under DSM or ICD criteria. Sixteen trials, totaling 988 participants, fed the meta-analyses, and 50.71% of participants were randomized to mindfulness-based interventions. The paper was received on 29 September 2025 and accepted on 29 January 2026, but the bigger story is the design: this review was built to test whether mindfulness does more than feel calming on a good day.
What changed, and by how much
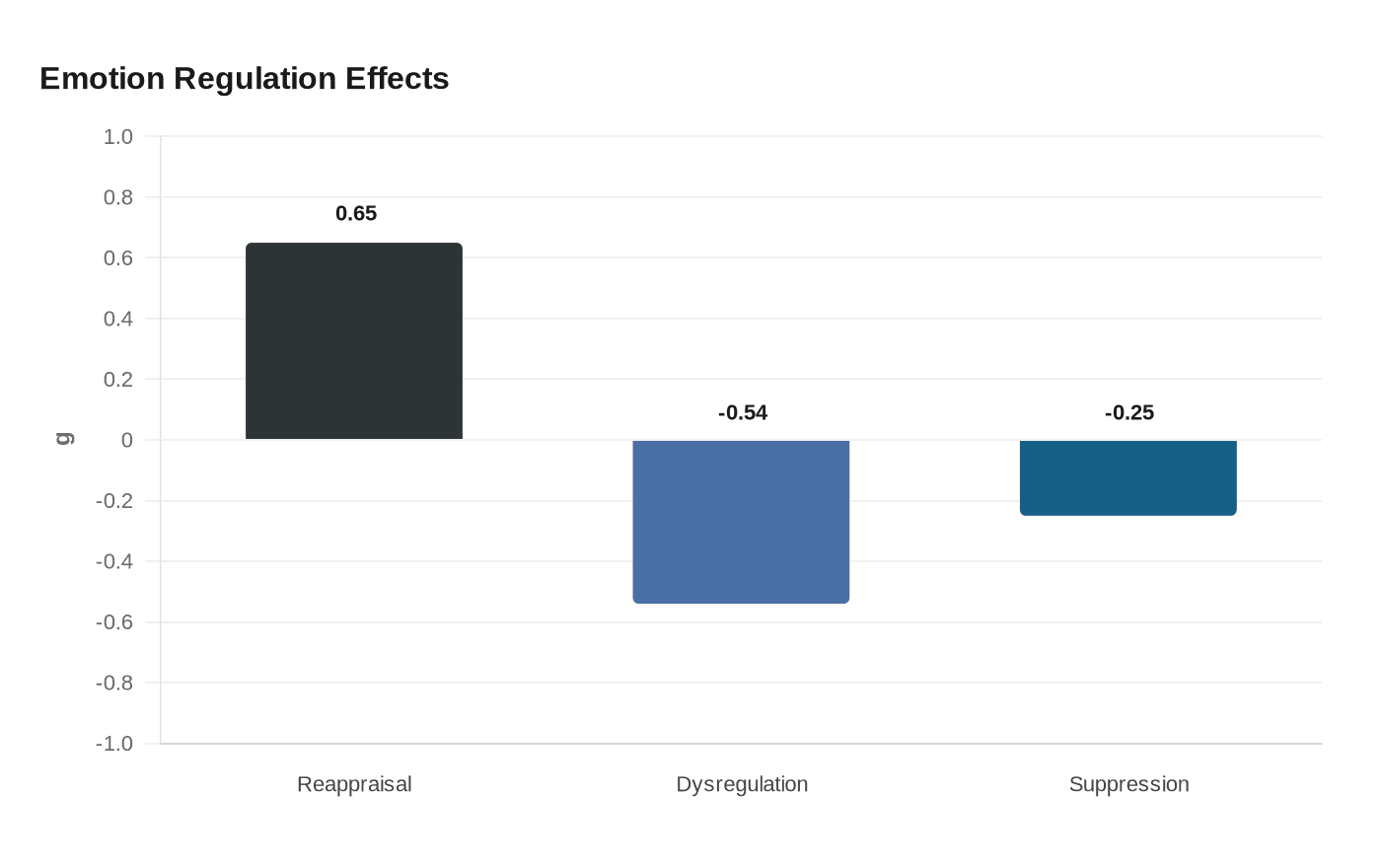
The clearest gain was cognitive reappraisal. Across six studies, mindfulness-based interventions improved it with g = 0.65, a solid effect that points to a better ability to reinterpret stress, discomfort, or a troubling thought rather than getting trapped inside it. That matters in daily life because reappraisal is the skill that turns a spike of panic into a sentence you can examine instead of a wave that sweeps you away.
