Mindfulness Training Boosts CBT Outcomes for Patients With Dissociative Symptoms
Adding mindfulness to CBT matched, not exceeded, CBT plus exercise for dissociation in 104 patients; the Oldenburg feasibility trial shows how low-intensity MBT can slot into inpatient workflows.

Researchers at Carl von Ossietzky University of Oldenburg published a controlled pseudo-randomized trial on March 31 testing one of the more stubborn clinical questions in psychiatry: does adding Mindfulness-Based Training to standard cognitive-behavioral therapy actually reduce dissociative symptoms better than CBT paired with a credible alternative? The answer, for now, is a qualified no, and the study is more instructive for what else it found.
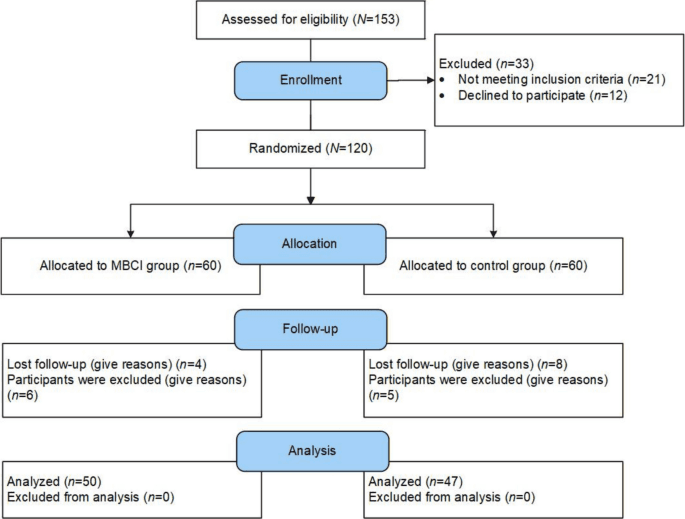
Federica Fedyk, Burkhard Croissant, C. Schulz, and René Hurlemann enrolled 104 patients presenting with dissociative symptoms and assigned them to either MBT combined with CBT or CBT combined with guided physical exercise as an active control. Both groups were tracked using the Dissociative Experiences Scale-II (DES-II), the field's standard transdiagnostic measure for dissociation severity, with the research team pre-registering their design, analysis plan, and reporting criteria before data collection began.
The primary result was a draw on paper but meaningful in context: MBT plus CBT did not outperform the exercise-augmented CBT group. Both conditions produced modest DES-II improvements across the treatment period. The null headline, however, sits alongside a finding clinicians building inpatient programs will find useful: low-intensity MBT was feasibly and safely integrated into a psychiatric inpatient workflow without adverse events, adding to a thin but growing evidence base.
The Oldenburg team flagged a specific patient cohort where mindfulness training may carry practical advantages regardless of direct efficacy comparisons: those with limited mobility or health contraindications that make structured physical activity impossible. For that population, MBT slots into the adjunct role that exercise otherwise fills, giving clinicians a workable alternative rather than a treatment gap.
Exploratory moderation analyses identified sex and the personality trait antagonism as potential moderators of treatment response, suggesting not all 104 patients responded equivalently. These findings were not pre-registered and require independent replication before clinicians can act on them, but they point toward the more pressing research question: which patients benefit most from MBT as an add-on, and through what mechanism. The theoretical framework leans on mindfulness strengthening present-moment awareness, reducing experiential avoidance, and rebuilding emotion-regulation capacities that dissociation disrupts, though the current data do not isolate those pathways causally.
The authors recommend careful clinical supervision and trauma-informed adaptation when delivering mindfulness protocols to patients with active dissociative profiles. Intensive or unguided practice carries risk in this population, and the low-intensity structure used in the Oldenburg protocol reflects that consensus deliberately. Practitioners working outside controlled inpatient settings should not treat this as a green light for standard MBSR or MBCT delivery without modification.
For the field, the study's honest null on efficacy is paired with its strongest contribution: an articulation of what a feasibility trial in this diagnostic space should look like, complete with a transdiagnostic recruitment frame and pre-registered methodology. Future controlled trials with larger samples and more refined active controls will be positioned to isolate what, precisely, mindfulness adds beyond general therapeutic engagement.
Know something we missed? Have a correction or additional information?
Submit a Tip