Mindfulness intervention may restore brain reward function in cannabis use disorder
A 2-week mindfulness trial is testing cannabis treatment at the level of brain reward circuitry, not just mood. It is a rare, rigorous fMRI design for a field that has long leaned on self-report.
A new kind of mindfulness evidence
The most interesting thing about this trial is not that it asks whether mindfulness feels calming. It asks whether a 2-week mindfulness-based intervention can shift the brain reward system in cannabis use disorder, using a double-blind, active-and-passive randomized controlled fMRI design. That is a much harder test, and it matters because reward circuitry sits near the center of craving, reinforcement, habit formation, and relapse.
Cannabis use disorder affects about 50 million people worldwide, and cannabis use is associated with alterations in brain reward pathways. The trial’s premise is simple but ambitious: if mindfulness can change the way reward cues register in the brain, it may do more than help people relax. It could become a treatment tool aimed at the compulsive pull of use itself.
Why reward function is the story
In addiction research, reward function is not an abstract neuroscience phrase. It is the machinery behind why a person may genuinely want to cut back and still get pulled back by cue-driven behavior. If the brain becomes less responsive to ordinary rewards and more reactive to cannabis-related cues, then willpower alone has to fight uphill against a reinforced habit loop.
That is why the study’s focus on reward function is so important for cannabis dependence. A mindfulness intervention that meaningfully changes reward processing would suggest a mechanism, not just a feeling. It would point to a practical path for treatment planning, one where meditation is treated as a targeted behavioral intervention with brain-level effects.
Why this trial stands out in mindfulness science
Mindfulness research has often been strongest in the realm of self-report: stress feels lower, mood improves, craving softens. Those outcomes matter, but they do not tell the whole story. By using fMRI, the researchers are looking for neural mechanisms rather than relying only on what participants say they feel.
The design is unusually rigorous for this corner of the field. An active control helps separate mindfulness-specific effects from attention, expectation, and the simple experience of being enrolled in a program. A passive control shows what changes happen when someone waits or continues usual care. Put together, those comparisons make the study much better suited to answer a clinical question: is mindfulness doing something distinct, or is it just another supportive structure?
That is why the trial feels like a threshold moment. It reflects a broader shift in mindfulness science toward measurable brain systems, especially when the goal is to understand addiction.
What the existing evidence says
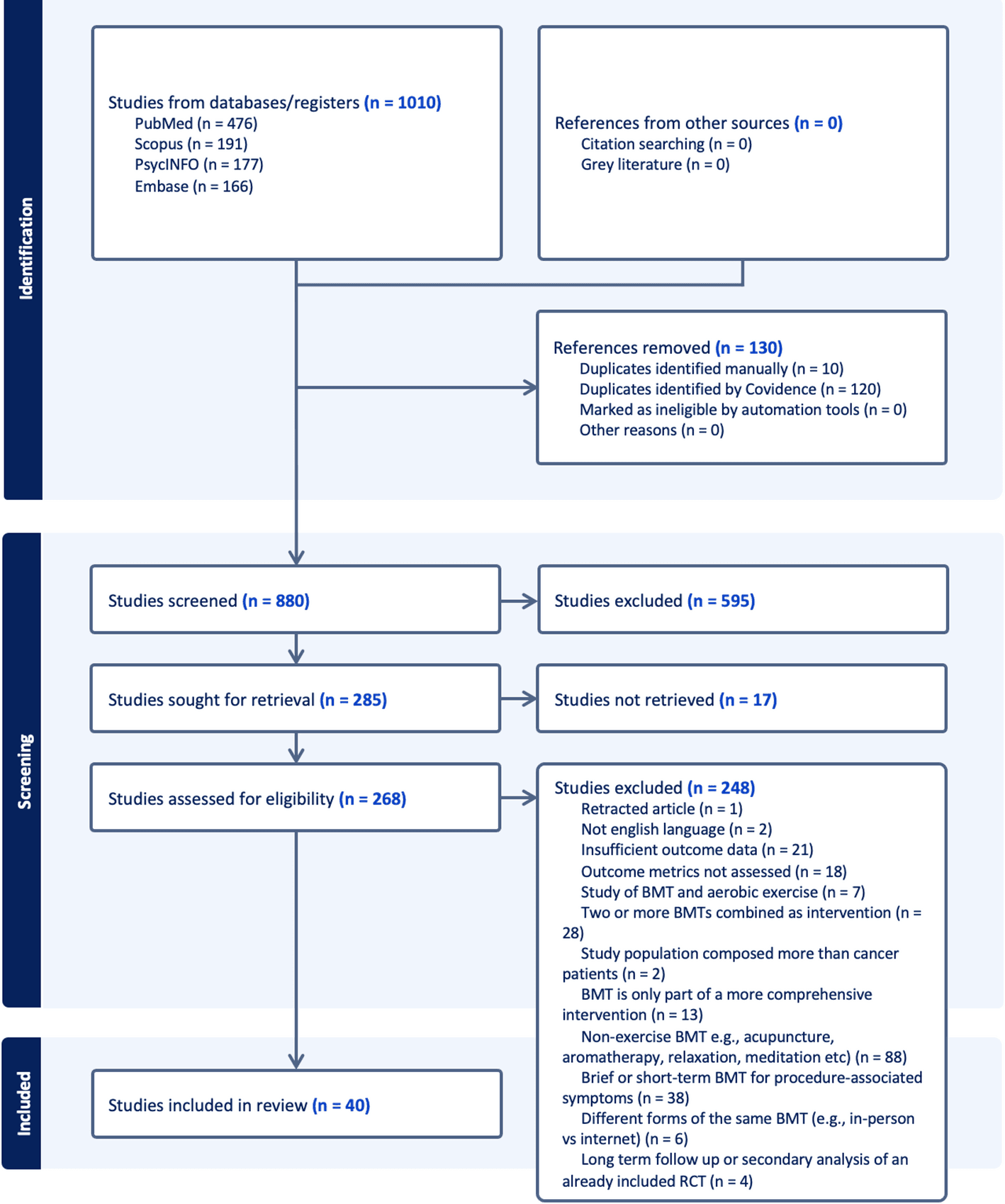
The new trial also lands in a literature that has been thin on mechanistic brain data. A 2023 systematic review of fMRI studies of mindfulness-based interventions in substance dependence found only seven qualifying studies. Those studies were limited to six tobacco studies and one opioid study, not cannabis. The review concluded that the evidence base was still limited.
