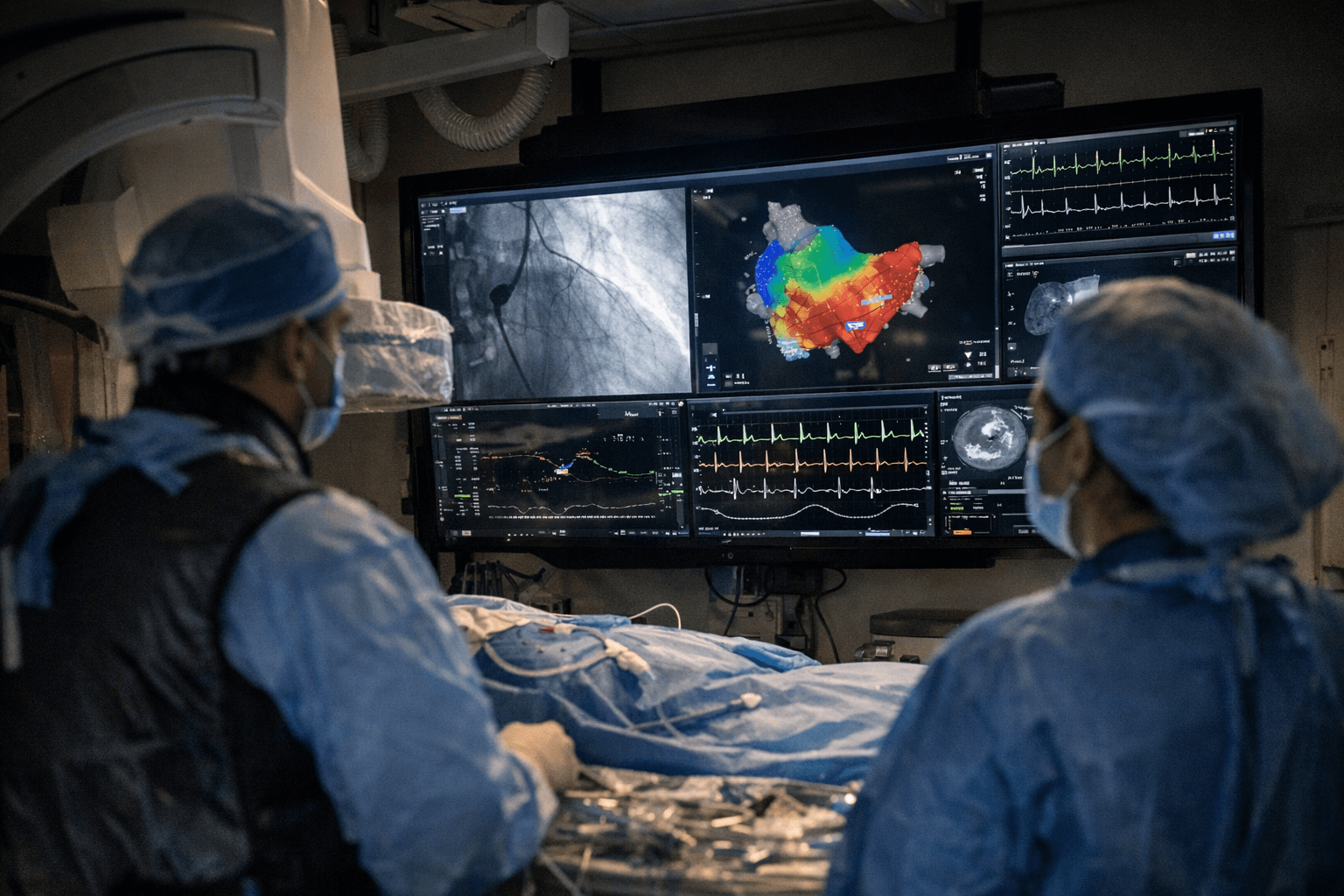
Medicare Advantage Payments Jump 5%, Boosting UnitedHealth and Humana Shares
The finalized 5% total Medicare Advantage rate increase for 2027, including a 2.5% risk adjustment boost, sent Humana shares up 13% in after-hours trading.

The Trump administration delivered a far larger Medicare Advantage payment increase than Wall Street had anticipated, sending shares of the nation's biggest health insurers surging and offering a critical financial lifeline to an industry that has been bleeding losses for two years.
The Centers for Medicare & Medicaid Services finalized a 2.48% average payment increase for 2027 Medicare Advantage plans, amounting to more than $13 billion in additional government payments. A separate 2.5% boost tied to changes in risk assessment payments for health status pushed the total effective rate increase to approximately 5%, a dramatic reversal from the near-flat 0.09% hike, worth roughly $700 million, that the agency had proposed in January 2026.
