Buddhist Mindfulness Training Boosts Executive Function and Well-Being in Young Adults
A Thai trial combining Buddhist chanting, movement, and breathwork hit effect sizes (d=1.05) nearly double the field's meta-analytic benchmark in healthy young adults.

Watcharaporn Daosang, Phrutthinun Surit, and Chanchira Wasuntarawat published an 8-week randomized trial in the journal Mindfulness on March 28 with a finding that quietly challenges the dominant image of the practice: the most effective mindfulness format in their study involved no silent sitting at all.
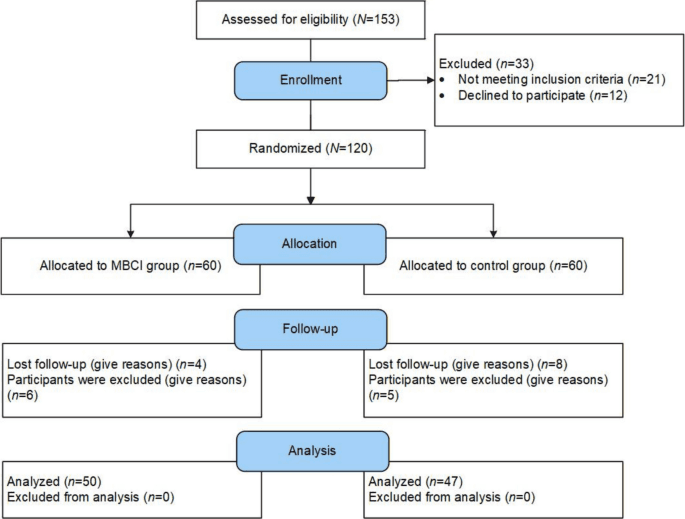
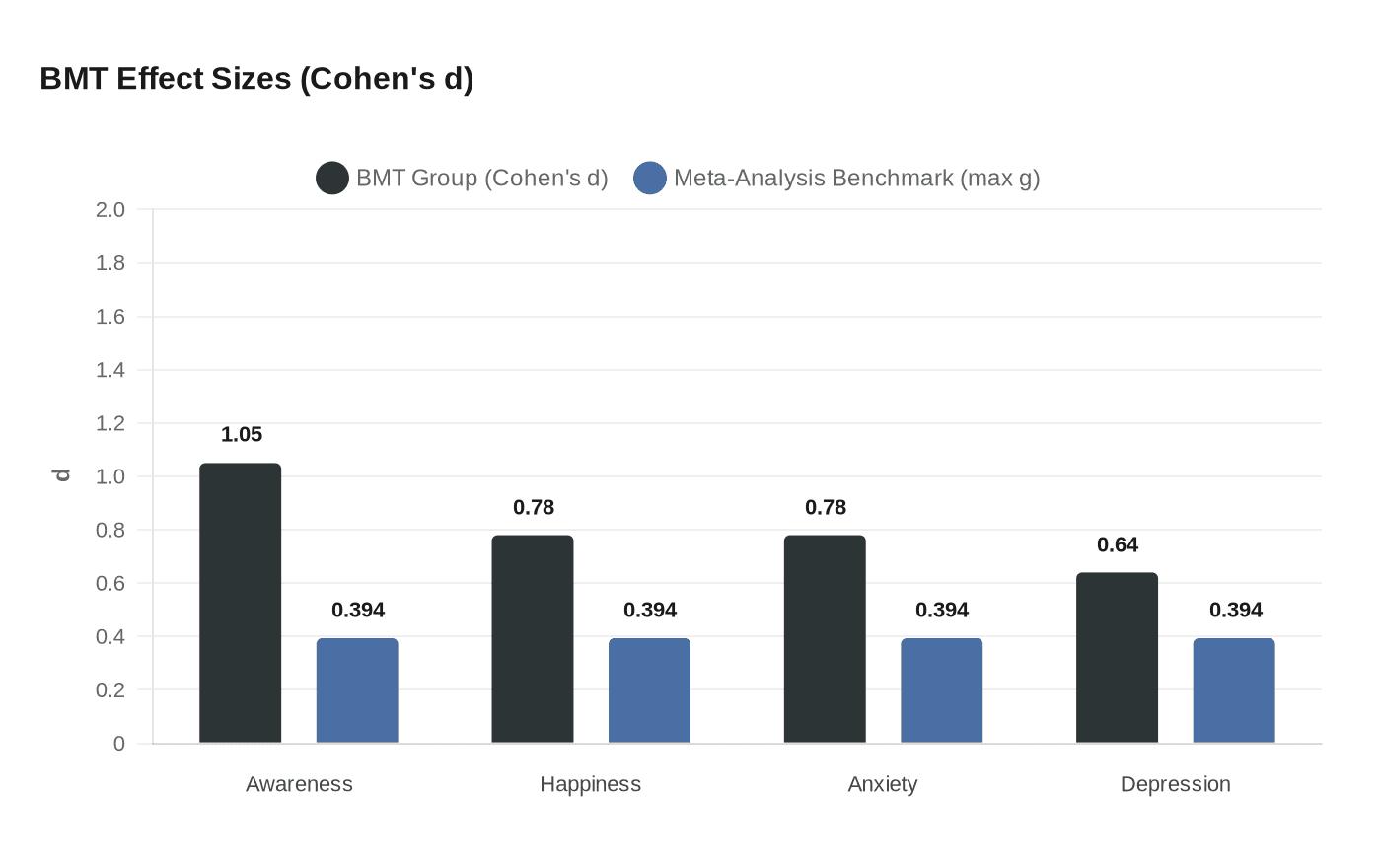
Their Buddhist Mindfulness Training protocol assigned 25 young adults to one hour daily of chanting, movement, and breathing meditation across eight weeks, with the other 25 serving as an active no-training control. When Daosang's team measured outcomes, the BMT participants showed large effect-size gains in awareness (Cohen's d = 1.05) and happiness (d = 0.78), with meaningful reductions in anxiety (d = 0.78) and depression (d = 0.64), all at p < .005. Those numbers sit well above the field's typical benchmarks: a 2023 meta-analysis of 111 randomized controlled trials enrolling 9,538 participants found that mindfulness-based interventions produced Hedges' g ranging from just 0.192 to 0.394 on executive function measures against active controls.
What a BMT session looks like matters here. Unlike Jon Kabat-Zinn's Mindfulness-Based Stress Reduction, developed in 1979 at the University of Massachusetts Medical School, which organizes eight weekly group sessions lasting 2.5 to 3 hours each around secular sitting meditation, body scan, and yoga, the BMT format breaks the work into daily one-hour blocks built around three rotating components. Chanting demands sustained phonological working memory and directed attention, the same cognitive resources that correlate with executive function capacity. Movement sequences require real-time inhibitory control to sequence postures and self-correct. Breath-focused meditation trains attentional shifting, the ability to redirect awareness from distraction back to target, which is directly tied to prefrontal regulation. Each element pulls on a different but overlapping executive network.
