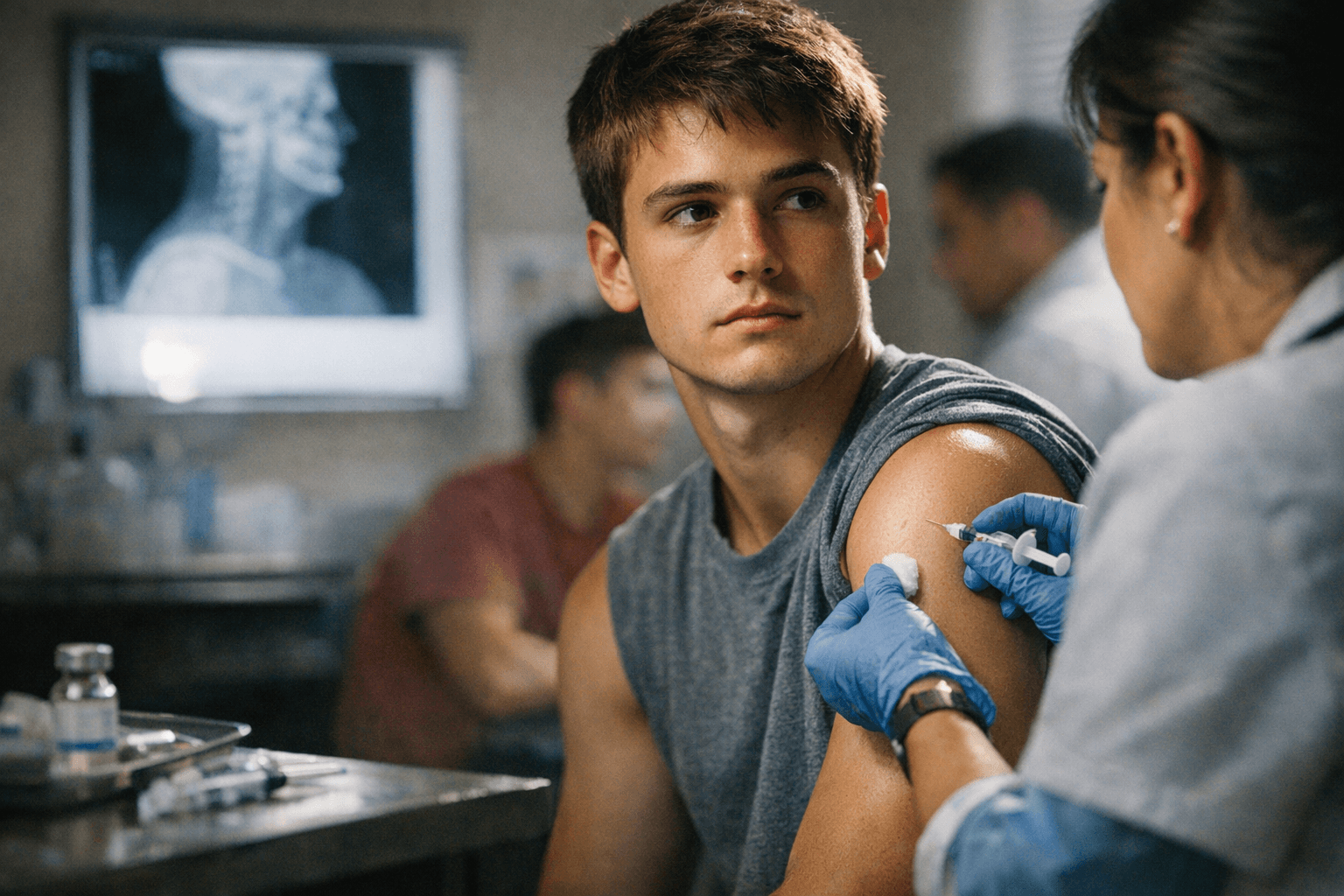
HPV vaccination may protect young men from multiple cancers
The first boys vaccinated against HPV are now showing lower cancer risk as young men, a finding that could narrow the long-standing uptake gap.