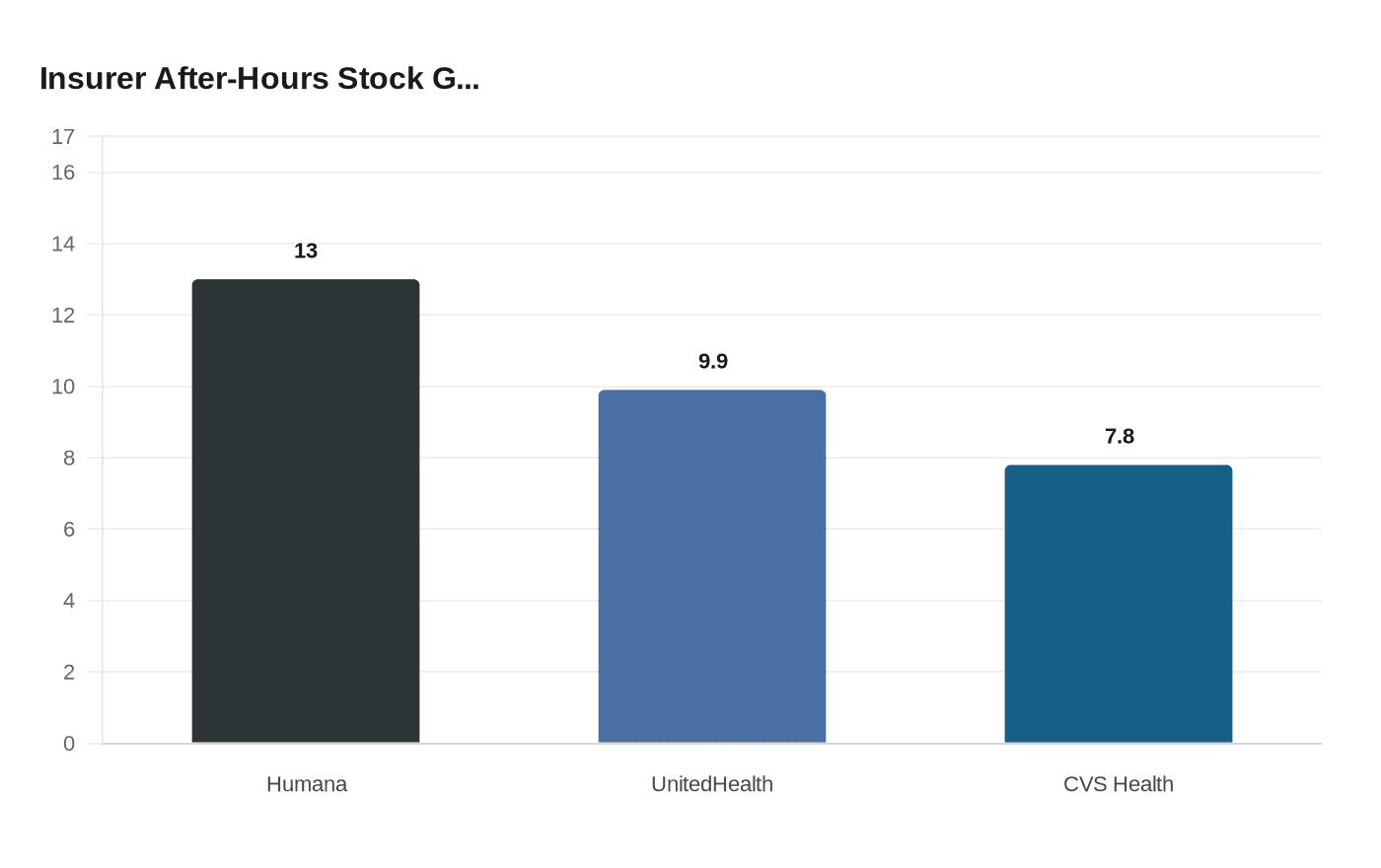
The announcement triggered sharp after-hours gains Monday. Humana jumped approximately 13%, UnitedHealth Group rose roughly 9.9%, and CVS Health climbed about 7.8%, erasing much of the losses sustained after January's advance notice rattled investors.
CMS Administrator Dr. Mehmet Oz framed the finalized rates in patient terms. "Medicare Advantage and Part D should work for the people who rely on them," he said in an official statement. "These updates keep coverage affordable and ensure patients get real value from their plans."
The administration also scrapped a January proposal that would have recalibrated the risk adjustment model using more current actuarial data: 2023 diagnosis records and 2024 expenditure data rather than the 2018 and 2019 data previously used. Insurers had argued the shift would have cost them billions of dollars by restricting how certain diagnoses counted toward risk scores.
The financial stakes extend far beyond any single insurer's balance sheet. CMS's annual payment policy influences how more than half a trillion dollars flow through private health plans, a figure that reflects Medicare Advantage's transformation into the dominant form of Medicare coverage. Enrollment reached a record 35.4 million beneficiaries in 2026, representing 51% of the 69 million Medicare-eligible individuals, up from just 19% of the eligible population in 2007.
Monday's decision arrived after two years of severe financial pressure across the sector. Aetna, CVS Health's insurance arm, swung from a $3.9 billion profit in 2023 to a $984 million loss in 2024. Humana's operating income fell 51% last year. UnitedHealth Group, the largest Medicare Advantage insurer by enrollment, posted a 16% decline in 2025 net earnings to $12.1 billion, down from $14.4 billion the year before.
That strain drove a wave of benefit cuts and market exits heading into 2025. More than 1.8 million Medicare Advantage members saw their 2024 plans discontinued, with Humana, CVS Aetna, and UnitedHealthcare collectively displacing over 1.2 million members through closures and market withdrawals.
Humana, which concentrates its business primarily in Medicare Advantage, remains more exposed to rate volatility than UnitedHealth Group or CVS Health, both of which have broader business lines to cushion losses. The 13% after-hours gain reflects how significantly Monday's rate decision moves the needle on Humana's recovery outlook.
The 2027 finalized rate follows a now-familiar pattern. In 2026, CMS proposed an increase of just 2.2% before finalizing at 5.06%. This year's final rate of 2.48% falls below that 5.06% benchmark, but the gap between January's proposal and Monday's decision tells a similar story of the final rule arriving substantially more favorable to insurers than its advance notice suggested.
Sources:
Know something we missed? Have a correction or additional information?
Submit a Tip