Mindfulness Program for Parents Cuts Obesity Risk in Young Children
A Yale mindfulness program for parents cut their toddlers' obesity risk sixfold compared to nutrition advice alone, a 12-week randomized trial found.

Teaching stressed parents to meditate may do more for a toddler's waistline than teaching them about vegetables. That's the striking takeaway from a Yale randomized trial published in Pediatrics, which found that a mindfulness-based stress management program for parents of overweight 2-to-5-year-olds protected those children from significant weight gain, while kids whose parents received only nutrition and exercise counseling faced a six-fold higher risk of overweight or obesity within three months of the program ending.
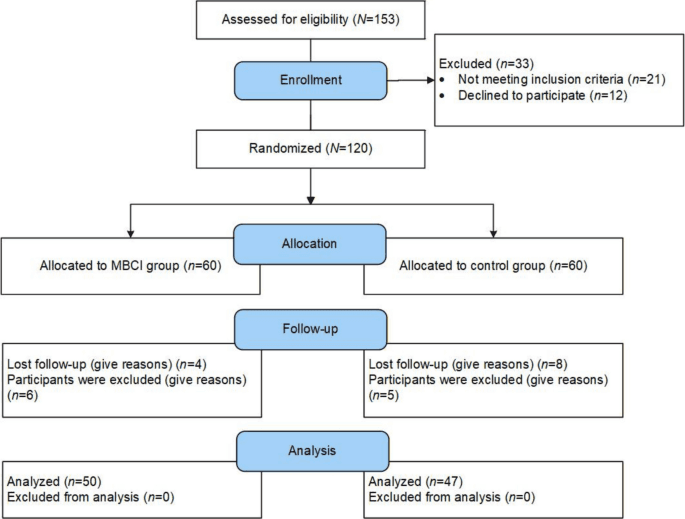
The study enrolled 114 parents from diverse ethnic and socioeconomic backgrounds, all of whom had children between two and five years old who were already overweight or obese. Researchers randomly assigned them to one of two groups. One group participated in Parenting Mindfully for Health (PMH), a 12-week program combining mindfulness techniques, behavioral self-regulation skills, and guidance on healthy eating and physical activity. The comparison group received counseling on nutrition and physical activity only. Both groups met weekly for sessions lasting up to two hours.
By the end of the trial, only the PMH group showed measurable reductions in parental stress. That same group also improved across specific parenting behaviors tracked by researchers: warmth, listening, patience, and positive emotional interactions with their children. Their kids consumed less unhealthy food and, critically, showed no significant weight gain at the three-month follow-up. The control group showed none of those improvements in stress or parenting.
"We already knew that stress can be a big contributor in the development of childhood obesity," said Rajita Sinha, director of the Yale Interdisciplinary Stress Center and the study's senior researcher. "The surprise was that when parents handled stress better, their parenting improved, and their young child's obesity risk went down."
The mechanism matters here for anyone in the mindfulness community thinking about why body-scan practice or breath awareness could ripple outward into a child's health. Prior research had flagged parental stress as a hidden driver of childhood obesity, with overwhelmed parents more likely to rely on fast food rather than structured meals. The PMH program specifically targeted that stress-behavior chain, pairing formal mindfulness practice with behavioral self-regulation strategies designed to interrupt reactive eating patterns in the household.

Sinha described the protective effect this way: "The combination of mindfulness with behavioral self-regulation to manage stress, integrated with healthy nutrition and physical activity, seemed to protect the young children from some of the negative effects of stress on weight gain."
The urgency behind the research is hard to miss. According to the U.S. Centers for Disease Control and Prevention, approximately one in five children and adolescents in the United States met the clinical definition of obesity in 2024. Standard prevention programs, which typically center on nutrition education and exercise, have frequently failed to produce lasting improvements, the researchers noted.
The Yale Interdisciplinary Stress Center, which Sinha directs, has operated as an interdisciplinary consortium since a 2007 National Institutes of Health Common Fund initiative established it to investigate the biological and behavioral effects of stress on chronic disease. This trial, authored by Nia Fogelman, Heather Bernstein, Tara Bautista, Mary Savoye, Tara M. Chaplin, Wendy K. Silverman, Ania M. Jastreboff, and Sinha, represents one of the most direct tests yet of whether parent-level stress reduction can move the needle on childhood obesity risk in the earliest, most formative years.
Know something we missed? Have a correction or additional information?
Submit a Tip