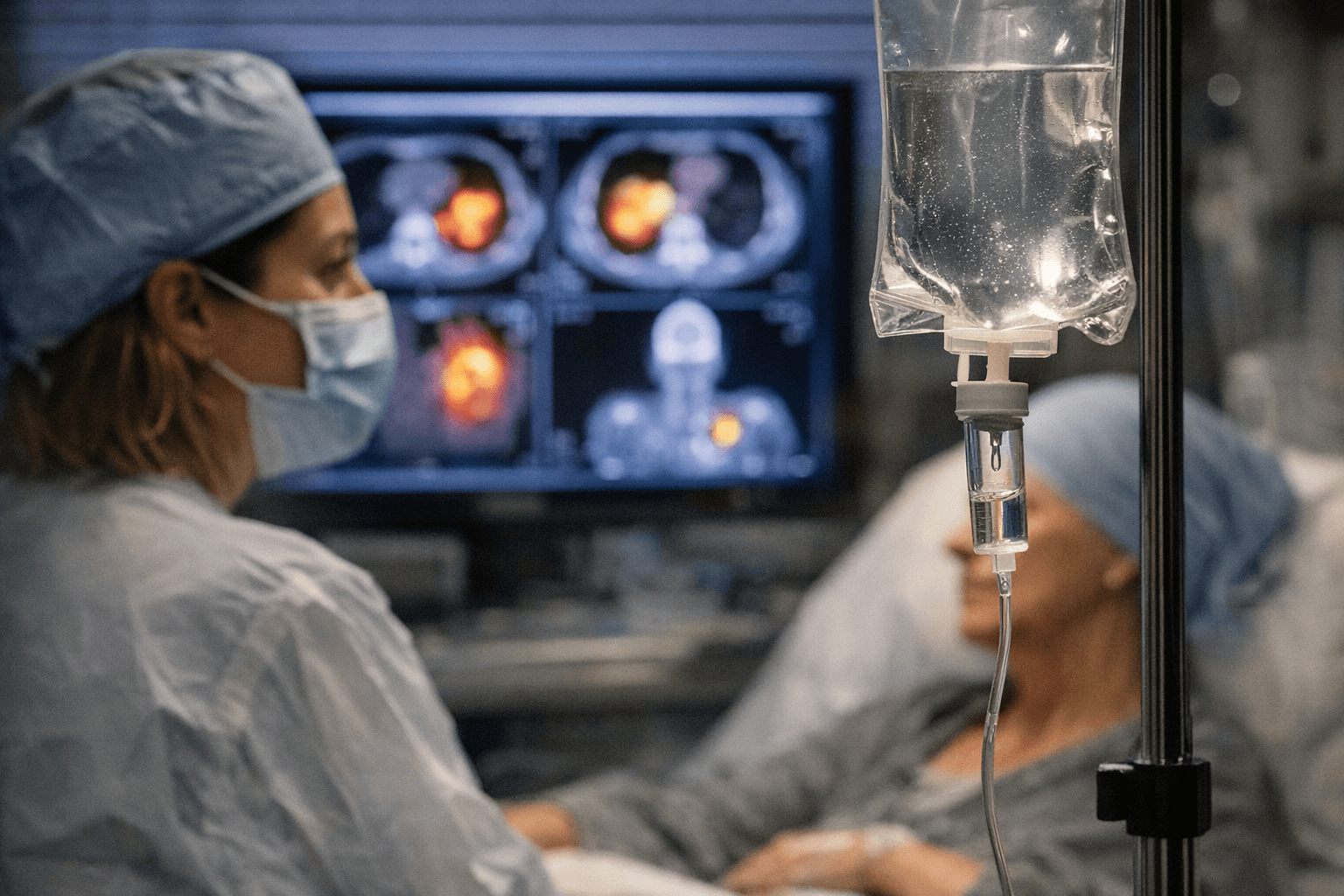
Immunotherapy is eliminating some cancers, raising hopes and questions
Some tumors are disappearing with immunotherapy, but the biggest wins are still limited to tightly selected cancers and patients. The breakthrough is real, yet access and proof remain the hard part.