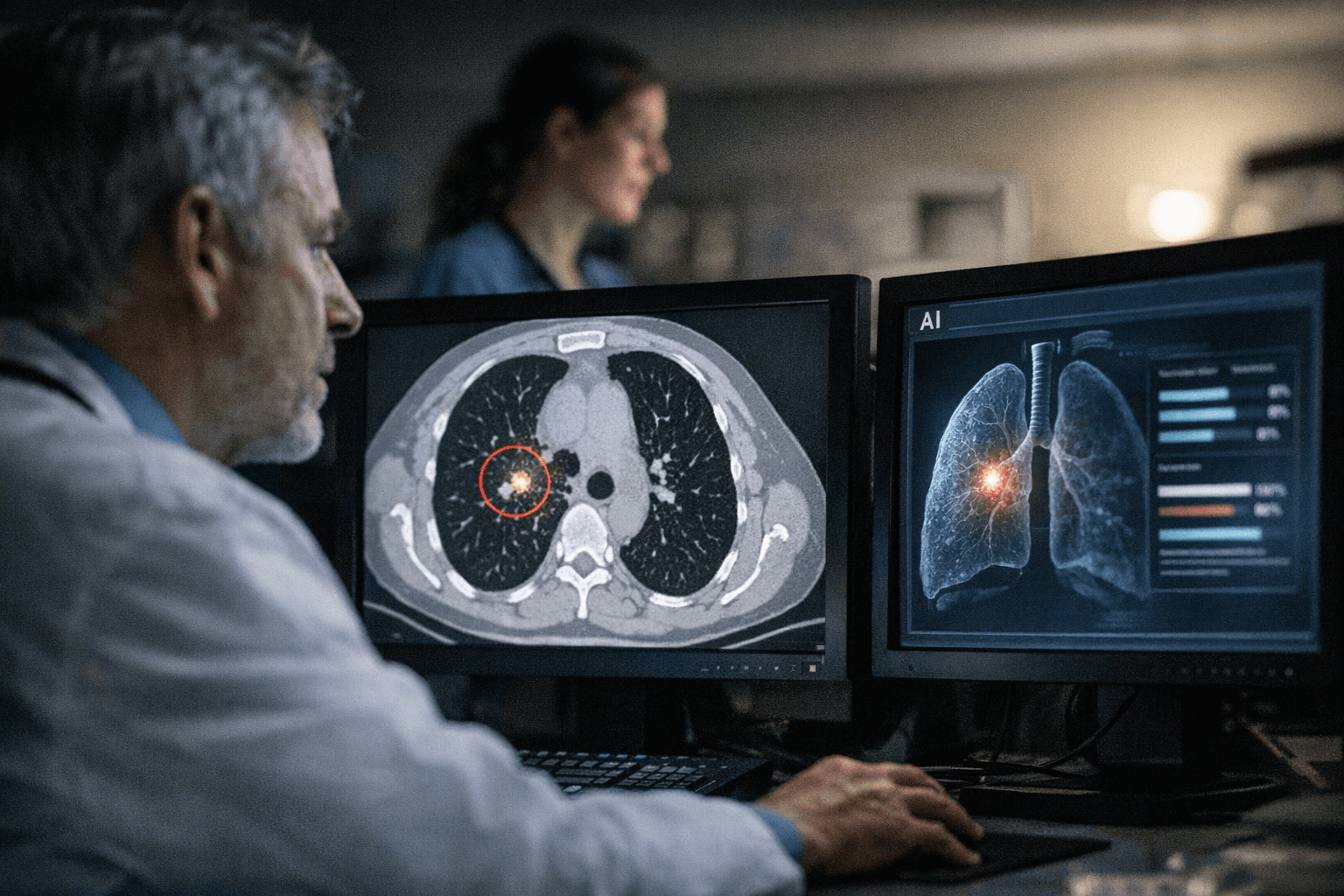
A generation of boys vaccinated against human papillomavirus is now old enough to show whether the shot does more than block infection. A new study in JAMA Oncology found that young men who received the 9-valent HPV vaccine had a lower risk of HPV-related cancers, including head and neck, esophageal, anal and penile cancers, strengthening the case for routine immunization as a cancer-prevention tool.
The analysis followed males ages 9 to 26 and compared 615,155 vaccinated with 2,290,623 unvaccinated before propensity score matching. After matching, 510,260 participants remained in each group. The vaccinated group had a lower risk of the composite cancer outcome, with a hazard ratio of 0.54, and the association remained significant in both the 9 to 14 and 15 to 26 age bands. That matters because HPV-linked cancers are still rare before age 50, yet the signal is appearing early enough to suggest that childhood and adolescent vaccination may prevent disease long before men would normally expect to see benefit.
Public-health officials have spent years trying to move HPV vaccination beyond its original association with cervical cancer. The Centers for Disease Control and Prevention estimates 49,908 new HPV-associated cancers each year in the United States from 2018 to 2022, including 22,827 among males. Among men, oropharyngeal cancers are the most common HPV-associated cancers, making the male cancer burden impossible to dismiss as incidental. The Advisory Committee on Immunization Practices recommended routine HPV vaccination for females starting in 2006 and for males in 2011, and current CDC guidance calls for routine vaccination at ages 9 to 12, catch-up through age 26, and shared clinical decision-making for adults ages 27 to 45.
The policy challenge is uptake. In 2024, only 63% of U.S. boys and girls ages 13 to 17 completed the HPV vaccination series, still well short of the Healthy People 2030 target of 80%. A 2025 joint statement from 62 NCI-designated cancer centers and other organizations said more than 40,000 cancers and hundreds of thousands of precancers in the United States are caused by HPV each year and are almost entirely preventable with timely vaccination. That gap between what medicine can prevent and what adolescents actually receive remains the central obstacle.
Cancer specialists have been pressing the same point. In a 2024 American Cancer Society summary of a study involving almost 3.5 million people, Glenn J. Hanna, MD, said the evidence showed that in boys and men, vaccination decreases the risk of HPV-related oropharyngeal head and neck cancers. The latest findings extend that argument across multiple cancers and give health systems a clearer reason to treat HPV vaccination as routine cancer prevention, not only as protection against a sexually transmitted infection.
Know something we missed? Have a correction or additional information?
Submit a Tip