Mindfulness Training Eases Pain and Anxiety in Students With Dysmenorrhea
Eight weeks of mindfulness training cut both pain scores and state anxiety in 185 students with dysmenorrhea, a Turkish university RCT found.

A randomized controlled trial enrolling 185 undergraduate students at a Turkish university found that eight weeks of structured mindfulness training produced statistically significant reductions in menstrual pain and state anxiety compared with a control group, adding some of the most rigorous population-specific evidence yet that non-pharmacologic approaches can meaningfully address primary dysmenorrhea on campus.
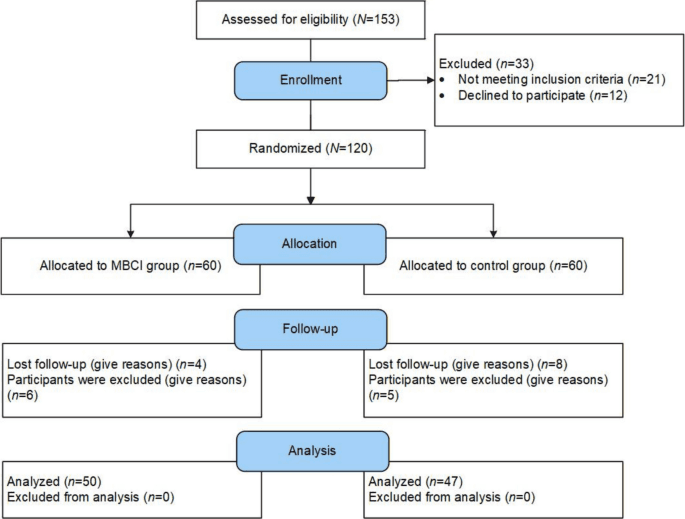
The trial, published in the European Journal of Integrative Medicine with an abstract indexed March 23, 2026, assigned 94 students to the mindfulness intervention and 91 to the control condition. The program consisted of weekly 120-minute mindfulness training sessions led by study personnel over eight weeks, followed by three months of encouraged independent practice. Researchers tracked outcomes using four validated instruments: a Visual Analog Scale for pain, the State-Trait Anxiety Inventory (STAI), a mindfulness scale, and the WHOQOL-BREF quality-of-life questionnaire.
By follow-up, the mindfulness group showed statistically significant drops in both VAS pain scores and state anxiety as measured by the STAI-TX I subscale. Self-reported mindfulness scores improved as well, and that increase mattered beyond the scale itself: higher mindfulness scores at follow-up were directly associated with lower pain and lower anxiety, suggesting the mechanism runs through the cultivation of moment-to-moment awareness rather than through distraction or placebo alone. Quality-of-life gains appeared across three WHOQOL-BREF subdomains, physiological, psychological, and environmental, while social domain scores were not reported as significantly changed. No intervention-related adverse events were recorded across the full sample.
For context, primary dysmenorrhea, painful menstrual cramps without an identifiable pelvic pathology, is among the most common conditions undermining academic functioning in student populations. NSAIDs and oral contraceptives remain the dominant clinical responses, but a meaningful share of students either prefer to avoid pharmacologic management or experience anxiety as a comorbid burden that medication alone does not address. The 8-week format here, structured group sessions with a gradual handoff to independent practice, maps onto what campus health and nursing programs can realistically deliver within a semester framework.
At 185 participants, the trial is notably larger than most prior pilot work in this space, and the randomized design strengthens the causal interpretation of the findings. The single-site limitation is real: the sample reflects one Turkish university's undergraduate population, and replication across different cultural contexts and multi-site designs would sharpen the generalizability claim. Still, the WHOQOL-BREF and STAI are internationally validated instruments, and the effect pattern, pain down, anxiety down, mindfulness up, held across all three measured quality-of-life domains.
Campus counseling centers and student health services looking to build out dysmenorrhea management beyond the prescription pad now have a well-powered RCT to cite when making the case for group mindfulness programming. The full article in the European Journal of Integrative Medicine contains the effect sizes, randomization procedures, and detailed methodology that practitioners will need before adapting the protocol for their own settings.
Know something we missed? Have a correction or additional information?
Submit a Tip