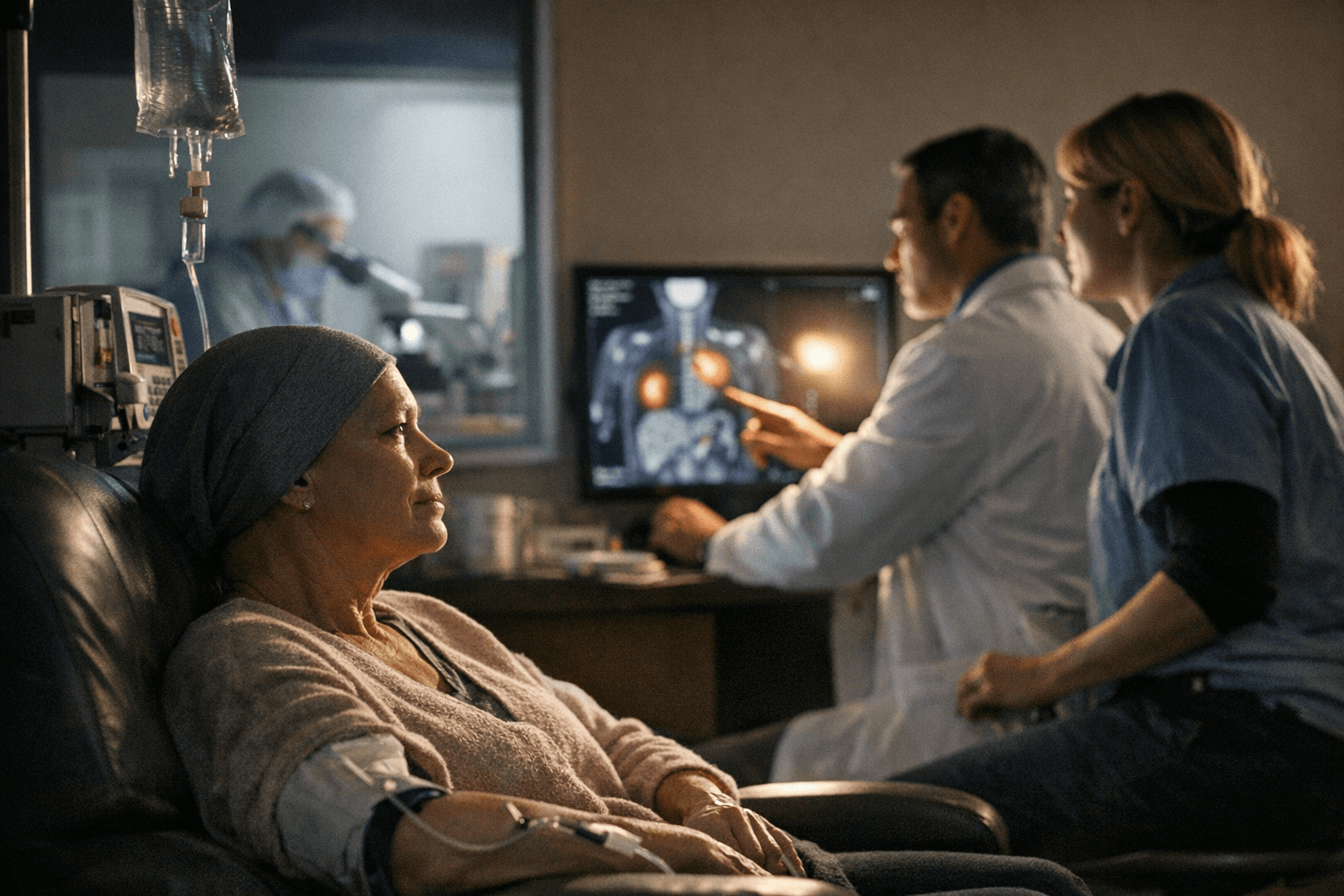
The clearest proof that tumors can vanish
Tumors are disappearing in some patients, but not because immunotherapy has become a universal cure. The strongest results are showing up where the cancer’s biology gives the immune system a clear target, especially in mismatch repair-deficient, or MMRd, tumors.
At Memorial Sloan Kettering Cancer Center, a larger trial reported in April 2025 found that nearly 80% of 103 patients with MMRd cancers were successfully treated with immunotherapy alone, without surgery, chemotherapy, or radiation. The group ranged from 26 to 87 years old and included rectal, gastric, colon, esophageal, urothelial and other cancers. In the earlier rectal-cancer experience, every rectal patient had no detectable tumor after treatment, a result that is rare enough to sound almost implausible until the pathology says otherwise.