For practitioners who cannot commit to a full hour, 30 minutes daily is the realistic entry point, but the dose-response tradeoff is concrete: meta-analytic data on mindfulness interventions already show modest effects in healthy adults under standard conditions, and cutting the dose narrows that window further. If you scale down, prioritize frequency over duration. A 30-minute daily session held consistently across all seven days will outperform an hour-long session squeezed in three times a week; distributed practice builds skill more reliably than massed exposure.
One result broke from the psychological gains in ways worth noting. Heart rate variability, the autonomic marker most often cited as the physiological bridge between meditation and stress regulation, did not shift in the BMT group. A 2021 meta-analysis on vagally-mediated HRV and meditation-based interventions found mixed results across the broader literature, so the null finding is not an outlier. But it does leave an open question: if chanting, movement, and breathwork can produce large psychological and cognitive improvements without detectable changes in cardiac vagal tone, which physiological mechanisms are actually carrying those gains in the short term?
The study carries real limitations. Fifty participants is a modest sample, and the trial was retrospectively registered with the Thai Clinical Trials Registry rather than preregistered, meaning outcome measures were not locked in before data collection began. Meta-analytic evidence also shows MBI cognitive benefits are domain-specific: the 111-RCT review found no consistent improvement in verbal fluency, processing speed, or episodic memory, so the gains here should not be read as broad cognitive enhancement.
What the trial establishes is a replicable structure: one hour, eight weeks, three modalities, culturally grounded, face-to-face. Meta-analytic data consistently show that face-to-face delivery and non-standard formats are both associated with stronger treatment effects than self-guided or standard MBSR programs, which means the BMT format carries two structural advantages from the start. Whether those advantages hold at larger scale is the question the field should be testing next.
Know something we missed? Have a correction or additional information?
Submit a Tip