Overall emotion dysregulation also improved, with g = -0.54 across nine studies. The gains were not vague either: they showed up in goal-directedness, impulsivity, and access to emotion-regulation strategies. In practical terms, that means mindfulness was associated with more room to stay oriented to a task, less hair-trigger reaction, and a greater ability to reach for coping tools when feelings were already running hot.
Where the signal was weaker
Not every regulation pathway moved. Expressive suppression, the habit of holding emotions in, did not show a significant effect, with g = -0.25 and a wide confidence interval from -0.94 to 0.45. That wide spread, plus significant heterogeneity, says the studies did not line up cleanly on this outcome, so the evidence is much less convincing than it is for reappraisal or overall dysregulation.
Study quality also significantly moderated both emotion regulation outcomes, which is a crucial caution flag. The strongest benefits were not evenly distributed across all trials, so the most responsible reading is that higher-quality studies carry more weight than the pooled average alone. For anyone deciding whether mindfulness belongs in a treatment plan, the message is to favor well-designed programs and realistic goals over inflated promises.
Why this matters in real care
The World Health Organization says that in 2021 nearly 1 in 7 people worldwide, or about 1.1 billion people, were living with a mental disorder, with anxiety and depressive disorders the most common. That scale is why emotion regulation has become such a practical target: if feelings are overwhelming, treatment often needs tools that help people stay steady long enough to use the rest of care.
Mindfulness fits that role because it is low-cost, non-invasive, and easy to layer onto therapy rather than replace it. The new meta-analysis suggests it is most useful as a complement when the real problem is emotional reactivity, not as a cure-all for every symptom or every coping style. If your goal is to pause before acting, rethink a spiral, or build a little more breathing room around distress, the evidence points in that direction.
The clinical lineage behind the modern wave
This work also sits on top of a long clinical tradition. Mindfulness-Based Stress Reduction, the original eight-week program developed by Jon Kabat-Zinn at the University of Massachusetts Medical Center in 1979, still shapes how mindfulness is taught in clinics, wellness settings, and hybrid groups today. That history matters because the field is no longer just asking whether mindfulness can soothe people in theory, but whether a structured, repeatable practice can move measurable mental health outcomes.
The answer from this review is yes, with limits. The intervention family appears to help people change how they handle emotion, but the effect depends on the outcome you are measuring and the quality of the study behind it. That makes it a mature finding rather than a glossy one.
How this fits the wider research
The new review does not stand alone. Earlier work has described mindfulness mechanisms such as attention regulation, body awareness, and changes in reappraisal, all of which fit the pattern seen here. A 2024 meta-analysis of mindfulness-based emotion regulation strategies pooled 110 studies and 8,105 participants and found a significant overall effect of g = 0.28, while another meta-analysis on mindfulness, cognitive reappraisal, and expressive suppression included 36 studies, 83 effect sizes, and 12,026 subjects.
Taken together, those numbers show a field that has moved well past anecdote. The newer JCPP Advances review narrows the claim to what is most defensible: mindfulness seems to help people reframe experience and reduce dysregulation, but it does not reliably change every strategy the same way.
What the size of the practice says about the moment
The broader culture around meditation keeps expanding, too. The National Center for Complementary and Integrative Health says U.S. adult meditation use rose from 7.5% in 2002 to 17.3% in 2022, and a 2024 study from the University of Bath and the University of Southampton found that just 10 minutes of daily mindfulness practice can improve wellbeing and reduce depression and anxiety. That makes the newest review especially useful, because it helps separate a short, realistic practice from a vague sense that mindfulness should fix everything.
For readers weighing whether to add mindfulness to therapy, the cleanest takeaway is this: the evidence supports it as a targeted aid for cognitive reappraisal and broader emotion regulation, with the strongest caution around expressive suppression and study quality. Mindfulness is not a magic reset, but it does look like a practical tool for helping people catch emotion before it takes the wheel.
Know something we missed? Have a correction or additional information?
Submit a Tip

