Compassion-Based Mindfulness Program Shows Promise for Adults with Type 1 Diabetes
A three-session compassion-based online group for adults with Type 1 diabetes showed early signs it can ease diabetes distress without adding much to an already crowded day.
What makes MindfulT1D different is how tightly it fits the realities of Type 1 diabetes. If your day is already chopped up by glucose checks, CGM alarms, food decisions, and the emotional whiplash of high and low readings, a generic relaxation class can feel out of touch fast. MindfulT1D, published online on April 22, 2026 in *Mindfulness*, was built for that exact lived experience: a brief, compassion-based online group program for adults with Type 1 diabetes, led by Molly L. Tanenbaum and colleagues.
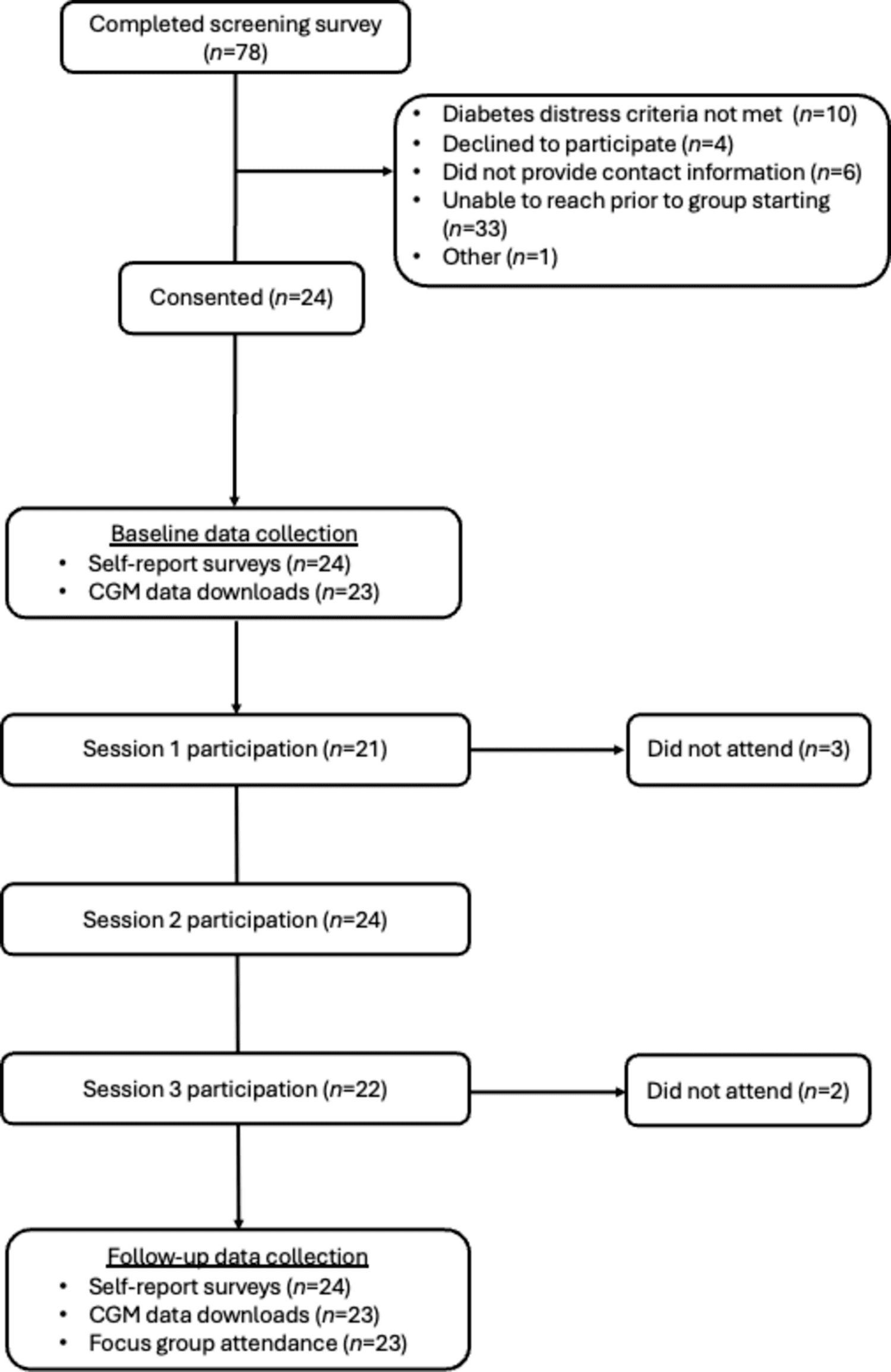
The study was a pilot and feasibility project, which matters because it asks a practical question before a bigger one: will people actually use this, and does the structure work? In this case, the answer appears promising. The intervention was a three-session online group workshop aimed at adult continuous glucose monitor users with Type 1 diabetes who were already showing elevated diabetes distress. The authors reported preliminary evidence that the program helped reduce that distress, and they signaled that the next step is to test it in broader groups, including people using multiple daily injections and those with lower time-in-range.