That matters because these are not minor clinical tweaks. For some of the people who responded, avoiding surgery meant avoiding ostomy bags, and avoiding radiation and chemotherapy meant preserving sexual function and daily quality of life. Maureen Sideris, one of the patients who responded, said she had “no evidence of cancer” and felt like she had “won the lottery.”
Where the promise is strongest
The National Cancer Institute has been careful not to oversell the moment. Its guidance says that for some people with earlier-stage cancers, a short course of immune checkpoint inhibitor treatment may be all they need to eliminate their cancer, but it also stresses that much more research is needed before that becomes routine care.
That caution is important because immunotherapy does not behave like a standard one-size-fits-all drug. It can work spectacularly well in one subgroup and fall short in another, even within the same disease category. The MMRd results are among the most striking examples because they suggest that, when the tumor is biologically vulnerable, the immune system can sometimes finish the job without the usual stack of local and systemic treatments.
Andrea Cercek of Memorial Sloan Kettering called the result “very exciting,” and said it shows that a broad range of MMRd tumors can be treated with immunotherapy instead of surgery and radiation. Luiz Diaz Jr. is among the clinicians associated with this line of work, which has helped move the field from theory into measured, repeatable clinical results.
A second lane of progress in metastatic gastrointestinal cancer
Another important signal came from the National Cancer Institute on April 1, 2025. Researchers reported that a new form of tumor-infiltrating lymphocyte therapy, or TIL therapy, combined with pembrolizumab produced substantial tumor shrinkage in nearly 24% of patients with metastatic gastrointestinal cancers. The same study found a 7.7% response rate with selected TIL therapy without pembrolizumab, and no objective responses with unselected TILs.
The trial enrolled 91 patients with esophageal, stomach, pancreatic, colon and rectal cancers that had already worsened after a median of four prior treatment regimens. That detail matters: this was not an easy population, and many participants had already exhausted standard options. Steven A. Rosenberg described TIL therapy as seeing “a little crack in the solid wall of cancer,” a reminder that even partial responses in advanced disease can be meaningful when the alternative is progression.
The result also shows how far the field still has to go. A 24% response rate is a real advance in a heavily pretreated group, but it also means most patients did not see major shrinkage. That gap between dramatic success and modest benefit is the central reality check in immunotherapy today.
Head and neck cancer shows how durable gains can be
One of the biggest signs that immunotherapy is moving earlier in treatment came from a 2025 phase III trial in newly diagnosed, locally advanced head and neck cancer. The Keynote-689 study, run across 714 patients at 192 sites in 24 countries, found that pembrolizumab given before and after standard treatment kept cancer at bay for an average of 60 months, compared with 30 months for standard care alone.
Researchers also reported a 10% reduction in the risk of cancer returning elsewhere in the body after three years. In a disease where standard care had not changed for more than 20 years, that is a major shift. It suggests immunotherapy is no longer only a rescue treatment for late-stage disease, but can be layered into curative-intent care to extend the disease-free window.
Why this is still not routine medicine
Even with these results, the practical barriers remain substantial. The patients most likely to benefit are still a selected minority, defined by biomarkers such as MMR deficiency or by the ability to harvest and expand tumor-infiltrating lymphocytes. In other words, the treatment works best when doctors can match the drug to the tumor’s biology.
There is also a geography problem. Some of the most sophisticated immune therapies are concentrated in large academic centers and trial networks, not in every hospital where cancer is treated. The head and neck study alone spanned 192 sites across 24 countries, which shows the scale needed to test these regimens properly. That breadth is encouraging, but it also underscores how specialized the delivery model still is.
The broader field has already shown what immune therapy can do in blood cancers and melanoma, but solid tumors remain harder to crack. Response variability, resistance, and the need for better biomarkers still limit widespread success. Nature also reported in February 2025 a record 19-year remission after CAR-T therapy, a striking reminder that some immune-based responses can be extraordinarily durable once the right target is found.
The line between breakthrough and routine is still being drawn. For now, immunotherapy is eliminating tumors in a narrow but growing set of cancers, and the central question is no longer whether the immune system can do this at all. It is which patients can access it, which tumors will respond, and how quickly the field can turn rare victories into standard care.
Know something we missed? Have a correction or additional information?
Submit a Tip