Even so, the earlier work pointed in a useful direction. The reported brain changes involved the anterior cingulate cortex and striatum, and those changes were correlated with greater mindfulness, lower craving, and lower drug quantity. In other words, there is already a hint that mindfulness may connect with the circuits that matter most in compulsive use. What has been missing is a cannabis-specific trial designed to test that idea directly.

This is why the 2-week cannabis study matters so much. The authors say mindfulness-based interventions had not previously been investigated for effects on cannabis use disorder or brain reward function. That makes the trial feel less like a follow-up and more like a first serious probe into a major unanswered question.
Why cannabis reward circuitry makes mindfulness plausible
A review of brain reward function in cannabis users helps explain why this target is so compelling. Cannabis use can be associated with lower sensitivity to natural rewards, paired with higher sensitivity to cannabis-related rewards. That combination is exactly the kind of imbalance that can keep a habit alive.
If everyday rewards feel muted and cannabis cues feel loud, then the brain is not simply chasing pleasure. It is stuck in a distorted reward landscape. Mindfulness, at least in theory, may help by changing how attention and reactivity are organized around those cues. The point is not that meditation erases craving. The point is that it may alter the circuitry that makes craving so sticky in the first place.
What this does, and does not, prove
This trial is exciting, but it should be read carefully. A rigorous design can tell us whether a mindfulness-based intervention moves reward-related brain signals in a cannabis-use sample. It cannot by itself prove that every meditator will benefit, or that a short course of mindfulness will work the same way for everyone.
It also does not mean mindfulness is a stand-alone fix for cannabis use disorder. Cannabis dependence is shaped by many factors: severity of use, environment, stress, co-occurring mental health conditions, and access to care. A brain-based finding would strengthen the case for mindfulness as part of treatment, not as a replacement for broader support.
For everyday meditators, the takeaway is narrower but useful. This research is not evidence that a few weeks of practice will “repair” the brain in any general sense. It is evidence that scientists are now testing whether mindfulness can alter a specific biological pathway tied to addiction. That is a much more concrete claim than the usual wellness language.
The public-health backdrop
The larger scale of the issue explains why researchers are pressing into this territory. The World Health Organization says about 147 million people, or 2.5% of the world population, consume cannabis annually. The National Institute on Drug Abuse, part of the National Institutes of Health, funds research on the health effects of cannabis products and the public health impacts of cannabis policies, including prevention and treatments for cannabis use disorder.
So the stakes are not theoretical. If a mindfulness-based intervention can affect reward function in cannabis use disorder, it could add a low-cost, behaviorally grounded option to a treatment landscape that still needs more tools. The real value of this trial is not that it crowns mindfulness as a cure. It is that it tests whether meditation can earn its place inside the circuitry of recovery.
Know something we missed? Have a correction or additional information?
Submit a Tip