The key idea is that this was not mindfulness in the abstract. It was compassion-based mindfulness, which is a useful distinction if you live with a condition that punishes perfectionism. Traditional mindfulness often gets described as attention training, but the compassion piece adds a different flavor: noticing what is happening without immediately turning it into self-blame. For diabetes care, that can be the difference between “I failed again” and “this is hard, and I can respond to it without piling on shame.”
That design choice makes the program feel more clinically honest than a one-size-fits-all wellness offering. Type 1 diabetes is not just stressful in a vague way. It creates repeated moments of evaluation, correction, and uncertainty, often in public and often under time pressure. A small, remote group format that explicitly targets distress is a better match for that reality than a broad stress-management course that never mentions glucose data once.
The problem MindfulT1D is trying to address is not rare. Earlier research in adults with Type 1 diabetes found elevated diabetes distress in 42.1% of participants, and the 9-month incidence reached 54.4%. That is a lot of emotional load for a condition that already asks for relentless self-management. Distress in this setting is not a side note. It affects how people feel about the work of living with diabetes, and it can pile up even when numbers look “good” from the outside.

That is also why the study fits into a broader care conversation already taking shape in diabetes medicine. The American Diabetes Association has said psychosocial care should be integrated into collaborative, patient-centered medical care for people with diabetes. The Centers for Disease Control and Prevention makes a similar point in its diabetes-distress education materials, noting that as many as 1 in 3 adults with diabetes report negative emotions such as stress, guilt, anxiety, sadness, and anger tied to their condition, and pointing to mindfulness and meditation as practical strategies for increasing self-awareness.
The best practical takeaway from MindfulT1D is that the intervention was brief, online, and narrow enough to feel doable. That combination is the real story here. Three sessions is not a huge ask. An online group removes travel friction. Targeting CGM users with elevated distress makes the intervention feel specific rather than aspirational. For people already using mindfulness in their own practice, that is a useful model: keep the practice small enough that it survives the day.
A hobbyist meditator managing chronic illness could borrow several things from this approach right now:
- Keep the practice short and repeatable, not heroic.
- Pair awareness with self-compassion after a bad reading or alarm.
- Use your actual diabetes triggers, such as CGM alerts or correction decisions, as the cue to pause.
- Treat support as part of the practice, whether that is a group, a clinician, or a structured program.
- Aim for steadiness, not perfect calm.
That last point matters. Mindfulness for chronic illness is not about floating above the diagnosis. It is about making room for the emotional noise without letting it run the whole system. In that sense, the compassion-based framing feels especially well-suited to diabetes, where self-criticism can become its own burden.
MindfulT1D also makes more sense when you place it beside earlier work. Stanford Health Care lists a 2021 pilot in adults with Type 1 diabetes showing that a behavioral intervention for CGM users decreased diabetes distress and improved time in range. A 2022 doctoral thesis at Royal Holloway, University of London, explored an online mindfulness-based intervention for fear of hypoglycemia, well-being, and self-management behaviors in adults with Type 1 diabetes. Taken together, these projects show a field that is no longer treating mindfulness as a generic wellness add-on. It is being tested as a specific tool for specific diabetes problems.
That evolution is what makes the current study worth paying attention to. The field is moving toward interventions that match the cadence of real diabetes care, not idealized self-care. If a program can be brief, remote, compassion-based, and aimed directly at distress, it has a better shot at fitting into lives already crowded with medication decisions and sensor noise.
The larger shift is simple: mindfulness is becoming more practical. MindfulT1D suggests that the strongest version of this work may not be the most expansive one, but the most precise one. For adults with Type 1 diabetes, that means support that respects the emotional labor of daily management and gives people a way to meet it without adding another impossible standard. That is a small study with a big implication: the most useful mindfulness tools are the ones that fit into the mess of real life.
Know something we missed? Have a correction or additional information?
Submit a Tip