Therapeutic scuba‑diving plus mindfulness reduces emotional eating and stigma in adults with obesity, randomized trial
Scuba diving plus mindfulness cut emotional eating scores 3x more than standard care in a 63-person randomized trial, with effects lasting 8 months.

Karolina Griffiths, Thibaut Markarian, Vincent Meurice, and their team published results in PLOS ONE on March 27, 2026 that most mindfulness practitioners would not have predicted: two months of structured underwater scuba sessions woven with formal mindfulness exercises reduced emotional eating significantly more than standard obesity care alone, and that advantage held at both five- and eight-month checkpoints.
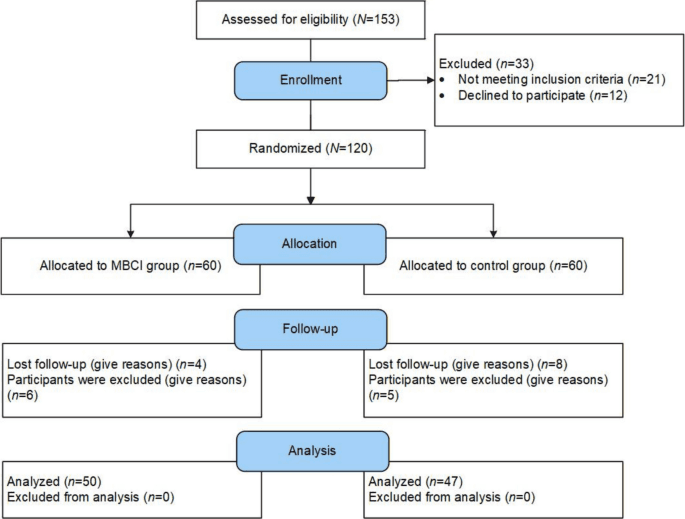
The trial recruited 63 adults with a BMI above 30 in Montpellier, France, randomizing participants between July and August 2022. Fifty-five entered the final analysis, a group that was 87.3 percent female with a median age of 46. The intervention arm combined the Bathysmed® therapeutic scuba-diving protocol with mindfulness practice and standard dietary and psychological support. The control group received standard care only.
The primary measure was the Dutch Eating Behaviour Questionnaire emotional eating subscale, a validated instrument tracking the tendency to eat in response to negative emotions. At two months, intervention-group scores dropped by a mean of 0.82 points (SD 0.81) against the control group's 0.27 (SD 0.61), a difference that reached p = 0.004. The intervention arm also showed reductions in weight self-stigma and stress alongside improvements in quality-of-life measures.
What the underwater environment contributes to those numbers is worth separating from the mindfulness component. Breath control below the surface is not aspirational; it is structural. Scuba divers must regulate inhalation and exhalation to manage buoyancy and air supply, which enforces the slow, deliberate diaphragmatic breathing that mindfulness instructors spend whole sessions trying to cultivate on a cushion. Add near-zero-gravity buoyancy that decouples perceived body weight from gravitational load, and an immersive sensory field that narrows attention to the immediate perceptual environment, and the dive becomes a compulsory present-moment practice rather than an elective one. The Griffiths trial interprets this compulsion as a core mechanism: it reduces the cognitive bandwidth available for emotional reactivity while offering movement in a context that does not reinforce weight-based self-evaluation.
Not everyone has access to a scuba facility. The three mechanisms that appear to drive the effect, breath regulation, reduced sensory noise, and body-neutral movement, can each be approximated on land. Slow pranayama sequences such as 4-7-8 breathing or box breathing replicate the diaphragmatic emphasis that a regulator enforces underwater. Float tank therapy mirrors the buoyancy and sensory attenuation more closely than lap swimming can. Body-scan meditation directed toward functional sensation, specifically what the body feels rather than how it looks, targets the weight self-stigma pathway that the Montpellier cohort also improved.
The study's limitations are real: 55 participants is a modest sample, and the 87.3-percent female composition limits generalizability to broader populations. The authors call for replication in larger, more diverse cohorts. Still, the randomized design, significant effect size, and sustained gains across two-, five-, and eight-month measurement points make a straightforward case that psychosocial adjuncts blending experiential physical practice with structured mindfulness can accomplish measurable work in obesity management that standard dietary support alone does not.
Know something we missed? Have a correction or additional information?
Submit a Tip